-
Welcome to Celiac.com!
You have found your celiac tribe! Join us and ask questions in our forum, share your story, and connect with others.
-
Celiac.com Sponsor (A1):
Celiac.com Sponsor (A1-M):
-
Get Celiac.com Updates:Support Celiac.com!
Search the Community
Showing results for tags 'abdominal pain'.
-
Constant low back, abdominal and pelvic pain!
Aussienae posted a topic in Coping with Celiac Disease
I have spent endless hours researching and reading this forum. Thank you everyone for sharing your stories! I was diagnosed in mid Feb 22 with positive blood. The hospital said to go gluten free asap as my levels were very high and did not need to be confirmed in biopsy. Im 3 months in and some things have cleared up, symptoms that I didnt even realise were related (sore feet and hands in the morning, dry mouth and eyes) but I have ongoing constant dull lower back and abdo pain, its so low its pretty much in my pelvis/groin (similar to menstrual pain) Weirdly its not there in morning when I get up but appears around mid day even if i dont eat. Its the same every day, although somedays it can be more painful to the point I take pain relief. I also have the feeling my bowel is full but I dont have C or D and am regular I take probiotics, digestive enzymes, B complex and magnesium. Ive had CT with contrast (last December) and more recently a pelvic ultrasound. Last blood test my Ferritin was slightly low and my CRP is always high. But all other tests normal, except for celiac of course. Any suggestions???- 60 replies
-
- abdominal pain
- celiac
-
(and 3 more)
Tagged with:
-
Hello, I just wanted to see if anyone else had similar symptoms during recovery. After dealing with severe abdominal pain for a couple of months, an endoscopy/biopsy confirmed I had Celiac. For the first few weeks going gluten free, I was generally feeling better. While I still had symptoms, they weren’t usually severe and my appetite was returning. I was finally able to sleep through the night and wasn’t bedridden the majority of the time. Fast forward to yesterday (6 weeks post-diagnosis) and I’ve been sick as a dog. I’m almost back to where I was pre-diagnosis: waves of nausea, heartburn, joint pain (especially in hips), restlessness, fatigue, loss of appetite, brain fog, and water just goes through me so I’m urinating frequently. I’m confused because I’ve been so careful about not eating out, cross contamination, and sticking to the gluten-free diet. I feel miserable! I haven’t been able to get out of bed most of the day. Anyone else get these debilitating episodes?? The only thing I can think of is eating Aussie Bites within the past couple of days. They’re labeled as gluten-free but they have oats and millet, so maybe I’m sensitive to that. And I just read that they were likely stored in a facility containing wheat 🙄. I also was having lactose almost daily until I cut it out a couple days ago after reading that it can irritate the intestines. So I’m wondering first how others have been able to recover from severe flare ups. But also is it normal to just have crazy, seemingly random flare ups throughout your recovery like this? I’m feeling really stressed and demotivated because this illness takes up so much of my time and mental space. I’m a graduate student and this has really interfered with my productivity. If it helps, my TTG was high at diagnosis (above 250) and there was a lot of villi damage. I was also tested for diabetes and got the full panel (CBC, kidney, etc.) at time of diagnosis and all came back negative. Glucose was fine. Had abdominal CT scan, which was also normal, and I’m waiting to hear back on follow up TTG + vitamin lab work results.
- 11 replies
-
- abdominal pain
- fatigue
-
(and 4 more)
Tagged with:
-
Celiac.com 07/02/2021 - Do you suffer from symptoms of abdominal pain, stomach aches, excess bloating, gas, diarrhea, fatigue, bone or joint pain, skin rashes, headaches, difficulty concentrating or irritability? Gluten, the major protein in wheat, barley and rye causes these symptoms in many people but most, including their physicians, are unaware that gluten is the cause and that a gluten-free diet may relieve these symptoms. Though there are diagnostic blood tests available for identifying gluten sensitivity, these test have limitations. Many physicians are unaware these blood tests are available, including genetic tests for the risk. Most physicians are also unaware of the broad manifestations of gluten sensitivity and fail to order tests that could diagnose the cause. Sadly, the condition often goes unrecognized and untreated when it is very common and reversible by simply following a gluten-free diet. No medications or surgery are required. Worldwide nearly 1 in 100 people have the most severe form of gluten sensitivity or intolerance known as Celiac disease though it is estimated that more than 90% are undiagnosed. Startlingly, many more than this, possibly 10-30% of people of northern European ancestry, have lesser forms of gluten sensitivity that causes symptoms that improve on a gluten free diet. The low carbohydrate diets have become popular because many have lost weight but they also frequently experienced dramatic improvements in general feeling of well being, increased energy, relief from fibromyalgia, joint aches, improved skin, fewer headaches, and improved digestive symptoms. However, many fail to gain full benefit because they don’t know they are gluten sensitive and have not completely eliminated gluten from their diet since gluten is present in so many foods that we eat. Gluten is insulinogenic, meaning it stimulates insulin release, and thereby promotes weight gain. Abnormal blood sugar regulation also often occurs. Some people will gain weight despite malabsorbing essential nutrients. It is now known that more than 10% of insulin dependent diabetics have celiac disease. What is not yet known is whether the celiac came first or the diabetes, but that they commonly occur together. Celiac disease is also commonly associated with other autoimmune conditions such as lupus, rheumatoid arthritis and thyroid problems. Celiac disease is a reversible cause of infertility, low birth weight infants, pre-term labor, and recurrent miscarriages. Untreated it is associated with a significantly increased risk of numerous cancers including all GI cancers and lymphoma. It is a common cause of unexplained anemia especially from iron deficiency and causes premature osteoporosis. Dietary elimination of gluten allows the intestine to heal so that absorption is normalized and symptoms are relieved. After five years of a gluten-free diet the cancer risk returns to normal as long as the individual remains gluten-free for life. Classic celiac disease is diagnosed by abnormal blood tests and an abnormal intestinal appearance on biopsy. Blood tests for celiac disease include antibody tests for gliadin (AGA), the toxic fraction of gluten; endomysial antibodies (EMA); and tissue transglutaminase antibody (tTG). High antibody levels to EMA and tTG are generally accepted as diagnostic for celiac disease though some individuals with celiac disease and most with lesser degrees of gluten sensitivity may have normal levels. AGA levels have, in the past, been considered very sensitive but not specific for celiac disease. Newer assays for AGA antibodies for gluten that has undergone a chemical change called deamidation that appears to be more specific for celiac disease (Gliadin II, Inova) may be as or more accurate than EMA and tTG antibody tests. However, lesser forms of gluten intolerance may be missed when any of these blood tests are normal or borderline