-
Welcome to Celiac.com!
You have found your celiac tribe! Join us and ask questions in our forum, share your story, and connect with others.
-
Celiac.com Sponsor (A1):
Celiac.com Sponsor (A1-M):
-
Get Celiac.com Updates:Support Celiac.com!
Search the Community
Showing results for tags 'celiac'.
-

How To Get Enough Fiber on a Gluten-Free Diet
Jefferson Adams posted an article in Additional Concerns
Celiac.com 12/18/2019 - If you have celiac disease, ditching wheat, rye and barley, and eating gluten-free is mandatory for proper healing. Adopting a gluten-free diet can pose huge challenges, but it's also an opportunity to improve nutrition and well-being. One of the biggest challenges gluten-free eaters face is getting enough alternative sources of fiber. Wheat, rye and barley are excellent sources of fiber, so going gluten-free can mean potentially facing a fiber deficit, especially if you eat processed gluten-free foods. Eating enough fiber is crucial for optimal long-term health. Fiber comes in two types. Soluble fiber is found in beans, legumes, nuts, oats, and some fruits and vegetables. Soluble fiber pulls water into your gut and turns into a gel, which slows digestion and helps you to feel full for a longer time. Insoluble fiber is typically found in whole grains, and vegetables. Insoluble fiber supports gut health, promotes healthy bowel movements, and eases constipation. In addition to eliminating wheat, rye and barley, it's important to eliminate or avoid variations of wheat including einkorn, farro, Kamut and spelt. So, what to eat? The solution, is to " (b)uild your gluten free-diet around fresh vegetables, fruits, dried beans, peas and lentils, nuts and seeds, and experiment with gluten-free grains," says Alicia Romano, a dietitian at Boston's Tufts Medical Center, and a spokeswoman for the Academy of Nutrition and Dietetics. Eat Gluten-Free Whole Grains One way to get on the path is to start with easy-to-find, simple-to-prepare brown rice, wild rice, quinoa and gluten-free oats, then branch out to grains such as buckwheat, teff, amaranth and millet. Eat Plenty of Fresh Vegetables Vegetables are nutritious, high-fiber, and naturally gluten-free. Fiber-rich vegetables include winter squash, green peas, corn, and potatoes and sweet potatoes with the skin. Other, less starchy, vegetables with good fiber include leafy greens, asparagus, mushrooms and cruciferous vegetables such as Brussels sprouts, broccoli, cauliflower and cabbage. Eat Plenty of Fresh Fruits Many fruits are a good source of fiber, vitamins, minerals, and antioxidants. Avocados, bananas, apricots, berries, cherries, citrus, and mango are all excellent sources of dietary fiber. Avoid Processed Foods Note that none of these food categories includes processed food. Although things are changing, many gluten-free processed foods have traditionally been low in fiber and high in things such as salt, sugar, fat, tapioca, or cornstarch. Do you have any favorite high fiber foods, or tips for getting enough fiber on a gluten-free diet? Share them in the comments section below. Read more at: fredericksburg.com-
- celiac
- celiac disease
-
(and 4 more)
Tagged with:
-
Celiac.com 12/11/2019 - While celiac disease affects an estimated 1% of people worldwide, more than 90% of people with the disease remain undiagnosed. Current celiac disease protocols call for screening patients with gastrointestinal symptoms or other autoimmune diseases, along with any first-degree relatives of celiac patients. However, current screening usually involves a trip to the doctor's office for a blood test that measures levels of celiac-specific antibodies. That simple trip can be a barrier to screening, and thus to treatment and healing. Even in more developed countries, more than half of celiacs are unaware of their disease. Rapid diagnosis and treatment of celiac disease is important, because delayed diagnosis often means persistent symptoms even after treatment, along with impaired quality of life. One solution lies in point-of-care (POC) testing, which moves medical testing from central laboratories directly to the place where the patient is receiving care. To assist in rapid and reliable disease screening, researchers from the University of Helsinki have developed a novel diagnostic method coined RFS (Rapid FRET serodiagnostics) for the rapid on-site measurement of antibodies from patient samples. This technology could revolutionize blood screening for microbial, autoimmune and allergic disorders. That same team recently applied their new diagnostic method to celiac disease screening. Fast and Easy Detection of Celiac Antibodies The research team took blood samples from 35 children and 35 adults with celiac disease. They also took samples from healthy control subjects. They measured samples with the new test method, and compared results with two current methods. According to Juuso Rusanen, MD, "The performance of the test was comparable to that of current methods, [which] involves transporting the sample to a central laboratory and a multi-step procedure taking hours." The new method provides accurate results "in less than half an hour by simply combining the sample and a reagent mix, waiting for a while and reading the result." Rusanen says that the team hopes that the new method can "lower the threshold for screening of celiac disease and thus help overcome the vast under-diagnosis of this relatively common condition." This test marks the first time their method has been used for diagnosing an autoimmune disease. The promising results invite the development of similar diagnostic tests aimed at other autoimmune diseases, says Rusanen. Read more at Eurekalert.com
- 2 comments
-
Celiac.com 12/10/2019 - Any mother of children with celiac disease can likely empathize with actress Casey Wilson. The Mrs. Fletcher star confesses that she was at wit's end when testing confirmed that her son, Max had celiac disease — a genetic, auto-immune condition triggered by gluten consumption. At first, she said, she was convinced the sky was falling, that the situation was "absolutely dire and it was my fault, that what needed fixing was me." While Wilson was happy to finally have an answer, the star also emphasized how the experience made her reflect on the ways she viewed herself as a mother. With time, and some support from husband, David Caspe, Wilson began to calm down and get a handle on her feelings, and a perspective on the situation. “It was a shock, followed by unimaginable relief," she said. "We finally had a diagnosis, and in the grand scheme of things it was a very manageable one,” the actress shared of learning her son’s condition. “We felt lucky it was not something worse.” As is not unprecedented, Max got tested, and thus diagnosed, by accident. It was only after suffering a broken leg, and a later seizure that doctors ordered a battery of blood tests, including a screen for celiac antibodies, which revealed the celiac disease. For all his early challenges, after six months on a gluten-free diet, Max saw major improvements in behavior and mood. “In six months, almost to the day, his truer self emerged...he is now an outwardly thriving, happy 4-year-old who is exploding with creativity and bursting with life,” she proudly shared. Like so many moms, Wilson came to learn that “It wasn’t about me! It wasn’t about my failure as a mother. And that’s something I have had to reckon with,” she explained. “Why was I so hard on myself? Why are we mothers all so hard on ourselves? With each passing day as his health improves, so too does my mental health.” For any parent, having children become sick, or get diagnosed with an auto-immune condition like celiac disease, can be a serious blow, and offer strong invitations toward guilt, and self-blame. Casey Wilson's experience shows a very human aspect of the very human struggle to deal with such a reality. Hopefully, her story will help others struggling with similar scenarios. We wish her the best. Do you have a story of struggling through a child's diagnosis with celiac disease? Share your story in our comments section below. Read more at: people.com
-
