-
Welcome to Celiac.com!
You have found your celiac tribe! Join us and ask questions in our forum, share your story, and connect with others.
-
Celiac.com Sponsor (A1):
Celiac.com Sponsor (A1-M):
-
Get Celiac.com Updates:Support Celiac.com!
Search the Community
Showing results for tags 'negative'.
-
Celiac.com 01/24/2023 - As with many studies sponsored by well-intended disease support groups, a recent qualitative study claims to link negative media portrayals of celiac disease with negative impacts upon people with celiac disease. However, the study, though well-meaning, is deeply flawed, and its conclusions are suspect. The study sets out to answer an important question: Is negative media coverage about celiac disease having a negative effect on people with celiac disease and gluten-intolerance? The problem lies in the methods used to gather information, the questions asked or not asked, and the conclusions drawn from that information. Researchers Satvik R. Verma and Manpreet Bains set out to describe and analyze the nature of the media coverage of celiac disease. They are affiliated with theTrauma and Orthopaedics, Kingston Hospital in London, and the Faculty of Medicine & Health Sciences, University of Nottingham in Nottingham, GBR. To begin, they commissioned a document analysis of local and national UK newspaper articles over three weeks, from May 2nd to May 22nd, 2016, ensuring coverage of articles from Coeliac Awareness Week. The team used Kantar Media of London to collect articles that used celiac disease-related language, and analyze them using a combination of thematic and content analysis techniques. They then used "an inductive approach" to code articles into themes, and to present frequency data. They included a total of four hundred eighty-eight articles in the analysis, with 233 in week one, 117 in week two, and 138 articles in week three. Articles exhibited one of six overarching themes: events around Awareness Week and food content noted as gluten-free (gluten-free); raising awareness; encouraging people to seek help; and other health implications and perceptions of celiac disease and the gluten-free diet, of which a significant proportion consisted of articles by Coeliac UK. They found both positive and negative articles. They noted that the number of negative newspaper articles rose sharply during Coeliac Awareness Week, with instances of negative articles rising in week one, and even more sharply in week three. From this information, they concluded that "mixed messaging" negatively impacted the potential and current patients with celiac disease, especially in relation to gluten-free diet adherence and diagnosis rates. The problem is that they don't have any actual data. They are simply saying that they found some negative articles and then concluded that those negative articles "negatively impacted the potential and current patients with celiac disease, especially in relation to gluten-free diet adherence and diagnosis rates." The conclusion sounds serious: Namely, that negative articles about celiac disease and gluten-intolerance are having negative effects upon people with celiac disease. Data Don't Support the Conclusion Based on what? Because they don't offer any data, even anecdotal, about the effects of these articles on people with celiac disease, they don't even seem to have a good correlation argument, let alone a causation argument. It's possible that this is true, but they need a great deal more data to prove their case. Right now, they're stuck with saying: we found a bunch of negative articles on celiac disease, and we THINK those are having a negative effect on people with celiac disease. But they offer no solid evidence to support that conclusion. They call this a qualitative study, but try to slip in a quantitative conclusion. That is, if they want to say that a certain number of people are affected in a certain way by negative celiac articles, then they need to do a better job of quantifying the effect. How many people are affected by negative celiac coverage? How are they affected? What's the damage? Without better methodology, and better data, this study simply fails to provide any clear picture of the supposed damage done to people with celiac disease, or even the exact nature of the "negative" coverage. Studies like this may sound important, and my even seem to show something, but they are deceptive. By simply assuming their conclusion, the study does no one any favors. Why Does it Matter? The study simply fails to prove that "negative" articles during Celiac Awareness Week translate into actual harm to people with celiac disease and gluten-intolerance, and even though this conclusion may seem self evident, a properly done study would not jump to this conclusion. To be meaningful, the study needs to do more to both describe the "negative" articles, and to clearly document their affect on people with celiac disease and gluten-intolerance. And it must, at some point, link the two with solid quantitative, not qualitative data. Read more at Cureus 14(12): e32444.