and/or small intestine biopsy is normal or indeterminate. Stool antibody testing for antigliadin and tTG has been performed in research labs and published in a few studies. The commercial lab, Enterolab, now offers these tests though the former research gastroenterologist Dr. Ken Fine, who patented the test, has yet to publish the results of his findings in a peer reviewed journal. His unpublished data and the clinical experience of some of us who have used his test have indicated the tests are, to date, 100% sensitive for celiac disease. They are highly sensitive for gluten sensitivity of lesser degrees before blood tests or biopsies become abnormal but when symptoms exist. These symptoms reverse on a gluten-free diet instituted by those with abnormal stool antibody levels. Small intestine tissue obtained by biopsy during upper gastrointestinal endoscopy has been considered the “gold standard” for the diagnosis of celiac disease since the 1950s. However, recent studies have demonstrated that some people with gluten sensitivity, especially relatives of celiacs with few or no symptoms, may have changes from gluten injury in the intestine that can only be seen on a small intestine biopsy with special stains not routinely used, or on electron microscopy done in the research setting. Immunohistochemistry stains can detect increased numbers of specialized white blood cells called lymphocytes in the intestinal lining tips or villi as the earliest sign of gluten induced injury or irritation. Electron microscopy also reveals very early ultrastructural changes in some individuals when all other tests are normal. According to published research, when people are offered the option of gluten-free diet based on these abnormalities they have usually responded favorably, whereas those who continued to eat gluten often later developed classic celiac disease. What these studies suggest is that a “normal small intestine biopsy” may exclude celiac disease as defined by strict criteria but it does not exclude gluten sensitivity, a fact appreciated by many individuals who ultimately started a gluten-free diet based on their symptoms, family history, suggestive blood test or stool antibody test(s). Those few physicians who appreciate the concept of the spectrum of gluten intolerance or sensitivity are outnumbered by the medical majority that continues to insist on strict criteria for the diagnosis of celiac disease before recommending a gluten-free diet. Physicians either unfamiliar with the research on celiac or who are holding onto the strict criteria for celiac as the only indication for recommending a gluten free diet unfortunately often leave many gluten sensitive individuals confused or frustrated. Some seek answers on the Internet or from alternative practitioners. Many have their diagnosis missed, challenged, or dismissed. Others are misinformed or receive incomplete information. As a result many may fail to benefit from the health benefits of a gluten-free diet because they are advised that it is not required because they have normal blood tests and/or normal biopsies. Another source of confusion lies in the knowledge that certain genetic patterns are present in over 90% of individuals with celiac disease. Testing for such specific blood type patterns on white blood cells known as HLA DQ2 and DQ8 is increasingly employed to determine if a person carries the gene pattern predisposing to celiac disease. Some use the absence of these two patterns as a way of excluding the possibility of celiac disease and the need for testing or gluten-free diet. However, there are rare reports of classic Celiacs who are DQ2 and DQ8 negative. Moreover, recent studies indicate other DQ patterns may be associated with gluten sensitivity though very unlikely to predispose to classic celiac disease. Testing for all the DQ patterns has been advocated by Dr. Fine based on his experience with stool antibody testing that has revealed that the other DQ types are associated with elevated levels, symptoms, and positive response to gluten-free diet. According to his unpublished data, all the DQ types except DQ4 are associated with a risk of intolerance to gluten. Testing for the DQ types allows a person to determine if they carry one of the two high risk gene types for celiac disease or the other “minor” DQ type associated with gluten sensitivity but low risk for celiac disease. Enterolab also offers the stool testing for gliadin antibodies and tissue transglutaminase antibodies as well as several other stool tests for food intolerance or colitis. Though not widely accepted, these tests have gained favor with the lay public as an option for determining sensitivity to gluten or other food proteins, either despite negative blood tests and/or biopsies, or in place of the more invasive tests. Most recommend the accepted blood tests and small bowel biopsy for confirmation of celiac. The favorable reports in the lay community have been overwhelmingly positive though they can’t be subjected to peer review by the medical community prior to the publication of Dr. Fine’s data. Physicians open to the broader problem of gluten sensitivity are reporting these tests helpful in many patients suspected of gluten intolerance with negative blood tests and/or biopsies, though some are not certain how to interpret the tests. The national celiac organizations have difficulty commenting on their application without published research though a recent article in the British Medical Journal did show stool tests highly specific for celiac. Dr. Fine’s has publicly commented that his unpublished data demonstrates those with abnormal stool tests indicating gluten sensitivity overwhelmingly respond favorably to a gluten free diet with improvement of symptoms and general quality of life. There is no agreed-upon definition for gluten sensitivity or intolerance, especially for those who do not meet the strict criteria for celiac disease yet may have abnormal tests and/or symptoms that respond to gluten-free diet. Those individuals become confused when they realize that because they aren’t diagnosed with celiac disease, they don’t know where to turn for more information. Consensus in the medical community on definitions and more research in this area are greatly needed.
-
- abdominal pain
- bloating
-
(and 8 more)
Tagged with:
-

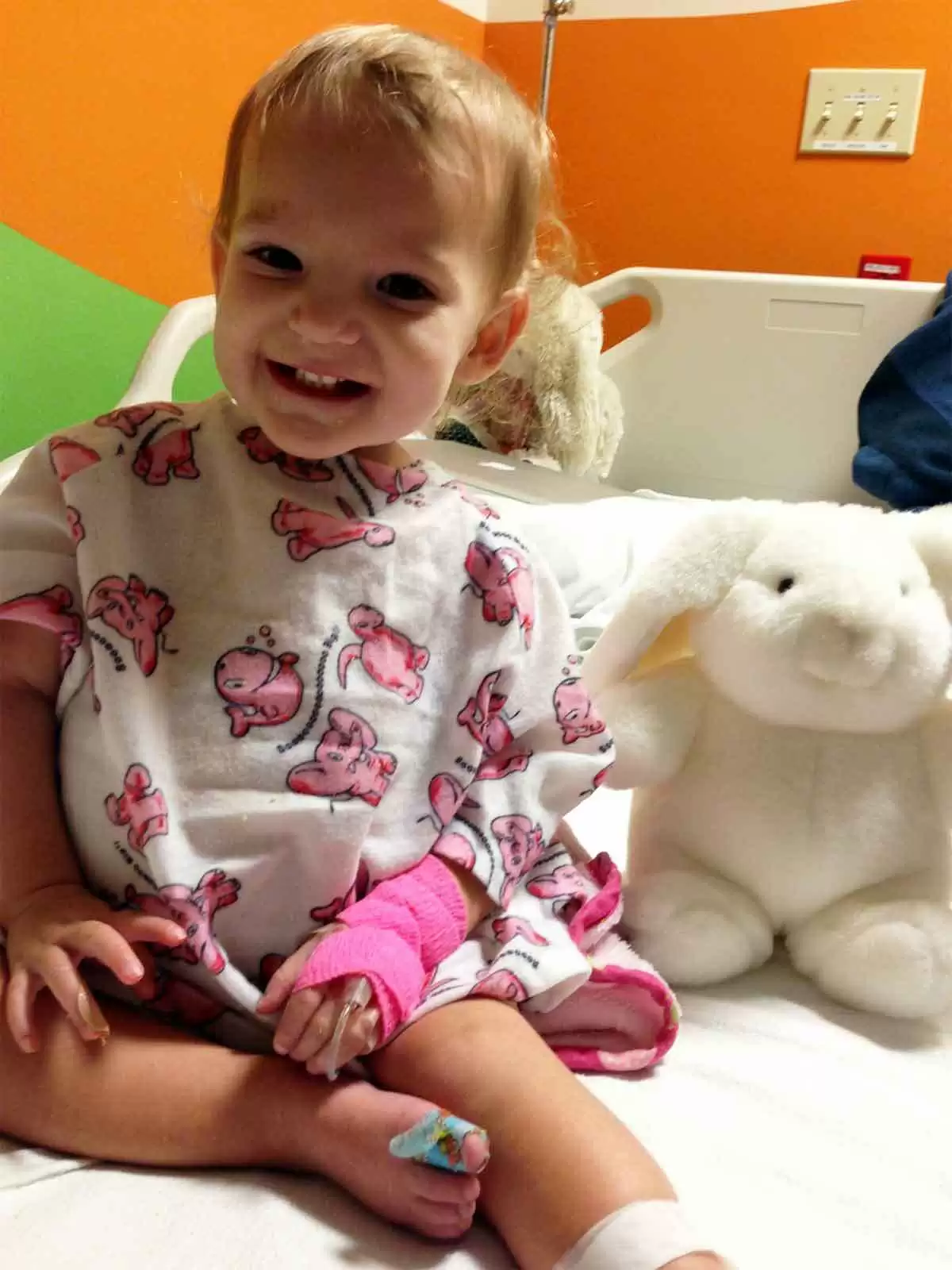
The Celiac Child: To the Brink of Death and Back Again
Reese Hogan posted an article in Winter 2021 Issue
Celiac.com 01/18/2021 - I remember the exact moment I first heard of celiac disease. I was sitting on a bed at the University of New Mexico Hospital, on the phone with my dad. My seventeen month-old daughter Mikaela lay listlessly in a metal crib across the room. Her limbs were emaciated and her belly swollen from starvation, after over a month of food had passed through her completely undigested. At least three weeks had passed since she'd last walked. By the time we'd landed here, at our third hospital, she just laid and stared, too weak to sit up or even cry anymore. Only the frequent blood draws and IV needles elicited any reaction from her now—heartbreaking screams I often had to leave the room for. It was at one of these blood draws earlier that evening that I first heard the word "celiac" uttered, passed between the technicians and barely caught by my exhausted ear. On the phone with my dad later, I mentioned that blood draw, mentioning it mostly because it had been such a bad one—they couldn't find a vein, it had taken forever, and it seemed like they'd taken a lot of blood. I must have mentioned the word "celiac," though, because my dad called