Celiac.com 12/04/2019 - There still is no easy and accurate way to monitor and diagnose celiac disease in patients who've been on a gluten-free diet for a while. Celiac disease patients on a gluten-free diet experience reactions to gluten, but researchers really don't understanding those reactions in any meaningful way. Systemic cytokine release was recently linked to reactivation of gluten immunity in celiac disease. A team of researchers recently set out to define the nature and time-course of symptoms and interleukin-2 changes specific for celiac disease patients. Their study shows that interleukin-2 assessment could help doctors monitor and diagnose celiac disease in patients already following a gluten-free diet. The research team included Jason A. Tye-Din, A. James M. Daveson, Hooi C. E, Gautam Goel, James MacDougall, Sarah Acaster, Kaela E. Goldstein, John L. Dzuris, Kristin M. Neff, Kenneth E. Truitt and Robert P. Anderson. They are variously affiliated with the Immunology Division, Department of Medical Biology, The Walter and Eliza Hall Institute, University of Melbourne, Parkville, Vic., Australia; Department of Gastroenterology, The Royal Melbourne Hospital, Parkville, Vic., Australia; University of Queensland, Brisbane, Qld, Australia; Sir Charles Gairdner Hospital, Perth, WA, Australia; ImmusanT, Inc., Cambridge, MA, USA; Prometrika, LLC, Cambridge, MA, USA; and Acaster Lloyd Consulting Ltd., London, UK. The team presented a gluten challenge to 25 celiac disease patients following a gluten-free diet, and to 25 healthy control subjects. Each group consumed a standardized 6 gram gluten challenge. The team compiled a Celiac Disease Patient-Reported Outcome survey and global digestive symptom assessment each hour for up to 6 hours after gluten challenge. They also recorded adverse events over a 48 hour period, and assessed serum interleukin-2 levels at baseline, and at 2, 4 and 6 hours. Healthy control subjects showed no detectable levels of serum interleukin-2, while 92% of celiac patients showed no detectable levels at baseline, but levels >0.5 pg/ml at 4 hours. Patient-reported outcome severity scores remained steady for all control subjects, while scores for celiac patients rose sharply after gluten in celiac disease patients. Symptoms of gluten exposure started at the 1 hour mark, and topped out after three hours. Patients with serious reactions typically suffered from nausea and vomiting, while those with milder reactions experienced headache and fatigue. The highest interleukin-2 levels were associated with more severe symptoms, especially nausea and vomiting. The timing and severity of gluten ingestion symptoms in people with celiac disease are strongly connected to elevated levels of serum interleukin-2. A gluten food challenge combined with interleukin-2 assessment could be valuable clinical tool for monitoring and diagnosing celiac disease in patients established on a gluten-free diet. Alimentary Pharmacology & Therapeutics
-
- celiac
- celiac disease
-
(and 6 more)
Tagged with:
-
Danna Korn founded R.O.C.K. in 1991 after her son, Tyler, was diagnosed with celiac disease. It has grown to international proportions, helping families all over the world deal with the unique challenges of raising a child on a gluten-free diet. When children are diagnosed with celiac disease at an early age, they usually have a severe intolerance to gluten, and are often extremely sick when ultimately diagnosed. Most parents share horror stories of visiting several doctors before finally arriving at a diagnosis, and are frustrated, exasperated, and angry, yet relieved to finally have a direction in which to turn. Sometimes it helps to talk about it, and it always helps to have some guidance when initially diving into the gluten-free diet. Raising Our Celiac Kids is a support group for parents, families and friends of kids with celiac disease or gluten intolerance. We welcome families of autistic kids involved in a gluten-free/casein-free dietary intervention program. We concentrate on dealing with the unique challenges that we have, including: Finding "fun" gluten-free treats for kids Menu ideas for school lunches, quick dinners, and sports snacks Helping the kids to take responsibility for reading labels, cooking and planning/preparing food How to prepare for unexpected birthday parties and food-oriented activities at school, church, and elsewhere Halloween, Easter, and other special days - how do we include our kids safely? Educating day-care providers and teachers - without burdening them Dealing with grandparents, babysitters, and "helpful" friends who offer gluten-containing foods to our kids Ensuring our kids won't cheat, and what to do WHEN they do Sending kids away to camp, friends' houses, and other times when we're not around to help The psychological impact of growing up with celiac disease (peer pressure, teenage years, and more) Visit their site at: https://www.raisingourceliackids.org/ R.O.C.K. Chapters in the United States Alabama Support Group - Mobile Contact: Marilyn Taylor ROCK’n Mobile, Alabama Tel: (251) 633-3528 E-mail: Taylor6211@bellsouth.net Slocomb - Support Group Contact: Nichole Alexander E-mail: mamma_hen3@hotmail.com Tel: (334) 886-7150 Alaska Chugiak - Support Group Raising Our Celiac Kids (R.O.C.K.) - ROCK'n Alaska Contact: Debbie Saddler Chugiak, AK 99567 Tel: (907) 688-6879 E-mail: alaskadebbie@gmail.com Arizona Gilbert - Support Group Raising Our Celiac Kids (R.O.C.K.) - Gilbert Chapter Contact: Deanna Frazee Gilbert, AZ Tel: (480) 641-8821 E-mail: deannafrazee@hotmail.com Phoenix - Support Group Greater Phoenix R.O.C.K. Contact: Lisa Potts Email: phoenixceliackids@gmail.com FB Page: facebook.com/PHX.ROCK Phone: (858) 442-5956 E-mail: lisa.potts4911@gmail.com Internet: www.phoenixrock.org Tucson - Support Group Raising Our Celiac Kids (R.O.C.K.) - Tucson Chapter Contact: Liz Attanasio Tel: (520) 877-9181 Tucson - ROCK'n Tucson Contact: Shelli Hanks Tucson, AZ 85750 Email: TucsonROCK@comcast.net Tel: (520) 577-0774 Arkansas Fayetteville, AR Melanie Faught Fayetteville, AR 72704 Tel: (479) 582-9232 E-mail: melaniefaught@cox.net California Conejo Valley - Support Group ROCK'n Conejo Valley Contact: Melissa Riches Westlake Village, CA 91361 Tel: (818) 706-0197 E-mail: melissa.riches@sbcglobal.net Danville - Support Group Contact: Ann Reigelman Raising Our Celiac Kids (R.O.C.K.) - Danville Chapter Danville, CA E-mail: areigelman@yahoo.com Lake Balboa - Support Group Contact: Melissa Gray Raising Our Celiac Kids (R.O.C.K.) - Lake Balboa Chapter Tel: (818) 510-0534 E-mail: Melissagray808@gmail.com Los Angeles - Support Group Contact 1: Amy Harley Tel: (818) 249-2432 E-mail: harleyhome@earthlink.net Contact 2: Cheryl Cohen Tel: (818) 784-4516 E-mail: cohencheryl@yahoo.com Moreno Valley - Support Group Contact: Kellee Shearer Raising Our Celiac Kids (R.O.C.K.) - Moreno Valley Chapter 10034 Snipe Circle Moreno Valley, CA 92557 Tel: (951) 242-8448 E-mail: Treshearer@aol.com Orange County - Support Group Contacts: Randi Leinen Raising Our Celiac Kids (R.O.C.K.) - Orange County Chapter E-mail: RMLeinen@aol.com ROCK’n Orange County, CA Contact: Drew Grant Tel: (949) 257-6349 E-mail: orangecountyrock@gmail.com Palo Alto - Support Group Contact: Kelly Velez or Debbie Duncan Bay Area ROCK E-mail: kellyvelez@comcast.net Tel: (650) 303-8409 E-mail: debbie@debbieduncan.com Tel: (650) 494-6959 San Diego - Support Group Raising Our Celiac Kids (R.O.C.K.) - San Diego Chapter Contact: Brenda McDowell E-mail: sdrockchapter@gmail.com San Francisco - Support Group Contact: Lisa Palme Raising Our Celiac Kids (R.O.C.K.) - San Francisco Chapter E-mail: palmer@smccd.net Sebastopol - Support Group ROCK North Bay Chapter Contact: Jennifer Iscol Sebastopol, CA 95472 Tel: (707) 824-5830 E-mail: iscol@aol.com Visalia (Central) - Support Group Contact: Shannon Williams Tel: (559) 741-1671 Visalia, CA Colorado Peyton - Support Group ROCK’n Peyton, CO Crystal Brauer Tel: (719) 494-8590 E-mail: Brauer.family@yahoo.com Connecticut Raising Our Celiac Kids (R.O.C.K) Fairfield County CT Contact: Karen Loscalzo/ Monika Lazaro/ Carolyn Caney E-mail: rockfairfieldcounty@gmail.com Internet: www.ROCKFairfieldCounty.com Simsbury - Support Group Raising Our Celiac Kids - R.O.C.K. - Simsbury Chapter Contact: Mark & Tracy Saperstein Tel: (860) 651-4857 E-mail: mtbahs@comcast.net Waterford - Support Group Raising Our Celiac Kids - R.O.C.K. - Waterford Chapter Contact: Donna Kensel Waterford, CT E-mail: CtCeliacKids@aol.com Florida Apopka - Support Group Contact: Deborah Pfeifle Raising Our Celiac Kids (R.O.C.K.) - Apopka Chapter Apopka, FL 32712 Tel: (407) 880-6104 E-mail: dpfeifle@earthlink.net Coral Springs/Palm Beach - Support Group Contacts: Janna Faulhaber and Stacey Galper Raising Our Celiac Kids (R.O.C.K.) - Coral Springs/Palm Beach Chapter Tel: (954) 255-7855 E-mail: Staceynagel@paxson.com Odessa (Tampa) - Support Group Contact: Terri Willingham Raising