-
- articles
- celiac disease
- (and 5 more)
-
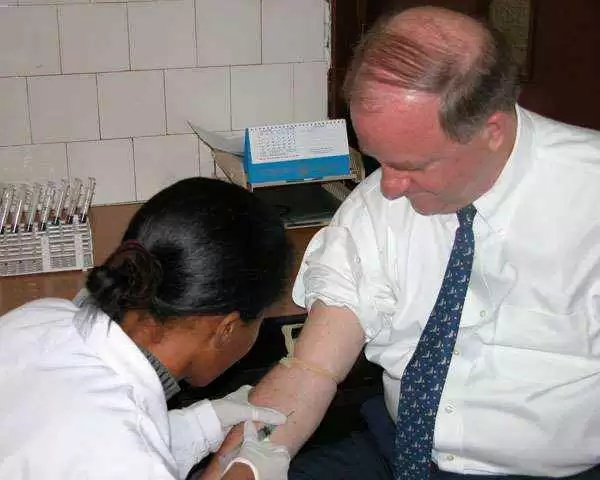
Celiac.com 08/15/2022 - In a significant finding, a celiac disease registry at University of Alabama reveals significant issues in accurately testing Black people for celiac disease using the TTG antibody test. The new registry of celiac disease patients at the University of Alabama at Birmingham is the work gastroenterologist Dr. Amanda Cartee, MD, and fellow colleagues at UAB. Among the most important findings, the registry reveals that Black people with biopsy confirmed celiac disease are exponentially more likely than non-Hispanic whites to show negative results on the most common diagnostic celiac disease blood test. For people with celiac disease, a positive TTG antibody test is the most common path to an endoscopy and biopsy to confirm or negate celiac disease. For most people with celiac disease, especially non-Hispanic whites, a positive TTG test is highly predictive of celiac disease, hence the routine endoscopy and biopsy to follow-up a positive test. In fact, less than ten percent of non-Hispanic whites with biopsy-proven celiac disease have a "negative" TTG test. However, according to the registry data, high percentages of Black people with celiac disease are testing negative for TTG antibodies, and so being denied a swift and properly diagnosis, simply because they never meet themes common threshold for biopsy. It's the TTG threshold currently used to determine the definition of positive and negative TTG that might just be at the heart of the problem. That's because the numbers are nearly reversed for Black people. While less than ten percent of non-Hispanic whites with celiac disease show negative TTG results, the registry data shows that a whopping eighty percent of Black people with biopsy-proven celiac disease have a "negative" TTG test. The means that these folks were unlikely to have gotten a biopsy as quickly as someone with a positive TTG test. It also means they may have had to suffer longer, and/or self diagnose. And those facts are also borne out by the registry data, which point to longer times to diagnosis and less biopsy-driven diagnoses for Black celiac patients. Black patients were also much less likely to have received genetic testing for celiac-associated genes. There is limited data on celiac disease and Black people, said Dr. Cartee, noting that only a single study with the primary goal of investigating the clinical characteristics of celiac disease and Black people has been done. While the registry revealed differences in TTG test results and BMI, it showed similarities in celiac disease diagnosis for non-Hispanic white and Black patients. These included symptoms as the primary cause for testing, length of time to diagnosis, and a diagnosis that did not include recommended blood tests and a biopsy. Basically, the data show that TTG tests will be negative in the vast majority of Black patients with biopsy-proven celiac disease. That means further study is needed to determine whether the TTG test is useful for Black patients, and more research needs to be done to figure out how to make sure they can get quickly and properly diagnosed. Stat tuned for more on this and related stories regarding celiac disease testing, screening, and diagnosis in Black people, and in other ethnic populations. Read more about the celiac registry data and findings presented by UAB gastroenterologist Dr. Amanda Cartee, MD, at Digestive Disease Week.