me back not long after to tell me to look up celiac disease. And there on the internet, in neat bullet points, Mikaela's symptoms were listed to a tee. By the time a doctor came in to tell us the results the next day, we already knew what the news would be. But we didn't realize at the time that Mikaela was no ordinary celiac patient. The First Hospital We were only two weeks into 2013, with a healthy sixteen month-old daughter, when we saw the first sign that something was wrong. It was January 19th, Martin Luther King Jr. Day Weekend, and we were in the small town of Chama, New Mexico, for a local ski race. My stepmom, Mary Ann, is in charge of the event, and after the usual busy months preceding the ski race, my family and I had had a fun and relaxing day in the mountains participating in cross-country ski events and playing with our bundled-up baby daughter. Although Mikaela had a history of being a colicky baby, she had always had good energy and enthusiasm, and I remember this weekend being no different. After eating a spaghetti dinner that evening, my husband, Trever, picked Mikaela up and trotted her around the room in his arms. Mikaela laughed and laughed. And then she threw up. Afterward, she was in good spirits and clearly wasn't sick. My dad, Patrick, who has a medical degree, was sure it was related to the copious amounts of milk she'd drunk right before we'd left for dinner. Another family friend, who had a daughter three years older than Mikaela, told me these things happen to young kids, and oftentimes you never find out why. I was uncertain, but felt reassured. That night, however, Mikaela had an episode of diarrhea so bad that it made a mess of her pajamas and crib. It was pure liquid, and contained entire chunks of grapes, complete with the peels. I was freaked out, but again, Mikaela had eaten lots of grapes the evening before, and I figured that combined with her upset stomach from the milk, she was just having some sort of brief stomach bug. The three-hour drive back home was brutal. She had that same diarrhea at least twice more. And that night, she threw up again. Over the course of the next week, she threw up every night, usually in her crib, and continued to have diarrhea once or twice a day. And every time, there were undigested chunks of food. Because Mikaela had no fever and no other symptoms of illness, I was convinced her problems were due to something she'd eaten. I spoke with a friend who'd had a baby with acid reflux and other allergies. The symptoms sounded similar, so I decided to take Mikaela off of dairy products for a week and see if anything changed. The vomiting stopped, but the diarrhea didn't. It was at about this point, a week and a half after her first symptom, that she started losing energy. She was walking less, and I could tell she was losing weight. Still figuring it was a bad stomach bug, or something she had eaten that was disagreeing with her, I brought her to the doctor, expecting to be told she'd get better in a few days and maybe be sent home with a prescription. Instead, she was sent to the hospital with severe dehydration and low blood sugar (34). She had dropped almost a pound since her last weigh-in two months earlier, to 18 pounds. Once she was at the hospital and hooked up to an IV, she cheered up again. The hospital gave her a stuffed animal she loved, which we affectionately named Doctor Hops, and we saw her smile again for the first time in a week. The week before her first hospital stay, it had been increasingly hard to find foods Mikaela would eat. At 17 months old, she was learning that food was hurting her, and already becoming afraid to eat it. Ironically, and sadly, she was living almost exclusively on saltines and graham crackers—very high sources of gluten that were unknowingly just making her sicker. But with her weight loss and her increasingly sensitive stomach, Trever and I were just happy we could get her to eat anything at all. At the hospital, they had little cups of vanilla ice cream that Mikaela fell in love with. Because I figured Mikaela's problem had been dehydration and low blood sugar, I let her eat them. She continued to have diarrhea in the hospital, which the doctors assured me would clear up soon, but she didn't throw up again so I figured the ice cream was in the clear. I was wrong. Almost as soon as we arrived back at our house, two days later, she threw up again. Alarmed and scared, I called the hospital back right away. They thought she might still be having a reaction to dairy, and told me it was most likely a result of all the ice cream she had eaten. They told me to keep an eye on her and call my doctor back if it continued. After I hung up the phone, I saw that Mikaela was back in good spirits after Trever had cleaned her up, so I knelt down and held out my arms. Mikaela tried to walk toward me. She was still so weak she only managed about three steps before falling and hitting her head on the kitchen floor. It would be the last time I'd see her walk for over a month. The Second Hospital It was at this time, between the first and second hospital visits, that I found out I was pregnant with my second child. Trever and I had long been excited about giving Mikaela a little sibling, but right now, with our first child so sick, it was hard to even think about a new child growing while the other one declined. I remember going in for a blood test and telling the nurse that my daughter, sitting in her stroller, had been sick, saying it like it was an ordinary thing but knowing in my heart that it wasn't. Our chief focus the week after Mikaela's release from the hospital was making sure she drank enough that she wouldn't end up back there. Mikaela and I visited her pediatrician every other day, often spending over an hour waiting to be fit in around the normally-scheduled patients. Mikaela, completely uninterested in walking and growing steadily weaker, would sit listlessly in my lap. I spent our time taking selfies of us together, doing anything I could to wring a smile out of her again. In less than three weeks, I could see barely a shadow of the vibrant baby we'd raised. Her growth charts showed a decrease of weight from her regular visit two months earlier: she had dropped from 15th percentile to 2nd. But one thing alarmed her doctor even more. Neither her height nor her head circumference charts showed any growth for the last four months, since she'd been 13 months old. The doctor wanted Mikaela to see a neurologist for her walking and an endocrinologist for her growth. More than anything, I remember feeling intense frustration that the doctor was fixated on this growth issue when Mikaela was so sick. I just wanted her to be healthy again, and thought we could figure out the growth charts afterward. With everything going on, it never occurred to me that this was an abnormal or serious issue. At her appointment that Friday, her doctor decided we could no longer wait to send her to a neurologist, because for a baby to stop walking for this long meant something serious was going on. She sent her to a different hospital. A neurologist tested her reflexes and declared that nothing was wrong with her legs. A doctor took an x-ray of her belly, which was now noticeably swollen from her constant diarrhea, and told us Mikaela was very constipated. They did an enema. It was a miserable process, and there was no noticeable improvement afterward. The second day at the hospital, I brought her to the playroom, hoping to rekindle her interest in playing, and propped her standing at a play table. Then, as she became half-heartedly distracted by the toys, I backed