-
Welcome to Celiac.com!
You have found your celiac tribe! Join us and ask questions in our forum, share your story, and connect with others.
-
Celiac.com Sponsor (A1):
Celiac.com Sponsor (A1-M):
-
Get Celiac.com Updates:Support Celiac.com!
Search the Community
Showing results for tags 'change'.
-

How Xylitol and Gluten Change Human Gut Microbiota and Biofilm
Jefferson Adams posted an article in Latest Research
Celiac.com 04/18/2024 - Human gut microbiota contains many viruses, bacteria and fungi. Escherichia coli representatives are facultative anaerobic bacteria in the colon that play a crucial role in the metabolism of lactose, vitamin synthesis and immune system modulation. E. coli forms a biofilm on the epithelial cell surface of the intestine that can be modified by diet compounds, such as gluten, xylitol, lactose and probiotics. Researchers recently examined the impact of probiotic-derived Lactobacillus rhamnosus GG strain on non-pathogenic E. coli biofilm. They also also treated mono- and multi-species biofilm with gluten, xylitol and lactose. The research team included Joanna Kwiecińska-Piróg, Karolina Chomont, Dagmara Fydrych, Stawarz Julita, Tomasz Bogiel, Jana Przekwas, and Eugenia Gospodarek-Komkowska. They arę variously affiliated with the Microbiology Department, Pharmaceutical Faculty, Collegium Medicum in Bydgoszcz, University of Nicolaus Copernicus in Toruń in Bydgoszcz, Poland; and the Clinical Microbiology Division, Antoni Jurasz University Hospital no 1 in Bydgoszcz, Poland. Probiotics May be Helpful in Rebuilding Gut Microbiota After Broad Spectrum Antibiotic Therapy The researchers used 96-well plates to obtain biofilm growth. They stained the biofilm with crystal violet. To evaluate the type of interaction in mono- and multispecies biofilm, a new formula was introduced - biofilm interaction ratio index (BIRI). To describe the impact of nutrients on biofilm formation, they calculated the biofilm formation impact ratio (BFIR). The biofilms formed by both examined species are stronger than in monocultures. All the BIRI values were above 3.0. It was found that the monospecies biofilm of L. rhamnosus is strongly inhibited by gluten (84.5%), while the monospecies biofilm of E. coli is strongly inhibited by xylitol (85.5%). The mixed biofilm is inhibited by lactose (78.8%) and gluten (90.6%). The relations between bacteria in the mixed biofilm led to changes in biofilm formation by E. coli and L. rhamnosus GG. Study Highlights: • Combining E. coli and L. rhamnosus creates a stronger biofilm than when each bacterium is cultured alone. • Adding xylitol to the diet can decrease the formation of biofilms by E. coli bacteria. • Lactose and gluten are less effective than xylitol in reducing the formation of biofilms by E. coli bacteria. The results indicate tha t probiotics might be helpful in rebuilding the gut microbiota after broad spectrum antibiotic therapy, but only if gluten and lactose are excluded from diet. Graphic Abstract Read more at: Sciencedirect.com- 1 comment
-
- biofilm
- celiac disease
-
(and 8 more)
Tagged with:
-
Celiac.com 09/11/2017 - The FDA has granted clearance for Immco Diagnostics' ELISA for celiac disease, and for Roche's Benchtop Analyzer. What does that mean? Immco's test is conducted as a solid phase immunoassay and is intended for the qualitative or semiquantitative detection of IgA or IgG antigliadin antibodies in human blood, and thus to aid in diagnosing patients with celiac disease or dermatitis herpetiformis in conjunction with other laboratory and clinical findings. In other important diagnostic news, a benchtop analyzer from Roche Diagnostics and an immunoassay system from Shenzhen New Industries Biomedical was among the instruments and tests cleared by the US Food and Drug Administration in July, according to the agency. The FDA granted 510(k) clearance to Roche's Cobas b 101 instrument platform, as well as the Cobas HbA1c test. The