Our Celiac Kids (R.O.C.K.) - Odessa Chapter Orlando - ROCK'n Celebration - Support Group Contact: Rose Parvaz Celebration, FL 34747 E-mail: rose.parvaz@celebration.fl.us Palm Beach gardens - Support Group ROCK'n Palm Beach Gardens Contact: Kimberly Wade Palm Beach Gardens, FL 33418 E-mail: tkcrw@comcast.net Tel: (561) 625-9005 Tampa - Support Group Contact: Melissa Ransdell Raising Our Celiac Kids (R.O.C.K.) - Tampa Chapter 14521 Nettle Creek Rd. Tampa, FL 33624 Tel: (813) 265-8105 Georgia Atlanta - Support Group Contact: Jeff Lewis, M.D. Children's Center for Digestive Health Care Raising Our Celiac Kids (R.O.C.K.) - Atlanta Chapter E-mail: jlewis@ccdhc.org Illinois Chicago - Support Group ROCK'n Chicago Contact: Alexandra Vavouliotis Tel: (847)-962-7244 E-mail: alexvav24@mac.com Dekalb - Support Group Contact: Audrey O'Sullivan Raising Our Celiac Kids (R.O.C.K.) - Stillman Valley Chapter Dekalb, IL Tel: (815) 756-2606 E-mail: Audrey08@aol.com ROCKn DuPage & Cook County Aleksandra de Leon -DuPage County E-mail: aleksandra.deleon@gmail.com Tel: 630-745-7429 Ilene Harris- Cook County E-mail: isf27@yahoo.com Tel: 847-222-9950 Moline - Support Group Contact: Lesley Lamphier ROCK'n Illinois (Moline) Moline, IL 61265 Tel: (309) 736-1507 E-mail: celiackids@mchsi.com Springfield - Support Group Land of Lincoln Celiac Support Group Contact: Joyce Hall Raising Our Celiac Kids (R.O.C.K.) - Springfield Chapter Springfield, IL Washington - Support Group Heart of Illinois Celiac Kids Contact: Samantha Young E-mail: info@hoiceliackids.com Indiana Henryville - Support Group Contact: Kristie Williams ROCK'n Indiana (Henryville) Henryville, IN 47126 Tel: (812) 294-1179 E-mail: kristiewilliamsrn@hotmail.com Indianapolis - Support Group Contact: Kelly Kurzhal ROCK’n Indianapolis Indianapolis, IN 46217 Tel: (317) 697-4933 E-mail: kellykurzhal@hotmail.com Mooresville - Support Group Contact: Cindy Holder Raising Our Celiac Kids (R.O.C.K.) - Mooresville Chapter 375 E. Countyline Rd. Mooresville, IN 46158 Tel: (317) 831-9871 E-mail: Holders2@comcast.net Iowa Des Moines - Support Group Contact: Lindsay Amadeo Raising Our Celiac Kids (R.O.C.K.) - Des Moines Chapter Des Moines, IA E-mail: llamadeo@yahoo.com Maryland ROCK'n Maryland Contact: Steffani Mykins Tel: (410) 626-1958 E-mail: stfine@comcast.net ROCK’n Maryland Contact: Lindsay Moe Mt. Airy, MD 21771 (443) 799-3432 E-mail: lindsaymoe@ymail.com Massachusetts Longmeadow - Support Group ROCK'n MA Contact: Christie Freda Longmeadow, MA 01106 E-mail: cfreda126@comcast.net Tel: (413) 567-5748 Somerset - Support Group Contact: Stacey Nasrallah ROCK'n Somerset (MA) Somerset, MA 02726 Tel: (508) 674-6211 E-mail: info@somersetrock.org Internet: http://www.somersetrock.org Michigan Ann Arbor - Support Group Contact: Anne MacDougald ROCK’n Michigan E-mail: anniemacdougald@gmail.com Macomb Township - ROCK'n MI Support Group Contact: Kimberly Fanelli Macomb Township, MI 48044 Tel: (586) 226-8480 E-mail: kfanelli@mac.com West Bloomfield - Support Group Contact: Gail Smoler Raising Our Celiac Kids (R.O.C.K.) - West Bloomfield Chapter 4358 Strathdale Court West Bloomfield, MI 48323 Tel: (248) 851-9451 E-mail: GailS63@aol.com Minnesota Minneapolis/St. Paul Support Group Contact: Lynda Benkofske Raising Our Celiac Kids (R.O.C.K.) - ROCK-Minneapolis/St. Paul Chapter E-mail: twincitiesrock@gmail.com Mississippi Columbia - Support Group Contact: Beth Broom Raising Our Celiac Kids (R.O.C.K.) - South Mississippi Chapter 50 Wilks Road Columbia, MS 39429 E-mail: sbroom@dixie-net.com Missouri O'Fallon - Support Group Contact: Beth Anne Miller 7264 Sweetcider Lane O'Fallon, MO 63366 Tel: (636) 294-2037 E-mail: Frankbethm@aol.com Montana Billings - ROCK'n Montana Support Group Billings, MT 59102 Contact: Perrin Grubbs E-mail: perrin@bresnan.net Tel: (406) 655-7897 Nevada Reno - Support Group Contact: Carrie Owen Raising Our Celiac Kids (R.O.C.K.) - Reno Chapter Tel: (775) 857-2708 E-mail: Renorockgroup@yahoo.com New Hampshire Manchester - Support Group Contact: Michelle Ouellette ROCK'n New Hampshire Manchester, NH 03102 Tel: (603) 627-1831 E-mail: rocknh2006@gmail.com New Jersey Blairstown - Support Group Contact: Marla Benson Raising Our Celiac Kids (R.O.C.K.) - Blairstown Chapter Blairstown, NJ MBenson890@aol.com (808) 362-7752 Freehold - Support Group Contact: Elissa Carlin Raising Our Celiac Kids (R.O.C.K.) - Freehold Chapter Marlboro, NJ 07746 Tel: (732) 252-8309 E-mail: ElissaC75@aol.com Morristown - Support Group ROCK'n New Jersey Contact: Andrea Kitzis Smith Morristown, NJ 07960 Tel: (201) 965-7309 E-mail: akitsm@att.net Short Hills - Support Group Contact: Ellie Fried Raising Our Celiac Kids (R.O.C.K.) - North Jersey Chapter Tel: (973) 912-0253 New Mexico Albuquerque - Support Group Contact: Traci Shrader Tel: (505) 450-1156 E-mail: tashrader@msn.com New York Auburn - Support Group R.O.C.K.'n Auburn Contact: Nicki Hai Tel: (315) 252-2764 E-mail: jnhai@roadrunner.com Glens Falls Region - Support Group Contact: Lisa Fox Lake George, NY 12845 Tel: (518) 668-5838 E-mail: fox_lisa@hotmail.com ROCK’n Hudson Valley, NY Contact: Terresa Bazelow Thompson Ridge, NY Tel: (845) 609-7432 E-mail: HVNYROCK@aol.com Nassau County- Support Group Contact: Angela Silverstein Raising Our Celiac Kids (R.O.C.K.) - Lynbrook Tel: (516) 593-2904 E-mail: venusangmm1@optonline.net Nassau/Suffolk - Support Group Contact: Randi Albertelli Raising Our Celiac Kids (R.O.C.K.) - Long Island Chapter E-mail: rsquared31@optonline.net Contact 2: Jill Schneider Tel: (516) 551-4564 E-mail: jahms@verizon.net Rockland, NY - Bergen, NJ Raising Our Celiac Kids (R.O.C.K.) - Rockland, NY - Bergen, NJ Chapter Contact: Gabrielle Simon Telephone: (646) 342-6960 Email: nynjrockmom@yahoo.com Rome - Support Group Mohawk Valley R.O.C.K. (upstate New York) Contact: Rebecca Madeira Rome, NY Tel: (315) 337-7671 Upstate - Support Group ROCK'n Upstate New York Contact: Karen Dorazio Jamesville, NY 13078 Tel: (315) 469-8154 E-mail: kdorazio@twcny.rr.com Vestal, NY ROCK’n Vestal, NY Contact: Razi Lissy E-mail: raziher@gmail.com Western New York - Support Group Raising Our Celiac Kids (R.O.C.K.) - Western New York Chapter Buffalo / Niagara Falls NY Contact: Jeanette Yuhnke Tel: (716) 625-8390 Internet: http://www.glutenfreeinwny.com/WNYCeliacKids.php Westchester, NY ROCK’n Westchester, NY Contact: Erica Peltz E-mail: Eps2104@gmail.com Tel: (917) 612-4676 North Carolina Charlotte, Support Group Contact: Nikki Everett Raising Our Celiac Kids (R.O.C.K.) - Charlotte Chapter Huntersville, NC 28078 Tel: (704) 804-4090 E-mail: haircolorexpertise@hotmail.com Harrisburg - Support Group Contact: Linda Witherspoon 5018 Wynford Ct. Harrisburg, NC 28075 Tel: (704) 957-6100 E-mail: Linda.witherspoon@aol.com Stantonsburg - Support Group ROCK’n North Carolina Contact: Carrie Forbes Stantonsburg, NC 27883 Tel: (252) 238-3132 E-mail: gingerlemongirl@gmail.com North Dakota Fargo - Support Group Contact: Stacey Juhnke Tel: (701) 237-4854 E-mail: DSJuhnke@yahoo.com Ohio Akron - Support Group Contact: Sue Krznaric Raising Our Celiac Kids (R.O.C.K.) - Akron Chapter Akron, OH Tel: (330) 253-1509 E-mail: skrznaric@cs.com Akron - Support Group Contact: Therese Semonin Raising Our Celiac Kids (R.O.C.K.) - Akron Chapter CSA Chapter 111, S.O.S. Save Our Stomachs Cincinnati - Support Group Contact: Beth Koenig Raising Our Celiac Kids (R.O.C.K.) - Cincinnati Chapter Cincinnati, OH E-mail: BethKoenig@cinci.rr.com Tel: (513) 923-4435 Cleveland - Support Group ROCK’n Cleveland Contact: Tracey Lavine Solon, OH 44139 Tel: (216) 533-1285 E-mail: Tracey95@aol.com Toledo - ROCK'n Toledo Support Group Contact: Amy Kinkaid Toledo, OH 43615 E-mail: kinkaida@bex.net Tel: (419) 509-6913 Oregon Salem - Support Group Contact: Kristen Klay Raising Our Celiac Kids (R.O.C.K.) - Salem Chapter Tel: (503) 581-3884 E-mail: kristenklay@yahoo.com Pennsylvania Greenville - Support Group Contact: Fiona Garner Raising Our Celiac Kids (R.O.C.K.) - Greenville Chapter Greenville, PA Glenside - Support Group Raising Our Celiac Kids (R.O.C.K.) - Glenside Contact: Wilhelmina Green Glenside, PA 19038 Tel: (215) 756-2708 E-mail: Wilhelmina.green@gmail.com Greensburg - Support Group Contact: Martin Martinosky, Jr. Raising Our Celiac Kids (R.O.C.K.) - Greensburg Chapter Greensburg, PA Tel: (724) 834-3435 E-mail: ROCKchapter@aol.com Hanover - Support Group ROCK’n Hanover Contact: Melissa Panzer Hanover, PA 17331 Tel: (717) 633-1667 E-mail: Glutenfree4life@live.com Harrisburg - Support Group Gluten Intolerance Group of Harrisburg Harrisburg, PA Tel: (717) 520-9817 Lancaster/York - Support Group Contact: Janelle Gregory Tel: (717) 687-8586 E-mail: janellegregory@verizon.net Lansdale - Support Group ROCK Bucks Montgomery Contact: Holly and Steve Staugaitis Lansdale, PA 19446 Tel: (215) 997-2706 E-mail: hollystaugaitis@gmail.com South Carolina Charleston - Support Group Contact: Cathy Leeke Lowcountry R.O.C.K. Tel: (678) 637-3277 E-mail: cwleeke@yahoo.com Clover - Support Group Contact: Lauretta McInnis Raising Our Celiac Kids (R.O.C.K.) - Clover Chapter Tel: (803) 222-5143 E-mail: laurettamcinnis@gmail.com Easley - Support Group Contact: Laura Armstrong Raising Our Celiac Kids (R.O.C.K.) - Easley Chapter Easley, SC Tel: (864) 850-0344 Lexington - Support Group Contact: Gail Fox Raising Our Celiac Kids (R.O.C.K.) - Lexington Chapter Lexington, SC 29072 Tel: (803) 957-7658 E-mail: gailfox@sc.rr.com Tennessee Nashville - Support Group Contact: Janet Lowery Raising Our Celiac Kids (R.O.C.K.) - Nashville Chapter Tel: (615) 758-2674 Woodlawn - Support Group Contact: Shantal Green Woodlawn, TN Tel: (931) 648-2289 Texas Austin - Support Group Contact: Frances Kelley ROCK'n Austin - Alamo Celiac GIG Austin, TX 78739 E-mail: fkelley@austin.rr.com Tel: (512) 301-2224 Dallas/FortWorth - Support Group Contact: Kelly LeMonds, Leader Raising Our Celiac Kids (R.O.C.K.) - Wylie Chapter 1821 Spinnaker Way Drive Wylie, Texas 75098-7855 Tel: (972) 442-9328 E-mail: leader@dallasrock.org Internet: http://www.dallasrock.org Dallas/FortWorth - Support Group Contact: Diane McConnell Raising Our Celiac Kids (R.O.C.K.) - Dallas/FortWorth Chapter Tarrant County, TX Tel: (817) 849-8646 E-mail: fortworthrock@swbell.net Houston - Support Group Contact: Janet Y. Rinehart, Chairman Houston Celiac Sprue Support Group Raising Our Celiac Kids (R.O.C.K.) - Houston Chapter 13722 Ashley Run Houston, TX 77077-1514 Tel: (281) 679-7608 E-mail: txjanet@swbell.net Internet: http://www.csaceliacs.org/ Houston - Support Group Contact: Faye Sallee Raising Our Celiac Kids (R.O.C.K.) - Houston Chapter 14830 Sagamore Hills Houston, TX 77082 Tel: (281) 496-9166 Houston - ROCK'n Houston Support Group Comtact: Monica Ryan Houston, TX 77025 Tel: (713) 667-1963 E-mail: Mwryan@ipa.net Lubbock - Support Group Contact: Beth Trostle ROCK'n Lubbock Tel: (806) 794-5917 E-mail: calvintrostle@nts-online.net Victoria - Support Group Contact: Julie Bauknight Raising Our Celiac Kids (R.O.C.K.) - Victoria Chapter Victoria, TX 77901 Tel: (361) 572-9252 Utah Holladay - Support Group Contact: Cathy Snowball ROCK’n Utah Holladay, UT 84121 E-mail: kileyannsmom@hotmail.com Ogden - Support Group Contact: Eileen Leatherow Raising Our Celiac Kids (R.O.C.K.) - Ogden Chapter Ogden, UT Virginia Ashburn - Support Group Keith Bird Tel: (703) 348-7607 rock@birdmk1.plus.com Bristow - Support Group ROCK’n Bristow Contact: Michael and Elizabeth Brown Bristow, VA 20136 Tel: (703) 753-9161 E-mail: 2xx1xy@comcast.net Fredericksburg - Support Group ROCK’n Fredericksburg Contact: Kathy Paz-Craddock Tel: (703) 507-0609 E-mail: kalalilys@gmail.com Paeonian Springs - Support Group Raising Our Celiac Kids (R.O.C.K.) - Paeonian Springs Becky Shore Tel: (571) 252-0036 E-mail: zoo2u@comcast.net Virginia Beach - Support Group Contact: Cynthia Olson E-mail: glutenfreemom@hotmail.com Washington Bellingham - Support Group Contact: Jean McFadden Layton ROCK'n Washington Bellingham, WA 98229 Tel: (360) 734-1659 E-mail: glutenfreekids@yahoo.com Bothell, WA - Support Group Contact: Lynn Crutcher Rock'n Washington Bothell, WA 98011 Tel: (425) 205-1327 E-mail: gfkids1@yahoo.com Poulsbo - Support Group Contact: Tim & Dawn Simonson Raising Our Celiac Kids (R.O.C.K.) - Poulsbo Chapter Poulsbo, WA 98370 Tel: (360) 779-9292 E-mail: timsimonson@csi.com Seattle - Support Group Contact - Irina Risuhina Raising Our Celiac Kids (R.O.C.K.) - Seattle Chapter E-Mail: iris510@hotmail.com Spokane - Support Group Contact: Jennifer Fancher ROCK'n Spokane, WA Spokane, WA Tel: (509) 891-7250 E-mail: nelsonfancher@live.com Vancouver - Support Group Contact: Theressa Rachetto Vancouver, WA 98662 Tel: (360) 713-1504 E-mail: theressarachetto@gmail.com Yakima - Support Group ROCK’n Yakima, WA Contact: Shanta Gervickas Tel: (509) 965-1130 E-mail: Shanta@network7.com West Virginia Hurricane - Support Group Contact: Karen Daniel Raising Our Celiac Kids (R.O.C.K.) - Hurricane Chapter 340 Green Acres Dr. Hurricane, WV 25526 Tel: (304) 757-0696 E-mail: krdaniel@suddenlink.net Wisconsin DePere - Support Group Contact: Pam Rourke Tel: (920) 339-7867 E-mail: mrourke@new.rr.com Jackson - Support Group Contact: Yvonne Schwalen Raising Our Celiac Kids (R.O.C.K.) - Jackson Chapter E-mail: trainman280@netzero.net R.O.C.K. Chapters in Canada Alberta ROCK 'n Olds Olds, Alberta, Canada Amy Smart 403-415-5789 asmart@telus.net
- 1 comment
-
- celiac
- celiac disease
- (and 7 more)
-
The Grey Science of Nutrition in a black and white world of Genetics and disease or the Elegant Neat IE Key method to (uncontrolled) inflammation in the body or How/Why low micronutrients IE Vitamins and restoring micronutrients aka(B-Vitamins) are key to maintaining good GI health or Why Vitamin Deficiency Test often fail to give us a black and white answer. The Purpose of this Blog post Is To Educate for “To Educate is to Free” for those who want to know and would try a Vitamin for their health…(sorry about the formatting I will endeavor to add breaks but the flow of the matter might not be concise) This Posterboy blog post is to encourage you to be tested for a B-Vitamin deficiency…but I betting you won’t test low… Through my research on Nutrients/Vitamins/Minerals IE Nutrients I with other deep researchers have come to similar opinions from different perspectives or journeys… For now …I just wanted to float the idea…of an “Elegant” theory of supplementation and how it can help people’s GI problems…. Last time I spoke of KIA’s and Jaguar’s… This time I am writing/speaking on “The Grey Science of Nutrition”…referring to an early DRAFT version of a “White” paper (new idea) not spoken or discussed before…. This will be wrong as much as right hence….the Grey Science…thought provoking ideas… though while sound in their logic and reasoning….totally unproven as to the science… the difference between an Hypothesis… and a theory… Even good working theories can take years let’s say 20+ years for this model/example… to be proven more than a good hypothesis… I will refer you to the “hormone smatter” site if you want to know more about Thiamine…which I will cite at the end regarding how and why vitamin deficiency test often fail us.... https://www.hormonesmatter.com/mitochondria-energy-not-genetics-underlies-health-disease/ Where they will say similar things …only having Thiamine aka B1 as their focus… I have spoken about my experience with Niacin aka B3 here before so I will not belabor that point now… What I want to discuss/talk about is how these B-Vitamins B1,B2, B3 together ---- work in a neat/elegant way to help control our immune system… Without which our immune system becomes disordered…IE attacks itself…. B3 was an easy target….because without it you will die…it is a medical fact… A short summary of why this is so can be seen here by a 2nd Year biology student that says it well you find “Pellagra in unexpected places” today every where are bodies needs energy… eventually Pellagra will show up… https://pellagradisease.wordpress.com/ Described here as “Pellagra: A Non-Eradicated Old Disease” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4019925/ But you do not have Pellagra but more like Pellagra Sine Pellagra aka Ariboflavinosis or a severe Riboflavin deficiency… Without energy…we can’t manage our bodies properly and stress kills us…but it maims us first… We all know stress kills but rarely do we think of it maiming us. “Fight or Flight” right! Well all these fleeing or fighting causes use to use up great amounts of energy (think Adrenaline and a young child lifting a car). Our body has a instant decision to make. Think for yourself when your GI flares up … are not you going through some personal stress in your life. Who has ever heard of the phrase – “A place for everything and everything in its place” We like for things to look neat and be neat most of the time right??? When we are low in B-Vitamins our bodies place for things get’s disordered… More importantly it should make sense to us IE be in black and white. We want to be able to find things in a moment’s notice. And why nutrition is a “Grey Science” Admit it you have gone to google and