slowly away to see if she'd remain standing on her own. She did, but it was less than a minute before she turned and saw that I'd moved. A look of fear flashed across her face, and her legs buckled beneath her. Whatever was going on with her, I knew it was far from "common." A doctor witnessed the event in the playroom, and Mikaela was taken for an ultrasound of her hips. There was some excess fluid in one of them. Mikaela was diagnosed with toxic synovitis—built-up fluid in the hips after a virus, which can sometimes affect walking. Reassured that they'd figured out what was wrong, the doctors told me it should clear up on its own within five days, possibly faster if we gave her infant Ibuprofen. Once again, Mikaela was sent back home. The Third Hospital Although the new diagnosis gave me hope at first, we saw absolutely no sign of improvement. In fact, Mikaela continued to get worse. She was painfully thin, with a protruding backbone and ribs. Her belly was so distended that she looked pregnant. Her cheekbones stood out sharply in her face. Her energy was nonexistent. She could no longer pull herself to a sitting position or grab my finger within her fist. She basically didn't move except when I carried her. For the first time, I began to fear she could actually die from this. But I felt the hospitals had done all their tests, and I didn't know what else they could do if I brought her back. I was torn apart by the terror and helplessness of the situation. Another thing that worried me was that we were on the cusp of a holiday weekend (President's Day), and I knew that it would be more difficult to get in and see her doctor if we had an emergency where she stopped breathing or something. I called my dad, who had visited the previous week and seen her condition. He felt as helpless as I did, but told me that after he ‘d related her story to a friend who'd lost a baby to SIDS, the friend had said, "That child needs to be in a hospital." I spoke to my best friend and she told me something that has stuck with me ever since: "You are her champion. You are the one who has to fight for her. You're all she has." When I hung up the phone, I knew what I had to do. I was going to bring her back to the hospital, this time on my own terms, and I wouldn't allow her to be discharged until we had a correct diagnosis and could see her health improving. It was 3:00 p.m. on Friday when I called her doctor's office and told them I needed to check my daughter back into the hospital. Her regular doctor was out of the office, but a different doctor called me back and said he'd sent Mikaela's info along to the UNM Hospital Pediatric ER, and to take her straight there. I showed up at the new hospital with Mikaela in my arms early Friday evening. Trever finally caught up with Mikaela and I in the ER waiting room, surrounded by the victims of that year's particularly bad flu season. Mikaela, too weak to fuss or cry, just lay in my arms amid the constant coughing and sneezing. Mikaela was checked in, and a couple doctors came to talk with us. I described the past three weeks as best I could. "I brought her to the doctor because she'd been having diarrhea for over a week. We kept seeing the doctor the week after her first hospital stay because she still wasn't walking." At one point, one of the doctors stopped me and said, "You can stop justifying everything, because this is all very unusual." The other doctor told us that we had finally come to the right hospital, because he said being a university hospital with actively studying interns, they got all the weird cases. The night that followed was a long one. Since the hospital was completely full from flu season, Mikaela and I were stuck into a space the size of a closet, with barely enough room to squeeze between her hospital crib and my bunk. In the middle of the night, one of the doctors from earlier returned with her growth charts, which he'd gotten from her records. He said, "I can't understand why either of those hospitals would have released her without addressing why her growth charts look like this." Mikaela was seventeen months old, but she'd basically stopped growing at twelve months. We were moved again in the early hours, to a curtained-off section of a room where a baby coughed horrendously the whole morning and I sat half-comatose in a chair next to Mikaela's crib. Occasionally, I'd pull Mikaela out of her crib to hold her, but she didn't react in any way. She dozed on and off, but it was hard to tell, because she didn't act any differently awake than when she was asleep. We tried to keep her hydrated and to feed her, but anything we gave her almost automatically came out again through her diaper. The next day, Mikaela was all over the hospital for testing. My mom had joined us, and tried to comfort me. My dad, who lives three hours away, kept calling to check on her and suggest tests to run and tell me what to say to the doctors. "Tell them she's starving to death," he said. At this point, sleepless and scared out of my mind, I heard an accusation in his tone that we had somehow caused this by not feeding her enough or feeding her the right things. It was an accusation that didn't exist—my dad was simply laying out the truth, and was as scared as I was—but I felt overwhelmed and sick from my pregnancy and couldn't deal with it anymore. I hung up the phone. I cried and cried. Mikaela went through two MRI's and a lumbar puncture. One thing they suspected was a brain tumor, and they also wanted to see if anything was wrong with her spine. Not only was the strength in her arms and legs gone, but she had absolutely no reflexes in her legs, which convinced the neurologists something was wrong with them. The tests found nothing wrong with Mikaela's brain or spine, but one doctor suspected a condition called Guillian-Barre, which can sometimes affect walking after a virus. But the tests weren't conclusive, and the symptoms didn't quite match up. My dad and stepmom joined us at the hospital. My dad was very apologetic, explaining that he never once meant her condition was due to anything we had done. I told my mom and dad about my pregnancy, and they and my husband helped out by accompanying Mikaela to the tests my pregnancy kept me from being present for. Over the next couple days, as test after test was run and Mikaela's IV's were changed out and unending blood tests were taken, Mikaela continued to get worse. Nurses would come in to weigh her every few hours. Her weight had dropped below 17 pounds, and we struggled to raise it again. Her magnesium, potassium, and folate levels were dangerously low. The diarrhea was constant. On our third day at the hospital, Mikaela puffed up like a balloon. The change was startling after her emaciated state. The doctor grimly told us it was a result of low albumin—a protein made by the liver. Albumin normally helps keep fluid in the bloodstream and out of other tissues, but in cases of severe malnutrition, like Mikaela's, the fluid escapes the blood and causes the body to swell. Mikaela's body had used up all its glycogen, all its fat, all its stored protein and its muscles. I didn't know it at the time, but this intense swelling is one of the last stages of starvation. On our fourth or fifth night there, with Mikaela barely clinging to consciousness, a team of techs came in and took one of their longest blood draws yet. They took blood at all hours, and part of me just wanted Mikaela to get some rest, but I was also afraid every time she closed her eyes that she wouldn't open them again. This blood test was so disruptive and late in the evening that I felt the need to