fully automated and self-contained Cobas b 101 uses a single-use reagent disc to measure HbA1c from capillary and/or venous whole-blood samples, according to a document filed with the FDA. The Cobas HbA1c is an in vitro diagnostic test for detecting the presence of glycate hemoglobin, which develops when hemoglobin joins with glucose in the blood, becoming 'glycated'. By measuring glycated hemoglobin (HbA1c), clinicians are able to get an overall picture of what our average blood sugar levels have been over a period of weeks/months. For people with diabetes this is important as the higher the HbA1c, the greater the risk of developing diabetes-related complications. The HbA1c assay is designed for use with the Cobas b 101 platform, which is not a portable home test, but is intended for a clinical laboratory or point-of-care setting. Other instruments receiving FDA clearance in July include a new flow cytometer from Becton Dickinson; an expanded version of Bruker's MALDI Biotyper; and expanded indications for BioMérieux's Vitek MS MALDI-TOF Mass Spectrometery System. The FDA recently cleared the Maglumi 2000 automated immunoassay analyzer from Shenzhen New Industries Biomedical, which uses chemiluminescent technology for running IVD tests on clinical serum samples. The firm's Maglumi 2000 TSH assay for the quantitative determination of thyroid-stimulating hormone in human serum also received 510(k) clearance. The assay is for diagnosing thyroid disorders. These are just a few of many new tests and analysis devices that are changing the way doctors diagnose and manage celiac disease, diabetes, and other diseases. Look for tests like this to have a profound influence on the way diseases are diagnosed and managed in the future. Read more: 360dx.com
-
- celiac
- celiac disease
-
(and 7 more)
Tagged with:
-
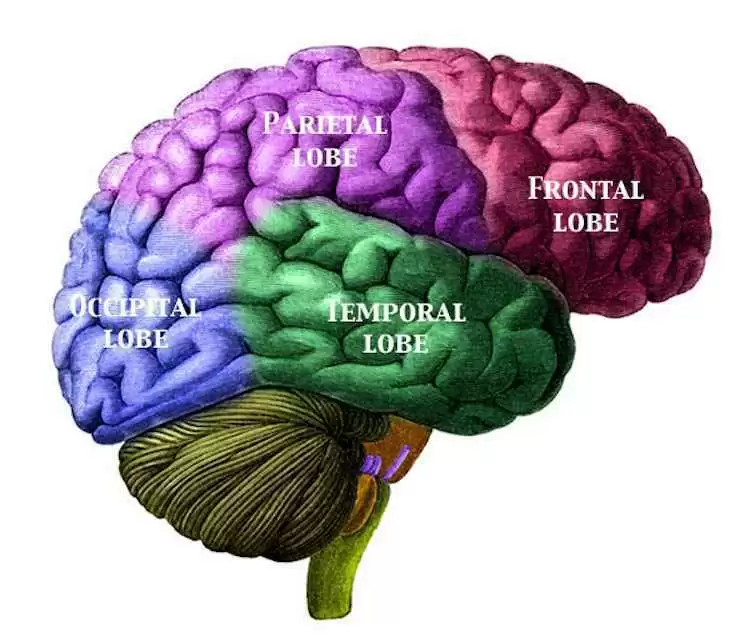
Celiac.com 06/12/2017 - Previously, Transcranial Magnetic Stimulation in de novo celiac disease patients has signaled an imbalance in the excitability of cortical facilitatory and inhibitory circuits. Researchers have reported that, after about of 16 months on a gluten-free diet, patients experience a global increase of cortical excitability, which suggests some kind of compensation for disease progression, likely mediated by glutamate. To better assess these finding, a team of researchers recently conducted cross-sectional evaluation of the changes in cortical excitability to TMS after a much longer gluten-free diet. The research team included M. Pennisi, G. Lanza, M. Cantone, R. Ricceri, R. Ferri, C.C. D’Agate, G. Pennisi, V. Di Lazzaro, and R. Bella. They are variously affiliated with the Spinal Unit, Emergency Hospital "Cannizzaro", Catania, Italy, the Department of Neurology IC, I.R.C.C.S. "Oasi Maria SS.", Troina, Enna, Italy, the Department of Medical and Surgical Sciences and Advanced Technologies, Section of Neurosciences, University of Catania, Catania, Italy, the Gastroenterology and Endoscopy Unit, University of Catania, Catania, Italy, the Department "Specialità Medico-Chirurgiche,” University of Catania, Catania, Italy, and the Institute of Neurology, Campus Bio-Medico University, Rome, Italy. For their study, the team enrolled twenty patients who had followed an adequate gluten-free diet for about 8.35 years, on average. They then compared the results with twenty de novo patients, and twenty more healthy controls. The team measured Transcranial Magnetic Stimulation, recorded from the first dorsal interosseous muscle of the dominant hand, as follows: resting motor threshold, cortical silent period, motor evoked potentials, central motor conduction time, mean short-latency intracortical inhibition and intracortical facilitation. De novo patients showed a shorter cortical silent period, while responses for gluten-free diet participants were similar to controls. Regardless of diet, all celiac patients showed a significantly smaller