typed in a few symptoms on webmd etc (web) and diagnosed yourself of the latest plague to hit the airways. But seriously, the medical community does this almost to the extreme. If you have xxx, then it is yyy because zzz happens when you are allergic, sick, etc ad naseum. They are called “keys” in the medical community. That is why the doctor in 15 minutes can diagnose low body temperature as a thyroid problem because it is our thermostat…but nutrition rarely can be reduced to just one thing/Vitamin right? But We want these quick hits. Because it make’s sense and is easy(ier) to diagnose that way. But what if a disease is more general in scope say malaise (celiac)/NCGS or has a possible nutrition base then it get complicated (messy) more test’s (keys) are needed to see which one fits. The problem with Celiac disease today is there are many “keys” than can fit in the door and seemingly all the keys work. 200 symptom’s all least by some estimates. So it can be hard if you are not looking at the right key’s to determine if have the right diagnosis. … IBS, Chrons, NCGS etc…. The problem with this solution is the more (longer) the doctor/practitioner/clinician looks for the right key the more their patients suffers. The “key” solution works fine if the medical problem is “Neat”. “ A place (key/symptom) for Everything and everything in it’s place.” But those of who have ever been diagnosed with Celiac disease or a gluten allergy know it is anything but “Neat”. It is a very messy process at times. But if you find/are a “good” doctor/practitioner/clinician who has been through the process with another patient then luckily your diagnosis goes more smoothly. Or not? Maybe they haven’t learned the keys yet. They have seen them before maybe. IBS, NCGS, Celiac Disease, UC etc all look a lot of like. Now remember for the most part these are all “general” practitioner’s. They have a lot of keys to juggle. And after a while they all look the same. Especially if it is a “sprue” tropical or non-tropical in nature disease like Celiac is. According to the medical dictionary “sprues” are a chronic form of malabsorption syndrome Time for a little vocabulary lesson chronic what does – Chronic mean? According to google dictionary “(of an illness) persisting for a long time or constantly recurring.” … most doctor’s will call it chronic if it lasts more than 6 months. So now we have a disease/syndrome of symptom’s (more on that later) that does not fit a “neat” picture in fact it can be very messy for the patient at times (and the clinician) who is doing his/her best to help you one key at a time. INSTEAD of 15 minutes it might take 5 to 10 years until a doctor/practitioner/clinician makes sense of all his or her keys. The fact that the problem is chronic “of an illness persisting for a long time or constantly relapsing” tells him/her that she has not found the right key yet right??? Is there a better way more Elegant way? (The Answer is YES there is – It is called Vitamins/Nutrition) Disease need not be CHRONIC when one understands the underlying cause. Indeed I believe we need got to all the way back to the root cause of nutrition — Pellagra Sine Pellagra presenting as digestive disorder which is healed (put in to remission) with supplementation in as little as 3 to 4 months depending on how many times a day it (B-complex) is taken. Knowledge is power as they say….use this new found knowledge to have your doctor test for B-Vitamin deficiencies is all I ask …. have them test for Vitamin B1, B2, B3 you might be surprised…or not depending on what you expect to find... or how well the test(s) are done... The researchers where who said “Pellagra, an Almost‐Forgotten Differential Diagnosis of Chronic Diarrhea: More Prevalent Than We Think” https://onlinelibrary.wiley.com/doi/abs/10.1002/ncp.10418 That is too Elegant to theorize/propose/diagnose Vitamins’ (more correctly the lack thereof) as the (possible) cause of (Celiac) disease/GI/digestive problem’s? Vitamins are the very definition of ‘elegant’ a nutrient needed in a minimum amount without which we become sick and develop malaise, disease and syndromes (like Pellagra) or Pellagra Sine Pellagra presenting as Celiac Disease or even Beri Beri etc). See this research on a Thiamine deficiency in someone with IBS and Chronic Fatigue… Entitled Thiamine and fatigue in inflammatory bowel diseases: an open-label pilot study. https://www.ncbi.nlm.nih.gov/pubmed/23379830 The researchers were surprised to find it and your doctor probably will be too! And the doctor’s can’t find there keys/studies in the medical record until more patients are diagnosed with these Vitamin deficiencies in (More) GI patients….because a “small cohort” is not deemed to be medically significant ….you can change the future today by being tested for these Vitamin deficiencies…it is really up to you now! But you we can educate them so they will begin looking! For this key nutrient Vitamin deficiency/dependency for “To Educate is To Free” …the next generation…. But note: Pellagra did not happen in a uncomplicated way (single nutrient) IE elegant way but in complicated Triad of nutrient deficiencies….a syndrome of symptom’s…from a complex of Vitamins… hence the “Grey Area” of Nutrition have left doctor’s/clinician’s in the dark as to the true cause of your syndrome of GI symptom’s… https://casereports.bmj.com/content/12/9/e230972 **** Note: This is not medical advice. I am not diagnosing, treating or recommending you change your routine before consulting your doctor but only advocating that nutrition needs to be rediscovered today as possible cause of your GI problems….More testing will need to be performed to confirm this analysis…. I meant this to be shorter than it is but you can only cover so much in one blog post I guess. It is important to note I do not NOW take Niacinamide or Riboflavin or Thiamine and have not for several years now. If it (B-complex) is the missing ingredient/nutrient(s) you will get better UNLESS more stress/trauma occurs robbing you of your God given burp indicating to you stress is now a problem again for you. If it helps (you find you have these deficiencies) and you feel better…tell someone else who is not better yet… get your doctor to do a key/study on your experience so future doctor’s will have the key/study in the medical record to find that Pellagra Sine Pellagra or Pellagra or Beri Beri is more prevalent today than once realized… presenting together (I believe) in the capstone disease Pellagra or Pellagra Sine Pellagra (without skin manifestations) much more commonly…as It did in me…as/with Angular Cheilitis…. It (Ariboflavinosis) low Riboflavin could of presented with many other symptom’s…and I wouldn’t have and (and doctors don’t) didn’t recognize it then…until it presented with a “Capstone” symptom… with it’s many other earlier symptom’s most doctor’s (and myself) did not know Geographic tongue for instance was an early sign of low Riboflavin aka Pellagra Sine Pellagra… https://glutenfreeworks.com/health/tongue-magenta-swollen/ The earlier you recognize any disease/syndrome the more symptom’s you can spare yourself of… Knowledge is power…pass it on…hopefully to your doctor ….and you have put your “key” diagnosis in the medical record so other doctor’s can find their keys for the next patient…we can’t wait another 15 to 20 years… (has been my thing) till this nutrition(al) knowledge filters down to the medical/clinical practitioner’s level…. I am not a doctor but I like most other sufferers have armed myself with knowledge. I studied every day diligently for 4+ years before the Lord being my help …. I was able to figure out I had a Vitamin deficiency (many reallly)… now it is up to those still suffering to put it in the/your medical record(s) for others doctor’s to find it in the future! In black and white! Praise be to God! To those who hear and listen. 2 Tim 2:7 “Consider what I say; and the Lord give thee understanding in all things” this included. 