recount it over the phone to my dad, somehow passing along that barely-snatched word I'd heard during the cacophony: celiac. It wasn't long after that he called me back and told me I needed to look up celiac disease. So I did. And it wasn't like toxic synovitis or Guillian-Barre, where it was a stretch to make the symptoms match. I knew instantly what I was looking at. I was looking at Mikaela. The Diagnosis Any Google search will show you what I found. Chronic diarrhea. Abdominal pain. Vomiting. Bloating. Fatigue. Decreased appetite. Weight loss. Failure to thrive. By the time a pediatric gastroenterologist came in the next morning, my whole family was waiting, sure we knew what the news would be. It was almost the first thing out of the doctor's mouth: "I think she has celiac disease." The blood tests not only confirmed the diagnosis, but hinted at how severe her case was. Non-celiacs have only a small amount of antibodies called tissue transglutaminase (or tTG's) floating around in their blood—usually at a level of below 20. Mikaela's tTG level was somewhere over 250—off the measurable charts. In a person with celiac disease, the body turns gluten into a protein that attacks the small intestine. Mikaela had stopped growing at the age of 13 months, shortly after she quit breastfeeding and was introduced to gluten for the first time. Amazingly enough, she didn't drastically start to decline for another two and a half months, when her lack of nutrients finally caught up to her and started shutting her systems down. When the pediatric gastroenterologist took a biopsy of her small intestine, he found that the villi inside lay completely flat, no longer able to catch and digest food. Not only did Mikaela undoubtedly have celiac disease, she was at the end of the spectrum for the most severe cases. She was taken off gluten immediately, and the doctors worked on getting all of her vitamins and nutrients back up. We knew it might take a while to start seeing improvements. But we were shocked. Within 24 hours of being off gluten, Mikaela was making eye contact again. Within three days, she had already regained enough strength to pull herself to sitting. I remember the first time we saw her smile after a month of listlessness. One of the nurses had a light-up dinosaur on her lanyard, and Mikaela reached out for it with a tentative smile. It was the most beautiful thing I'd ever seen. She was showing interest in the world again. And four days after her diagnosis, Mikaela took a couple shaky steps across the hospital playroom on legs so skinny, they didn't seem capable of supporting weight. Our daughter was coming back to us. Mikaela was discharged from UNM Hospital after just over two weeks. Although she still suffered from diarrhea and low weight, she was walking again, smiling again, and in improving health. Trever and I were certain she would fully recover within the next few months on the right diet. It was true we wouldn't face the same level of decline that had almost killed her at 17 months. But Mikaela would face unexpected complications with her celiac disease over not just the coming few weeks…but the next several years. The Aftermath That summer was a rocky one, in terms of her health. Mikaela remained dairy-free for the next several weeks. Her baby brother grew bigger in my womb. We sold our house and lived with my mom for a month and a half as we waited on our new house to pass inspections. We're not completely sure to this day, but we think Mikaela ate a piece of cat food (which is very high in gluten) around the time we moved in. For the next month, we fought diarrhea so bad it threatened to put her back in the hospital. But she still had frequent doctor's appointments, and through careful monitoring and hydration, we managed to keep her healthy enough. She regularly saw a developmental counselor, who helped her get back on track after her delay. She still hadn't started growing again, and her belly was still very distended. On the plus side, her tTG's were on the charts by July—from greater than 250 to 167. Another antibody that had tested very high at the time of diagnosis—deamidated gliadin antibodies, or IgA's—had fallen from 60 all the way to <.2. This number, at least, read perfectly normal now, and was a pretty clear indicator that we were successfully keeping gluten out of her body. By September, when she turned two, her growth charts had finally started showing improvement in her height as well as her weight. She was also able to tolerate dairy again, and her diarrhea was under control. Her little brother Alexander was born in October. After our scare that spring, we felt truly lucky to have two healthy children in our lives. But when she took her blood test a month later, we were shocked to find out that her tTg antibodies had gone up again—all the way back off the charts. Her doctor was puzzled, but Mikaela was healthy and her diarrhea was gone, so he chalked it up to the fact that sometimes those numbers take a long time to normalize. Only a few months later, he left UNM Hospital, never realizing that Mikaela was going to be a unique case. We were delayed by the position being refilled, and waited to see if Mikaela's blood work would come down on its own. But a year later, the tTg's were still off the charts, even though her iGa's remained promisingly low. Her stomach was still distended, and by this time, we'd passed it off to a body type issue and hardly noticed it anymore. In April 2015, the new doctor, a pediatric gastroenterologist from England, decided to take another endoscopic biopsy to see if the inside of her small intestine was showing improvement. The results weren't as good as we'd hoped. After almost two years on a gluten-free diet, the villi in her small intestine had gone from severe blunting to moderate blunting. It was clear that a normal gluten-free diet wasn't sufficiently healing her. The doctor brought up a possible diagnosis of refractory celiac disease. This is a rare form of celiac that is resistant to a regular gluten-free diet. 1% of the population is said to have been affected by celiac, and refractory celiac disease only affects about 1% of those diagnosed. Not only was this strain of the disease rare, but it's virtually unheard of in children. It can also be a very dangerous diagnosis; there are two types of RCD, and one of the types leads to cancer. Fortunately, Mikaela's bloodwork suggested that even if she did have RCD, she wasn't likely to have the second type. However, even the doctor doubted this diagnosis, because patients who suffer from RCD are in poor health and have trouble keeping their weight up. Mikaela clearly didn't fit this profile. Even though Mikaela was healthy on the outside, the doctor was concerned that leaving her small intestine that damaged could cause her health problems later in life, and even increase her risk of cancer. She wanted to start her on a steroid that would suppress her immune system and allow her gut to heal. I was very reluctant to put my healthy three year-old daughter on steroids, and suggested we cut back her diet to eliminate even the slightest chance of gluten cross-contamination. The doctor agreed it was worth a shot, so Trever and I proceeded to cut all processed foods out of Mikaela's diet. This meant grinding our own flour out of rice at home, making oatmeal from nuts instead of oats, buying only uncured meats, and no longer purchasing foods with more than four ingredients, to name just a few changes. It wasn't an easy diet to adjust to, but with the help of paleo cookbooks and my dad's excellent cooking skills, we were able to find a variety of