amplitude of motor response than did control subjects, Again, without regard to diet, all celiac patients showed a statistically significant decrease of mean short-latency intracortical inhibition and enhancement of intracortical facilitation with respect to controls. The team also observed that gluten-free celiac patients showed more intracortical facilitation compared to non-gluten-free patients. Neurological examination and celiac disease-related antibodies were both negative. This study showed that a gluten-free diet helps to mitigate the electrocortical changes associated with celiac disease. Even so, in many patients, an intracortical synaptic dysfunction, mostly involving excitatory and inhibitory interneurons within the motor cortex, may persist. The calls for further investigation into the clinical significance of subtle neurophysiological changes in celiac disease. Source: PLoS One. 2017 May 10;12(5):e0177560. doi: 10.1371/journal.pone.0177560. eCollection 2017.
- 1 comment
-
- activity
- associated
- (and 12 more)
-
Celiac.com 07/17/2014 - Italian researchers are claiming a major scientific and potentially commercial breakthrough that could lead to a revolution in the food available to people with celiac disease. The researchers, all at the Department of Agricultural Sciences, Food and the Environment, University of Foggia are claiming that their revolutionary new method will enable the manufacture of wheat products safe for people with celiac disease. The method method involves modifying the gluten proteins in standard wheat so that it will not trigger an adverse gluten reaction in people with celiac disease. They claim that their method enables the production of celiac safe and gluten-friendly foods containing “all the dough and baked products made with flour from commonly obtained wheat.” A patent has been made by Prof. Aldo Di Luccia and Prof. Carmen Lamacchia, and CNR researcher Dr. Carmela Gianfrani. The application was filed in Italy with the Italian Patent and Trademark Office at the Ministry of Economic Development, on 2 October 2012. An application for extension according to the International Patent Cooperation Treaty (PCT) was filed on 29 April 2013. Both researchers have earned a very positive evaluation by the award of the higher threshold of the so-called "scientific credibility". Specifically, they claim that their method induces changes in gluten proteins, which break the chain of chemical combinations that trigger the so-called "intolerance" changes, thus avoiding the inflammatory process that interferes with nutrient absorption, and causes lesions and bowel dysfunction. Source: University of Foggia
-
Celiac.com 03/08/2012 - Eating gluten-free for an entire lifetime is no easy task. Many people with celiac disease and gluten-sensitivities would love an alternative to a gluten-free diet, and a number of companies are looking to develop alternative therapies that would enable people to consume gluten without suffering damage. Even though nearly all drug-development programs include gluten challenges, very little is known about the duration of gluten challenge and gluten dosage. That is, how quickly does gluten cause damage, and at what dosages? A team of researchers recently studied the ways in which antibodies respond and mucosa change when the small bowel is exposed to gluten in people with celiac disease. The study team included Marja-Leena Lähdeaho, Markku Mäki, Kaija Laurila, Heini Huhtala, and Katri Kaukinen. To assess the amount of gluten-exposure needed to cause some small-bowel mucosal deterioration, the team conducted a gluten-challenge on twenty-five adult celiac patients. Each patient received either a low (1-3 g) or moderate (3-5g) doses of gluten daily for 12 weeks. The team assessed patient symptoms, including small-bowel morphology, densities of CD3+ intraepithelial lymphocytes (IELs) and celiac serology. Their results showed that both moderate