2 Cor 1:3,4 3)Blessed be God, even the Father of our Lord Jesus Christ, the Father of mercies, and the God of all comfort; 4 Who comforteth us in all our tribulation, that we may be able to comfort them which are in any trouble, by the comfort wherewith we ourselves are comforted of God Posterboy by God’s Grace, Addendum: This Posterboy blog post is/was to encourage you to be tested for a B-Vitamin deficiency… but I betting you won’t test low…but I hope and pray you will get tested...to see if (it) is happening...and if you only needed a test to diagnose you...why wouldn't you do it...even a low normal test can be helpful to guide you...in your journey back to health....right now I am low normal in Vitamin D...but I didn't know until I got tested... See this Hormones Matter blog post about why most people (even when low in Thiamine) will test normal… http://www.hormonesmatter.com/thiamine-deficiency-testing-understanding-labs/ the same is true for Riboflavin (and Niacin often) as well….depending on the factor you used in the test … a deficiency might show as being normal… see this study in the UK… https://www.ncbi.nlm.nih.gov/pubmed/19102813 factor’s have not (at the time of their test (yet)) been standardized to determine what constitutes a Vitamin deficiency (for many B-Vitamins)...so we guess often...(at least when it comes to B-2 aka Riboflavin) though we know what to test for... soooooo many people go undiagnosed……they (UK researchers) estimated as many as 1/3 of the (UK) population might have a “hidden” deficiency depending on the “factor” used to determine a Riboflavin deficiency….etc… Note: I can't tell how much a cow weighs by looking at it...I have to have it tested/weighed to see if my guess is accurate... and neither will you be able to "guess" what deficiency (if any) you have without being tested for them... I wish everybody well....I hope this is helpful but it is not medical advise. I must stop for now...but good luck and God speed on your continued journey...and if you do test low at least then you will know.... Posterboy,
-
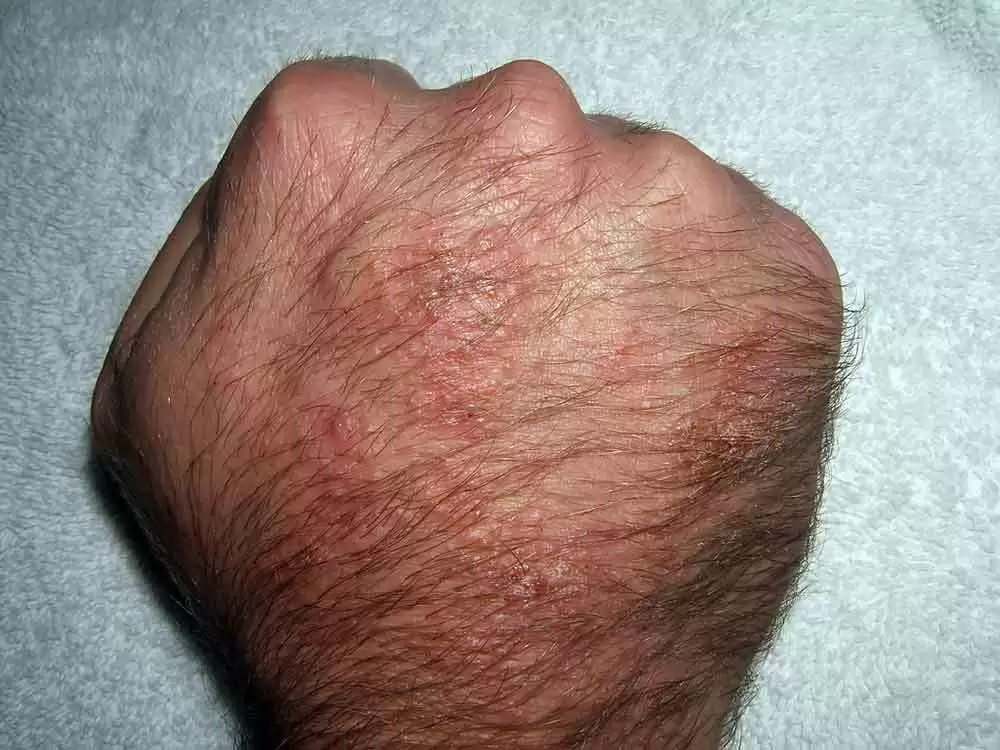
Celiac.com 11/20/2019 - Both atopic dermatitis and celiac disease are often accompanied by other immune-mediated disorders. A team of researchers recently set out to see if they could find a connection between atopic dermatitis and celiac disease in a broad community-based population. The research team included Guy Shalom, Khalaf Kridin, Keren-Or Raviv, Tamar Freud, Doron Comaneshter, Rivka Friedland, Arnon D. Cohen, and Dan Ben-Amitai. The team conducted a cross-sectional observational design, in which they collected demographic and clinical data for patients enrolled in a large health management organization who were diagnosed with atopic dermatitis by a dermatologist in 2002–17. They recorded presence of celiac disease and celiac-related morbidities for the entire group, for adults over 18 years old, and for adults with moderate-to-severe atopic dermatitis. They then compared the findings with a matched control group without atopic dermatitis. The study group included 116,816 patients, with a total of 45,157 adults, along with 1,909 adult adults with moderate-to-severe atopic dermatitis. Multivariate analysis showed that atopic dermatitis was associated with a significantly higher rates of celiac disease across the entire study population, and for each study group. The results showed a meaningful connection between atopic dermatitis and celiac disease, and demonstrate the need for timely screening of people with atopic dermatitis for gastrointestinal morbidities. Read more in the American Journal of Clinical Dermatology The researchers in this study are variously affiliated with the team of researchers recently set out to Clalit Health ServicesTel Aviv, Israel; the Division of Community Health, Faculty of Health Sciences, Siaal Research Center for Family Medicine and Primary Care Ben Gurion University of the Negev Beer-Sheva, Israel; the Department of Dermatology Rambam Health Care Campus, Haifa, Israel; the Pediatric Dermatology Unit Schneider Children’s Medical Center of Israel, Petach Tikva, Israel; the Chief Physician’s Office, Clalit Health Services Tel Aviv, Israel; and the Sackler Faculty of Medicine, Tel Aviv University, Tel Aviv, Israel.
- 11 comments
-
- atopic dermatitis
- celiac
-
(and 3 more)
Tagged with:
-
I have been living with a diagnosis of Celiac for 10 years and now also am type 2 diabetic. My question is: is there anyone else out there with these two conditions and how do they navigate making and buying and eating food for both conditions? Thank you for your help!
-
Celiac.com 11/13/2019 - After not eating much all day, and receiving free alcohol at the bar he was playing, Finley Quaye, a Brit award-winning singer with celiac disease, started a row, punched a bartender and threatened to stab people. Scotland-born Quaye, 45, of Earls Court in London, is best known for his album Maverick A Strike in the late 1990s. The singer, who has celiac disease, had not eaten much the day of the attack, and was given free alcohol by the club he was playing. He had been performing at Troubadour on the Old Brompton Road, and enjoying free booze throughout the evening, as a perk for singing at the club. Judge Michael Snow of Westminster Magistrates’ Court heard testimony that Quaye had asked bar manager Robert Jenei to search for a female companion’s handbag after the pair had left the venue at around 1.30 am. But after returning without the bag, Jenei found Quaye visibly angry. Quaye began making threats to security staff, before punching Jenai in the face. The court heard Quaye then kicked a car belonging to security staff, before shouting “I will stab you lot in the kidney” and “I will stab you in the windpipe.” After pleading guilty to assault for punching and threatening to stab Jenai during the unprovoked attack, Quaye has now been ordered by a judge to perform 200 hours of unpaid work. When questioned by police the next day Quaye said he had drunk a lot of alcohol on an empty stomach and had no memory of punching Jenei. Quaye had been given free drinks as a bonus for performing at the bar. At Quaye’s sentencing on Monday, Defense attorney Shahnaz Sargent cited the free alcohol in Quaye's defense. She added that he had not drunk much water and, had not eaten anything all day "because he suffers from celiac disease." The court also heard about Quaye's previous convictions for offenses including battery and public disorder going back to 2012. Through his lawyer, Ms Sargent, Quaye said that he has "made a determined effort to address his problems with alcohol and drugs.” Ms Sargent added that Quaye had been attending addiction services, adding: “He’s very sorry for the way he behaved towards Mr Jenei.” Ultimately, Quaye received a sentence of 200 hours of unpaid work and a rehabilitation order from Judge Michael, who said: “What makes this offense serious is the level of culpability involved...before the punch you made considerable threats that would have caused significant fear, then you punched this man in the face.” Did lack of eating, due to celiac disease, play a role in an outburst by Brit Award-winning singer, Finley Quaye, which led to attack on a bartender? Possibly. Of course, not eating due to celiac disease is no excuse for Mr. Quaye's behavior, for which he rightly faced legal consequences. However, anyone who's ever found themselves hungry, but with no good gluten-free options, might understand how easily anger and rage can manifest, and how quickly things can spin out of control, especially if alcohol is involved. As many celiacs know, it never hurts to have a bunch of gluten-free snacks on hand, especially if you're going to be someplace with restricted gluten-free food options. Luckily for Mr. Quaye, no one was seriously hurt. Hopefully, the results of Mr. Quaye's legal case will lead him to better manage both his drinking, and his celiac disease. Have you or anyone you know ever been stranded without gluten-free food and had a meltdown? Feel free to share your stories in our comments section below. Read more at BBC.CO.UK
-