recipes and foods for our family. We were fortunate that Mikaela was a non-picky eater, and adjusted to these dietary changes with no fuss. Outwardly, we saw no changes; she appeared to be a strong and healthy young girl with a big tummy and a vivacious attitude. After six months on her new and stricter diet, Mikaela's tTg levels were still off the charts, and she was put on iron for perpetually low ferritin levels. The doctor decided to give her another half-year to show improvement, but when labs were taken again in May 2016 and her levels remained the same, she put Mikaela on a six-month stint of corticosteroids called Budesonide. As I'd dreaded, she became aggressive toward her younger brother, and more disagreeable with us. She was constantly hungry and started retaining water, which made her body and face appear puffy and bloated. I hated the steroids just as much as I'd feared. They did succeed in reducing the tTG antibodies, but it was slow and painful progress. After three months, they were down from over 250 to 208, then at six months, they were at 161. It had taken six months of steroids to get them as low as they'd gotten on their own shortly after her diagnosis, before they had climbed again. So what had changed? Another biopsy was done in December 2016. There was improvement over the one from April 2014, with only mild villous blunting now. With her prescription for Budesonide done, the doctor decided to see if she'd continue improving without the steroids. But sadly, by August of 2017, the tTG numbers had soared off the charts again. I was really upset by the news, sure this meant the doctor would see that steroids were the only thing that worked and put Mikaela back on them. It was at this time that UNM Hospital hired a gastroenterologist who specialized in celiac disease. At our first appointment with him, he took one look at Mikaela and said there was no way she needed to be on steroids. She was entirely too healthy. Unconcerned, he spent another year monitoring her bloodwork then decided to schedule another biopsy to see how things looked. It was clear that despite her high numbers, he expected to find nothing wrong based on her great outward health. But this was not the case. Her small intestine still had villous blunting. When he called to tell me the results, he asked some questions about her diet, especially now that she'd started kindergarten. But I could tell in his voice that he didn't think the answers lay there, since she'd struggled with this for over four years now. My doctor called me back a few weeks later to say he'd met with another celiac expert from the University of Chicago, named Dr. Guandalini. Reassuringly, this doctor had met other rare patients like Mikaela—asymptomatic on the outside, but not fully healing on the inside. He told my doctor that a dairy-free diet had helped in these cases. So we decided it was worth a shot. As with every other step we'd taken, we didn't expect to see any differences outwardly. But I noticed, quite by surprise a couple months after starting the diet, that the distended belly she'd had since her diagnosis at 17 months was gone. The first thing I thought was that it was due to her taekwondo or other physical activity. But Mikaela has always been an active child, ever since she felt good again, and the difference in just two months was dramatic. Until that point, I'd never even considered that her stomach was related to her celiac disease, or thought much about it at all beyond thinking it was just the way she looked. A month later, she went in for another blood test. I was optimistic that the outward change would mean her tTG's would be below 250 again—maybe even as low as they'd been on steroids, in the 160 range, even though it had only been three months. When I called the nurse, the first thing she said was, "Her tTG levels seem to be elevated. Has she been exposed to gluten?" I said, "How high are they?" She said, "49." I almost dropped the phone. Her antibodies had fallen by over 200 in three months! At long last, we finally knew why her numbers had dipped briefly in the aftermath of her diagnosis before climbing back up again—it was because we'd reintroduced her to dairy. Either because of the destruction in her gut from the gluten, or because it was something else she'd been born with, this intolerance to dairy had been keeping her tTG levels extremely high and keeping her from fully healing. Mikaela has been gluten-free for seven years now and dairy-free for two and a half years. She is healthy and thriving, and rarely has stomach issues at all anymore. She had another endoscopy just last month, and everything came out perfectly normal for the first time in her life. The diagnosis of Celiac disease saved her life, and I will forever be grateful to the doctors at the University of New Mexico Hospital who figured it out in the nick of time. Mikaela lives a full life now, thanks to everything we've learned since that day back in 2013.- 15 comments
-
- abdominal pain
- celiac disease
-
(and 6 more)
Tagged with:
-
Celiac.com 10/19/2020 - A team of researchers recently set out to determine the rates of functional abdominal pain disorders (FAPDs) and functional constipation in children with celiac disease on a strict gluten free diet. The research team included Fernanda Cristofori, MD; Mariaelena Tripaldi, MD; Giusi Lorusso, MD; Flavia Indrio, MD; Vincenzo Rutigliano, MD PhD; Domenico Piscitelli, MD; Stefania Castellaneta, MD; Vincenzo Bentivoglio, MD; and Ruggiero Francavilla, MD, PhD. They are variously affiliated with the Interdisciplinary Department of Medicine-Paediatric Section, University of Bari, Italy; the Department of Paediatrics San Paolo Hospital, Bari, Italy; Section of Pathology, Department of Emergency and Organ Transplantation, University of Bari, Italy; the San Giacomo Hospital, Monopoli (BA), Italy; the Faculty of Medicine, Paediatrics Specialization School University of Padua; and the “B. Trambusti” Department Giovanni XXIII Hospital- Via Amendola 207 Bari, Italy. For their prospective study, the team looked at 154 males and 263 women at a tertiary care center in Italy from 2016 through 2018. All patients were diagnosed with celiac disease according to ESPGHAN criteria, followed a strict gluten-free diet for more than 1 year, and also had negative results from serologic tests. Patients with celiac disease had higher rates of FAPDs, at 11.5%, compared to 6.7% for control subjects, while the relative risk was nearly 2%. Nearly 20% of celiac patients had functional constipation (functional constipation), and more than 7% had irritable bowel syndrome (IBS), defined by the Rome IV criteria, compared with more than 10% and 3.2% respectively for control subjects. Parents and children over 10 years old answered questions about pediatric gastrointestinal symptoms, according Rome IV criteria. As a control group, the team used 145 male and 227 female siblings or cousins, who had negative results from serologic test for celiac disease. People with celiac disease face an increased risk of both IBS and functional constipation. The team stresses the importance of strategies for managing IBS and functional constipation in celiac patients. Read more in CGHjournal.com
- 4 comments
-
- abdominal
- abdominal pain
- (and 7 more)
-
I need help understanding this because my doctors are no help. Why would my Gastro Dr. not tell me about Gluten free diet? My son is actually the one who told me that I may have a sensitivity after seeing me in pain everyday and feeling like I cannot eat....and he's not a Dr.! I am hoping to have people reach out because I am at my wits end!