and low amounts of gluten induced small-bowel damage in 67% of celiac patients. However, moderate gluten doses also caused mucosal inflammation and gastrointestinal symptoms in seven patients that lead to their premature withdrawal from the study. Interestingly, 22% of patients who developed significant small-intestinal damage showed no symptoms. The team concludes that, for most people with celiac disease, even low amounts of gluten can cause significant mucosal changes. However, since many people with celiac disease show no such response, sample sizes must be large enough to be statistically significant. Source: BMC Gastroenterology. 2011;11(129).
-
Celiac.com 01/19/2010 - A new study says that migraines and carpal tunnel syndrome may point to celiac disease. Moreover, 35% of people with celiac disease report a history of depression, personality changes, or psychosis. Others commonly suffer from neurological issues that are not improved with a gluten-free diet. Researchers recently screened a cohort of 72 patients with biopsy-proven celiac disease, recruited through advertisements and interviewed using a standard questionnaire. Nearly one in three celiac patients (28%) reported a history of migraine, though numerous patients showed a decrease in frequency and intensity of migraine attacks after adopting of a gluten-free diet. While about 20% of patients suffered from carpal tunnel syndrome, epilepsy was, surprisingly, less common than expected," report the researchers. "Only 4 individuals presented with a history of generalized or focal seizures." In general, doctors believe about 6% to 10% of celiac patients show typical neurological presentations, the study authors note. Prior studies have shown cerebellar ataxia to be the most common celiac disease-associated neurological symptom. This new study found cerebellar ataxia in 6% of patients, and vestibular dysfunction in another 6%. In all, 26% of patients showed afferent ataxia. About a third of patients had problems with stance and gait, with numerous cases of deep sensory loss and reduced ankle reflexes. "Gait disturbances in celiac disease do not only result from cerebellar ataxia but also from proprioceptive or vestibular impairment," report investigators led by Katrin Bürk, MD, from the University of Marburg in Germany. The bad news is that such neurological problems may develop "despite strict adherence to a gluten-free diet," says Burke. "Most studies in this field are focused on patients under primary neurological care," the researchers note. "To exclude such an observation bias, patients with biopsy-proven celiac disease were screened for neurological disease." Motor problems, such as basal ganglia symptoms, pyramidal tract signs, tics, and myoclonus, were not common. A total of 14% of patients reported problems with bladder function. The underlying causes for neurological problems in celiac disease are not yet understood. There has been some evidence to implicate deficiencies in folic acid, vitamin E, and biopterin in the pathogenesis. However, the investigators note that, in most patients, replacement therapy does not resolve clinical symptoms. They note also that hypo-vitaminosis rarely causes obvious abnormalities in celiac patients, and most with neurological symptoms show no evidence of any nutritional deficiencies. "The prevalence of neurological manifestations in celiac disease is striking and must be considered more than accidental," they say. "The patients' gluten-free diet had resolved intestinal symptoms but had not prevented the development of neurological deficits." The investigators suggest that, because of the considerable clinical variability, neurological and psychiatric dysfunction in celiac disease is likely the result of numerous pathogenic mechanisms. Source: Mov Disord. 2009;24:2358-2362.
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8-M):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8-M):