Celiac.com 11/07/2019 - Despite major improvements in awareness and testing, it can still take years to get a proper celiac disease diagnosis, in part because other diseases can cloud the issue. Often, doctors suspect, or even diagnose, other diseases before the patient's celiac disease is revealed. It’s easy for doctors, and even patients, to simply stop with one of these other diagnoses, causing unnecessary delays in a celiac diagnosis. Celiac disease is often confused for one or more of these twenty-one diseases. In many cases, patients can get one or more diagnoses for these conditions before finally being diagnosed with celiac disease. People with one or more of these conditions might want to get screened for celiac disease, especially if they have any celiac-related symptoms. Here are twenty-one diseases commonly suspected or diagnosed before celiac disease is discovered: ALLERGIES Many people find themselves wrongly diagnosed with environmental allergies long before they are diagnosed with celiac disease. CANKER SORES Study data published in BMC Gastroenterology indicate that aphthous stomatitis, commonly called canker sores, can be the sole symptom for about one in twenty people with celiac disease, so it makes sense to perform celiac screening these people. Anyone with canker sores and any of the myriad symptoms of celiac disease would be advised to check for celiac disease. LACTOSE INTOLERANCE Lactose intolerance is a common condition. In some cases, people discover their lactose intolerance after their celiac diagnosis. That’s because mucosal damage from gluten can leaves celiac patients unable to digest lactose. This can last until the gut fully heals, and many different foods may trigger adverse symptoms until full healing occurs. Some people see their lactose intolerance improve and even vanish after adopting a gluten-free diet. Probably, their gut is healed thoroughly enough that they no longer react. However, if you suspect celiac disease and are diagnosed with lactose intolerance, then consider pressing for a celiac disease screen, just to be sure. Especially if you still have symptoms after going dairy-free. IBS/IBD It’s been recently reported that celiac disease is uncommon in people with irritable bowel syndrome, so there's no need for routine celiac testing in IBS patients. However, for a proper diagnosis of IBS, it’s important to first rule out the presence of celiac disease. For this reason, anyone suspecting IBS should get checked for celiac disease, just to be sure. MENTAL ISSUES Many people with celiac disease suffer from mental issues, or psychiatric disorders such as anxiety and depression. We also know that a gluten-free diet can help to relieve some symptoms of schizophrenia. In some cases, especially in those without classic celiac symptoms, these psychiatric disorders can be among the few symptoms, and can make celiac disease difficult to diagnose. Moreover, many doctors attribute symptoms of celiac disease to psychosomatic causes. That is, they think it’s all in the patient’s head. Anyone who suffers from mental health issues along with celiac disease symptoms should probably get checked out for celiac disease. THYROID DISEASE Thyroid disorders are common in people with celiac disease. People with celiac disease have much higher rates of autoimmune thyroid disease than the regular population. For this reason, anyone diagnosed with autoimmune thyroid disease should be screened for celiac disease just to be sure. GALLBLADDER DISEASE It is not uncommon for people with celiac disease or gluten intolerance to have their symptoms attributed to gall bladder disease. Occasionally, this can lead to removal of the gall bladder, which may not result in symptom improvement. Anyone with celiac-associated symptoms who receives a diagnosis of gall bladder disease might want to get screened for celiac disease, just to be sure. AMOEBA/PARASITE/INFECTION Celiac disease symptoms can mirror symptoms of certain gut parasites, which is one reason that many people with celiac disease find themselves being checked for parasites long before they get checked for celiac disease. COLITIS/SPASTIC COLON Another common culprit for misdiagnosis is colitis, which shares many symptoms with celiac disease. Similarly, many people who actually have celiac disease find themselves with a diagnosis of “spastic colon.” ACID REFLUX/GERD People with GERD don't have any higher rates of celiac disease than the rest of the population. However, to be fair, a pretty high percentage of newly diagnosed celiac patients have reflux and/or esophageal dysmotility; which might explain the high prevalence of reflux symptoms in celiac disease patients, and the common misdiagnosis of GERD. If your symptoms persist, consider getting checked out for celiac disease. PSYCHIATRIC DISORDERS In many cases, celiac disease symptoms can be so hard to pin down that doctors find themselves wondering if the symptoms aren't really in the patient's head. In their quest for diagnosis, many people with celiac disease have been referred to a psychologist, rather than evaluated for celiac disease. CHRONIC FATIGUE For these reasons, it’s important for patients diagnosed with anemia, especially unexplained anemia, to be checked out for celiac disease. Also, anyone with unexplained fatigue might want to press their doctor for a celiac disease screen. Many people with celiac disease report recurrent fatigue as one of their symptoms. Sometimes, fatigue can be one of the few or only symptoms, making celiac disease difficult to diagnose. Fatigue can be caused by low-iron, which can be a sign of anemia. Often, though, doctors simply diagnose anemia as the cause of the problem, rather than seeing it as a potential sign of celiac disease. WEIGHT GAIN Classic celiac disease patients commonly suffered weight loss or low body weight. That has changed. These days, it is much more common for patients with normal or high BMI to have celiac disease. There’s also some evidence that obesity plays a major role in triggering autoimmune disease. For these reasons, physicians should not discount the possibility of celiac disease based solely on BMI. Screening Versus Symptoms: Does Detection Method Affect Body Mass For Celiacs on a Gluten-Free Diet? How can I be overweight with Celiac? CYSTIC FIBROSIS Cystic fibrosis is another disease with some symptoms, such as big appetite but poor weight gain, and bulky, smelly, greasy bowel movements, that can sometimes be blamed for celiac disease. Rates of celiac disease are about triple for patients who also suffer from cystic fibrosis, compared to those without cystic fibrosis. That’s why it’s important that people diagnosed with cystic fibrosis receive a screen for celiac disease. DIABETES Numerous studies have shown connections between celiac disease and diabetes. In fact, researchers have found that celiac disease often precedes Type 1 diabetes in children with both conditions, and that up to 10% of children with Type 1 have clinical celiac disease. For this reason, it’s a good idea for people with diabetes to be screened for celiac disease, especially if they are suffering any type of celiac-associated symptoms. STRESS Also, there’s some evidence for a strong correlation between childhood stress and trauma, and the presence of celiac disease in adults. Being diagnosed with a stress-related disorder, such as post-traumatic stress disorder, acute stress reaction, adjustment disorder, and other stress reactions, was significantly associated with an increased risk of autoimmune disease, compared with matched unexposed individuals. For these reasons, it’s important for people with celiac-like symptoms, who receive a diagnosis of stress, to be checked out for celiac disease. ANEMIA We also know that doctors are likely primary care physicians are likely under-testing for celiac disease in patients with iron deficiency anemia. For these reasons, it’s important for patients diagnosed with anemia, especially unexplained anemia, to be checked out for celiac disease. We know that celiac disease is common in cases of unexplained iron-deficient anemia. Read more on Anemia and Celiac Disease VIRUS (VIRAL GASTROENTERITIS) Another very common thing doctors suspect long before they suspect celiac disease, is viral gastroenteritis. CANCER/LYMPHOMA Certain types of cancer and/or lymphoma are strongly associated with celiac disease. For example, patients with celiac disease over five years showed higher rates of non-Hodgkins lymphoma, small-intestinal cancer, colon cancer, and basal cell carcinoma of the skin. That’s why it’s important for people with such types of caner/lymphoma be screened and evaluated for celiac disease. SKIN CONDITIONS Having celiac disease can leave people at much greater risk for various skin conditions. People diagnosed with one of the following seven skin conditions commonly associated with celiac disease might want to consider getting checked out for celiac disease. PELLAGRA Pellagra is a disease caused by low levels of niacin, also known as vitamin B-3. It's marked by dementia, diarrhea, and dermatitis, also known as “the three Ds.” Because the symptoms of diarrhea and skin rash are similar, pellagra can be mistaken for celiac disease. Pellagra is easily treated with niacin supplements, but it's crucial that it is treated, otherwise it can be fatal. The two conditions can also co-exist, so anyone who is receiving enough niacin, but still presents celiac-like symptoms should likely be checked out for celiac disease.