- 2 replies
-
- abdominal pain
- abdominal pressure
-
(and 3 more)
Tagged with:
-
Celiac.com 04/26/2017 - "The universe is made of stories, not atoms" — Muriel Rukeyser Helen, a woman with severe lifelong eczema/dermatitis, wrote to me a few weeks ago, saying "I have taken your advice and been strictly gluten free for five months now. The eczema inflammation is 99% gone and my skin quality has significantly improved. I do still get a bit itchy around my neck area and elbow creases, more so at night when it is warm. I have noticed a significant improvement in my asthma also. I still use antihistamines perhaps once or twice a week for runny nose. Does this mean I will need to be gluten free for life? Which of your books would you say would be the most relevant for someone in my position? Thank you for your assistance, regards, Helen. I recommended eBook: "Dermatitis Eczema: Gluten Wheat – Solving the eczema puzzle." Available at: http://www.GlutenEczema.com This is an excerpt from the chapter: "Children better off gluten/wheat". To help you get a better idea of how gluten can trigger eczema, here are narratives of some children whose eczema got better when their gluten sensitivity was recognised and treated. Most had good remission of their eczema on a gluten-free diet. Their stories told by their parents. To give context to the blood test values, the normal reference ranges were: AGA: 0–15 tTG: 0–20 Celiac disease with bad eczema Lily at five years old was diagnosed by me with celiac disease. Symptoms: eczema. Run down, pot tummy and slow growth. Tests: All of her blood tests were positive for celiac disease (tTG 120) and she had an abnormal intestinal biopsy which confirmed the bowel damage of celiac disease. AGA very high (115). Her mum said: "Lily has now been gluten-free for the last year. She came to see Dr. Ford to investigate her allergies. She had a blocked nose and troublesome eczema. She also had quite a pot tummy and Dr Ford said that her growth was slow (she was thin and short). Dr Ford said that she needed blood tests for gluten and celiac disease: these were both positive. So she had an endoscopy, which was abnormal, showing the villus blunting of celiac disease. Therefore, she had to go on a gluten-free diet." "Since she has been gluten-free over the last year, she has gotten better and better. She no longer has lots of infections, she has more energy, and interestingly, her allergies have nearly gone away. Her skin used to give her a lot of trouble – she had a lot of bad eczema. Her eczema now is very much better and she only has small amounts left in her creases. And if she has any gluten errors it flares up." Recovering from gluten-eczema Isabella, at two years old, was recovering from her eczema. I asked her mother what happens if Isabella has any gluten. Her mum said: "Isabella had eczema all over her body. She was on strong steroid creams. She had the positive blood tests for gluten antibodies (AGA of 66), so it was suggested I take her off the gluten. I did this." "I took her off gluten and it has cleared her eczema up. Now, when she does eat anything with gluten in it she gets little patches of eczema on her legs. I just can't believe it!" Blood all over her sheets Emily was three years old. She had a high anti-gliadin antibodies (AGA 48) but she did not have celiac disease (normal tTG). Her mother told me: "Initially her skin was really sore, dry and scratchy. She would have blood all over her sheets in the morning from scratching while she was asleep. Her poos were really sloppy and nasty." "But after taking gluten out of her diet her skin cleared up within days, and the itchiness of her skin settled. She was just so much happier." Dry skin and worsening eczema Breanna and Alyssa, twins aged 3 years. Symptoms: eczema and poor sleeping. Both had high AGA levels (60 & 68) and normal tTG levels (5 & 3). They did not warrant an endoscopy. Mum writes: "My twins were born at 26 weeks. During our stay in NICU they developed very dry skin, at times you felt like you wanted to peel the dry skin off. The word eczema was mentioned on more than one occasion. There is a history of eczema and asthma in our family, so at the time I tried to deny all knowledge of that word." Dry skin and worsening eczema "Eleven weeks later we took our twins home. Their skin was still dry and we were given a moisturiser to use as required. As time went on their skin didn't improve and eventually at around the age of one year they showed real signs of eczema. We started to use steroid creams: 1% Hydrocortisone to start with, then onto a much stronger steroid cream. Soon, this stronger cream was used all the time to control their eczema as the other creams were of no real help." "At around 2 years old, while at a playgroup session one of the mothers was talking about her daughter's eczema and how she had gone to see Dr Ford and now there were no signs of it there today. Of course my ears pricked up. I was interested to hear how her diet affected her skin and the word gluten was mentioned." At the time it didn't mean a lot to me. Therefore, I made an appointment and I was excited to think that we might be able to change the girls' diet and their skin condition may improve. They had positive gluten blood tests "The day arrived and we had our first visit. He talked to us about this gluten thing and that if we could avoid it then their skin might make a dramatic improvement. I was keen to try anything. Firstly, they had to have some skin prick allergy tests – it showed a reaction to wheat among a few other things. Next, the girls had a blood test confirming that they definitely had an allergy to gluten, and their iron levels were also very low. The final step was to set about changing their diet. I can honestly say that this was daunting to start with but once we got our heads around the issues, it became second nature." Sleeping at last! "One of the biggest changes we have noticed is that they are now sleeping so much better. I was constantly up and down to them all night and was getting so worn out now we can almost guarantee a full nights sleep, Yahoo!! The other major issue was the steroid cream use: we haven't used the strong steroid cream for 12 months. So for me, going gluten-free was a huge step in the right direction." Gluten-free gets easier "There are heaps of products that we can use and the staff in shops were very helpful with information and getting stock in. I have since brought a number of cook books all with sections on gluten-free that have been helpful. When baking or cooking, I now just do it the gluten-free way and everyone in our family eats it with no complaints. We have all adjusted accordingly." "Our thanks goes out to Dr Ford for all his help. I also send good luck to all of you who are about to embark on a gluten-free diet – the rewards will be well worth the sacrifice." Sharon Losing her hair – alopecia Ella, age 6 years. Symptoms: eczema, alopecia, moody, abdominal pain, multiple food allergy. AGA high (49), tTG normal (3), EMA negative, Small bowel biopsy, normal. Mum writes: "Ella is now age 6 years. At age 3 years Ella started to lose her hair. After a year of scalp treatment, by the time she turned 5 years old, all but one small patch had regrown." Losing her hair "About 4 months later a small patch of alopecia reappeared and her hair loss rapidly progressed from there. At this time her eczema, always present in a mild form, worsened and became almost impossible to control. Many forms of treatment were tried and all failed. Within the year Ella had lost all her hair and was constantly itching. Over this time Ella also complained of tummy pains and weight loss." Diagnosed as gluten-sensitive "As her father has celiac disease, we decided to get Ella checked. Her blood test was positive but the biopsy was negative for celiac disease. In discussion with the GP and some unanswered questions we eventually had an appointment with Dr Ford. After this appointment, Ella started on a strict gluten-free diet and has remained on it for the past 4 months." Amazing results "The results are amazing. Ella has stopped most of her scratching and she is far more comfortable. Ella's mood has changed and she is now a very happy little girl. Best news of all is that she has started to have a small amount of hair growth." "At no time, despite the variety of people seen and the fact that they were aware of family history, did anyone suggest getting Ella tested for celiac disease. It was purely parents at the end of their tether, pushing." Sue She was getting worse eczema Tessa, age 2 years. Symptoms: eczema, poor growth, multiple food allergy. Tests: AGA high (51), tTG normal (7), Biopsy not done. Mum writes: "Tessa was our first-born baby. She weighed a healthy 8lb and was breastfed until 6 months. I introduced solids at 5 months. Having given a bottle of expressed milk every night since she was 10 weeks, I found that she preferred this and weaned herself." Eczema at the time of solids "Tessa had eczema from the time she commenced solids, but it was manageable with mild steroid ointments. However, at six months her eczema became more distressing for her. She had her first course of antibiotics at this age." "We felt that we were using more and more topical steroids, oral antibiotics, and even a course of oral prednisone. None of these treatments felt satisfactory to her family. We needed a solution to prevent the problem. Not only was her skin getting worse but also she was quietly losing weight. A friend suggested visiting Dr Rodney Ford." Allergies to egg, dairy and peanuts "Our first visit involved an extensive medical history and allergy testing. Tessa was found to be allergic to egg, dairy, peanut, grass, and cats. We excluded the food allergens from her diet. But, over the next four months Tessa had a dramatic weight loss, going from the 50 percentile to falling off the Child Health nurse growth graph. She required more steroids, and antibiotics." Waking screaming "My angel baby, who had slept through the night from age 6 weeks, was now 16 months and woke every night screaming inconsolably. We were getting desperate, putting in an awful lot of work by eliminating dairy and egg with no rewards. With a new baby due to be born Tessa's exhausted parents needed answers. Back to Dr Ford we went. He suggested running some blood tests to check her gluten markers. It came back that her Anti-Gliadin Antibody was 51, suggesting that she was gluten-sensitive." Gluten-free as well! "We trailed a gluten-free, egg-free, and dairy-free diet. This was a totally overwhelming prospect for our family, as at that time we were introducing a two-week-old baby to the world! Luckily, Tessa's father, who too is an adult sufferer of eczema, was able to take all this on board and went off grocery shopping, bringing back lots of acceptable goodies. It was also at this time that I learnt of the real benefits of living in a small town." We had a gluten-free buddy "We were very fortunate that another mother of gluten-sensitive children took me by the hand grocery shopping, showing me how easy it is! Also, the church where we regularly attend made a whole week's worth of meals for the freezer which all fitted the requirements for Tessa's diet. All this really just through word of mouth!" At last she is better "We are so excited to see such an improvement. She has just been allergy tested again and we are able to introduce egg and dairy again. I had been giving small amounts of dairy already, hoping that she would have grown out of this. At one point all she would eat was cheese, so to get some calories into her that is what we fed her. Having Tessa on a gluten-free diet requires us to be organized and creative. It is especially difficult when you spontaneously decide to go out for the day: there are no guarantees that we will find appropriate food for Tessa, so usually we pack a lunch." Gluten-free is expensive "The food that is gluten-free is also usually twice the price of other foods. We have had to learn to bake, which is something I still struggle with. We have had some major disasters, especially baking cakes. Whenever it seems too difficult, and we are out of ideas, it is not too hard to find a reason to keep trying." Improved gluten free "Our little girl has significantly improved since becoming gluten-free. She has not required antibiotics or oral steroids for eczema since commencing the diet. We can now apply the topical steroid ointments as prescribed "sparingly". She no longer gets up in the morning, her pyjamas and sheets covered in blood, and forehead weeping. She can play in sandpits without fear that the sand will get into her sores, and once again they will be infected." "We are so lucky that something so simple as changing Tessa's diet has had such a dramatic affect on her life." Mum Think about the gluten-eczema link As you have been told by these families, gluten has been found to be an important trigger for eczema in these children. My research findings show that the majority of people over three years of age, who have ongoing and troublesome eczema, have gluten-sensitivity. When gluten is removed from their diets, they get better. Advice about blood testing for gluten and for information on a gluten-free diet can be found on our webpage: http://www.DrRodneyFord.com and in the previous chapters. This is an excerpt from Dr Rodney Ford's eBook, "Dermatitis Eczema: Gluten Wheat – Solving the eczema puzzle" Available at: http://www.GlutenEczema.com Written in the spirit of cooperation and knowledge sharing. See Part 1: Cutaneous Gluten Sensitivity
-
- abdominal pain
- alopecia
- (and 7 more)
-
Hi, I have some questions that I hope to get some answers to. First of all, I am not diagnosed and have not been tested for celiac. Only bloodtest I have taken that's relevant is Ferritin and Iron. I'm not anemic, but both my levels are on the lower range of normal (Ferritin 20-25 and Iron 9 and Iron binding capacity a bit over the normal range). My first question is if this is normal in celiacs, or would the Ferritin and Iron be lower if I was celiac? I eat meat and vegetables and my periods are normal. Second Question is related to abdominal pain. I have these IBS related pains (cramping before going to the bathroom) sometimes and also some bloating and stuff. But sometimes I get this lower abdominal pain that is different, it's much much worse when I press my stomach in or touch it. It almost feel normal when I sit still in one position, but when i lean forward, touch it or press it in, it's really bad. Does anyone else with celiac relate to this kind of abdominal pain? The reason I'm asking these questions is because I'm wondering if I should get tested for celiac. I've had symptoms for a while now, and I want to suggest different blood tests to my doctor. I have a feeling I should get tested for something autoimmune. There are already three different Autoimmune diseases in my mother's family (grandmother with psoriasis, cousin with diabetes, mother with ulcerus colitis), and I've been having diffuse symptoms for a while now, like abdominal pain, diarrhea, muscle/bone pain, some joint pain, muscles falling asleep, some tingling, anxiety, neck pain, fever feeling without fever, chills, fatigue (especially after lunch), bad hangovers etc etc. The list is long. So I'm just trying to get some answers so I can be more clear with my doc. Thanks!
- 1 reply
-
- abdominal pain
- autoimmunity
-
(and 5 more)
Tagged with:
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8-M):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8-M):