- 13 comments
-
- celiac
- celiac disease
-
(and 3 more)
Tagged with:
-
To All, No more doughnuts brought up the topic of Lectins today so I thought I would start a topic on it. Here is the research I am aware of ...20 years ago...it was controversial enough then to get a doctor fired over discussing this theory... https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1115436/ It doesn't mean he was right...but it was concerning enough people felt unsettled/threatened over this topic....I would like to hear the forum members opinions...about whether he was right or not??? it would explain the cross contamination issues of eating things other than gluten that might be causing/mimicking a gluten reaction like someone who can't tolerate corn for example...celiac.com has done articles on this topic but some people might feel like commenting on an article ...that might more at ease discussing it as part of thread on related disorders/or further/other celiac research.... Posterboy,
-
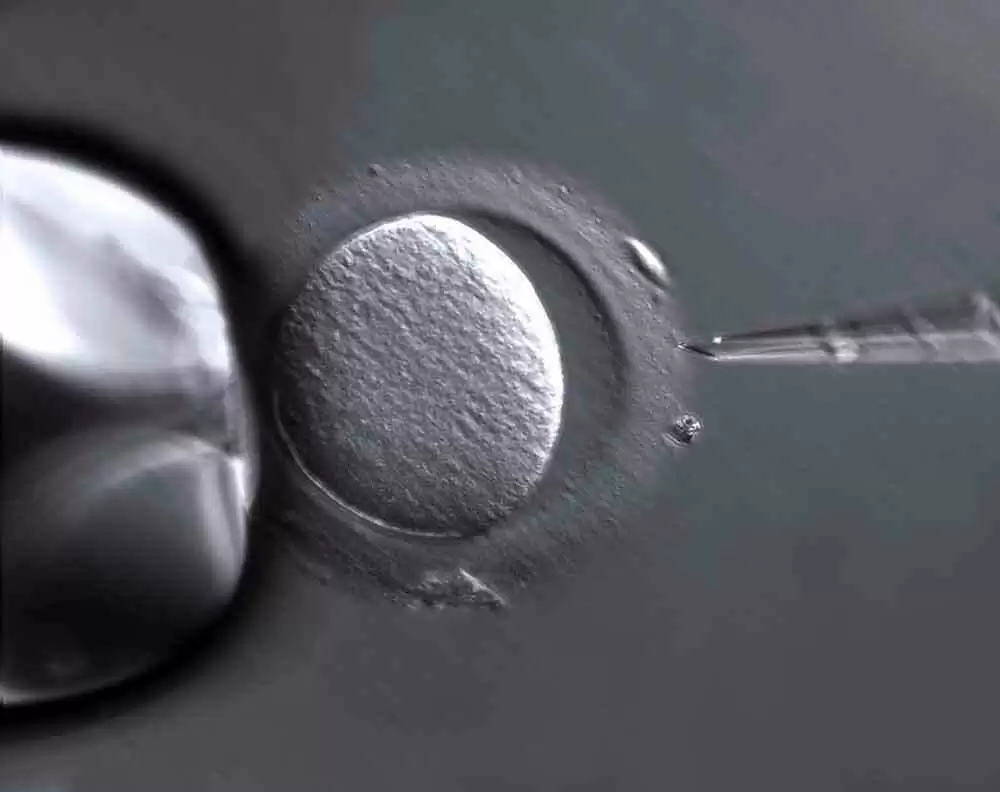
Celiac.com 11/05/2019 - After failing to conceive naturally over several years, the woman, Helen Tzouganatos, turned to IVF doctor Professor Mark Bowman. Tzouganatos says she and her husband had "tried every fertility trick in the book – expensive ovulation kits, herbal remedies, acupuncture, eating more of this and less of that, taking a holiday, taking another holiday – and nothing worked." During her intake, Tzouganatos told Dr. Bowman that she had no "serious" health issues just unexplained anemia since childhood, abdominal cramps and lactose intolerance. To his credit, Dr. Bowman immediately suspected she was a celiac. He ordered a celiac blood screen. When the results came back positive, everything became clear. "You’re a celiac and that is why you’re infertile," Dr. Bowman told her. "You need to cut gluten immediately.” Tzouganatos began a gluten-free diet immediately, and, after six rounds of IVF treatment, she conceived her son Vasili, followed by a daughter, Sofia, conceived on the second frozen embryo transfer 17 months later. Statistical data indicate that one in 70 Australians have celiac disease yet 80 per cent are undiagnosed. Tzouganatos is lucky that her celiac disease was discovered quickly by her IVF doctor, after sneaking under the radar for so long. Any women experiencing unexplained infertility, especially in conjunction with other celiac-related symptoms should be screened to rule out celiac disease. Quick adoption of a gluten-free diet can often lead to full healing and normal, or greatly improved fertility. Read more at SMH.com.au
- 1 comment
-
- celiac
- celiac disease
-
(and 5 more)
Tagged with:
-
Celiac.com 10/30/2019 - More and more, doctors are noticing cases of both celiac disease and eosinophilic esophagitis (EoE) in children. A team of researchers recently set out to examine the results of therapeutic dietary treatment in a group of children with celiac disease and eosinophilic esophagitis. The research team included Tiffany Patton; Ankurt Chugh; Leena Padhye; Catherine DeGeeter; and Stefano Guandalini. They are variously affiliated with the Section of Pediatric Gastroenterology, Hepatology, and Nutrition, Comer Children's Hospital, University of Chicago Medical Center, Chicago, IL; the Section of Pediatric Gastroenterology, Hepatology, and Nutrition, Medical College of Wisconsin, Milwaukee, WI; the Division of Allergy and Immunology, Rush University Medical Center, Chicago, IL; and the Section of Pediatric Gastroenterology, Hepatology, and Nutrition, Stead Family Children's Hospital, University of Iowa, Iowa City, IA. For their assessment, the team reviewed patient records obtained from the University of Chicago Celiac Center Database from August 2008 to July 2013. The researchers collected information on children with both celiac disease and eosinophilic esophagitis including age, sex, dates of diagnoses, presenting symptoms, length of symptoms before diagnosis, family and personal history, dietary therapy, and esophageal response to dietary treatment. The team reviewed records of 350 pediatric celiac disease patients. Twenty-two children, or 6.3% had confirmed celiac disease and eosinophilic esophagitis, 17 of those children had repeat biopsies. In four cases, the esophageal eosinophilia cleared up on a strict gluten-free diet, 10 of 17 (59%) needed to eliminate other foods before the problem resolved, 1 of 17 failed to reached histological remission, while there was no follow-up information for 2 of those 17 patients. After symptom improvement, five out of five patients could tolerate soy, three of five could tolerate eggs, three of seven could eat dairy, two out of four could tolerate nuts 2 of 4, and two of four can tolerate fish. This is perhaps the largest pediatric study to examine the histologic aspects of EoE-associated esophageal eosinophilia in response to dietary treatment of pediatric patients with both celiac disease and eosinophilic esophagitis. The results show that most of these patients can tolerate soy, and suggest that making it the first food to be reintroduced, or testing out a soy-inclusive elimination diet could be helpful for those patients. Read more in the Journal of Pediatric Gastroenterology and Nutrition: August 2019.
-
Celiac.com 10/28/2019 - Among other things, a recent study on nutrition and bone health in adults with probable undiagnosed, untreated celiac disease drives home the importance of early diagnosis and quick adoption of a gluten-free diet. The importance can be seen in the findings of a research team that recently looked at variations in nutritional intake of calcium, vitamin D, and phosphorus; their levels in the blood; and bone health in adults with and without likely, undiagnosed celiac disease. The research team included Lara H. Sattgast, Sina Gallo, Cara L. Frankenfeld, Alanna J. Moshfegh, and Margaret Slavin. They are variously affiliated with the Department of Nutrition & Food Studies, George Mason University, Fairfax, Virginia, USA; the Department of Global & Community Health, George Mason University, Fairfax, Virginia, USA; and the Food Survey celiac diseases Research Group, Agricultural Research Service, U.S. Department of Agriculture, Beltsville, Maryland, USA. The team analyzed data from 48 adults with likely undiagnosed celiac disease and positive immunoglobulin A endomysial antibody tests, and 13,634 controls. The data came from What We Eat in America and the National Health and Nutrition Examination Survey 2009–2014, and included self-reported information on dietary and supplement intake from a single day of 24-hour recalls, serologic indicators, and dual x-ray absorptiometry images. The team's statistical analysis included multiple linear regression modeling controlled for age, sex, race/ethnicity, energy intake, and poverty income ratio. Rates of likely undiagnosed celiac disease were 1 in 285. Patients with likely celiac disease showed an average 251.6 mg higher daily total calcium intake, higher dairy consumption by 0.7 cups per day, and higher serum phosphorus levels. Probable celiac patients showed a substantially higher total dietary and supplement intake measured in calcium density and phosphorus density. The researchers saw no differences in serum calcium, vitamin D, or alkaline phosphatase levels between the groups. Patients with likely celiac disease were associated with lower femur bone mineral density (BMD) and a lower femoral neck BMD, but showed no difference in total spine BMD. This is one of the first studies to examine variations in nutritional intake of calcium, vitamin D, and phosphorus; their levels in the blood; and bone health in adults with and without likely, undiagnosed celiac disease. Adults with probable undiagnosed celiac disease had lower bone density than those without celiac disease, even though they reported higher calcium intake and nutritional density of calcium and phosphorus. Among other things, the variations in BMD in this study demonstrate the importance of early diagnosis and the rapid adoption of a gluten-free diet for patients with undiagnosed celiac disease. Read more in the J Am Coll Nutr. 2019 Jul 19:1-10.
- 1 comment
-
- adult
- bone health
-
(and 7 more)
Tagged with:
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8-M):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8-M):