-
Celiac.com 12/28/2021 - Social media algorithms are pushing potentially inappropriate content featuring thin bodies on people with celiac disease who are just searching for gluten-free food as a way to stay healthy, not to lose weight. This is just one scenario among many, in which social media companies are profiting by pushing potentially harmful content toward users making innocent searches for unrelated material. In the above scenario, the content topics quickly move from general weight loss and thinness to sites and content that glorifies eating disorders. If this seems scary in its implications, it is. If it seems rare, it is not. The scenario is drawn directly from the experience and documentation presented by former Facebook product manager, Frances Haugen, during her testimony before the Senate Commerce subcommittee in October 2021. Haugen explained that not only do Instagram’s algorithms routinely push teenagers toward potentially dangerous and unhealthy topics, but Facebook knows this and disregards expert advice to make the platform safer, chiefly due to greed, says Haugen. “Facebook knows its engagement ranking on Instagram can lead children from very innocuous topics like healthy recipes, to anorexic content over a very short period of time,” Haugen said during her testimony. As part of her testimony, Haugen handed over internal documents to numerous media outlets. Haugen's documents and testimony strongly support her claims that, during her time at Facebook, she regularly experienced “Facebook choosing to prioritize its profits over people." Facebook researchers found that more than 2 out of 3 teenage girls and 2 out of 5 of teenage boys confront negative social comparisons on Instagram. Data also shows that more than half of teen girls experience negative social images and messaging about beauty standards, which can trigger negative self esteem and body dysmorphia. According to Haugen, Facebook understands the importance of drawing young people onto its platforms in order to expand and monetize. “They know that children bring their parents online,” she said. Have you encountered offensive, or potentially dangerous content related to searches for gluten-free food, or celiac disease? Share your experience in the comments below. Read more fun the Daily Free Press
-
Celiac.com 10/02/2021 - Faced with what she calls a "vindictive" gluten-free patron, who "tried to get them shut down with Facebook witch hunt," the owner of a small cafe in Cornwall is fighting back. Emma Price, who co-owns The Lighthouse café in Mevagissey, Cornwall, says the problem began when her staff informed the female patron that they could not guarantee their ingredients were completely free of gluten to be safe enough for a person with celiac disease. Despite café staff being clear and honest with the woman, and putting "customer safety above their profits," Emma claims the woman became angry and later took her complaints to a Coeliac group on Facebook, where she exhorted its tens of thousands of members not avoid the café. After discovering the harsh comments, Price later learned that the customer even reported Emma's café to local authorities, when she received an inspection visit from the local supervisory authority, called Trading Standards, during a busy lunch rush. Despite the inspection finding no breach of any rules and regulations, Emma says the incident has left her feeling "extremely upset" and "vulnerable." She decided to share the cafe's ordeal in an effort to encourage people to consider the potentially negative effects such "vindictive" and "untrue" reviews or comments can have on a small business. "The problem with Facebook is that people can say what they want, then there's this huge pile-on of people who have never visited our café, never looked at our products and had never spoken to us yet threatened us with physical violence...It makes you feel quite vulnerable and you know it's not just us working in the café," says Price. Eating gluten-free at restaurants can be challenging and stressful for people with celiac disease. However, very few, if any, restaurants anywhere will absolutely guarantee that a given meal is 100% gluten-free. The best most places can do is to repeat the measures they take in sourcing the ingredients, and preparing the food. Guarantees carry legal implications, and are practically unheard of, even in establishments that reliably offer gluten-free menus. If the owner of a restaurant is honest and let's you know that they can't guarantee that your food will be gluten-free, you should thank them for their honesty rather than to take revenge. Read more in Walesonline.co.uk
-
Celiac.com 11/05/2012 - Over the last 40 years, studies have shown higher rates of menstrual abnormalities and pregnancy complications among women with celiac disease. However, the data from these studies have been inconsistent, and inconclusive regarding the actual effects of celiac disease on female fertility. To get a better picture of the relationship between celiac disease and female fertility and pregnancy, researchers recently conducted a more comprehensive study. The research team was led by Stephanie M. Moleski, MD, of Thomas Jefferson University Hospitals in Philadelphia. Dr. Moleski presented an abstract of the study data at the American College of Gastroenterology Annual Meeting 2012. In the abstract, she points out that women with biopsy-proven celiac disease had significantly higher rates of fertility and pregnancy complications and gave birth to less children than those without the disease. Because it is an abstract, the study data and conclusions should be regarded as preliminary until they appear in a peer-reviewed journal, where they can be given a fuller context and be more widely scrutinized. For their study, Dr. Moleski and her colleagues recruited patients treated for celiac disease at Thomas Jefferson University Hospitals, as well as members of the National Foundation for Celiac Awareness and the Gluten Intolerance Group, to respond in an anonymous Internet-based survey about fertility and pregnancy. Women without celiac disease also completed the survey and served as a control group. The survey included questions about celiac diagnosis and history, menstrual history, fertility, spontaneous abortions, and pregnancy outcomes. Approximately 1,000 women who completed the survey. Of those, 473 had physician-diagnosed celiac disease, while 298 women had the been confirmed for celiac via small-bowel biopsy. The researchers used the group with biopsy-proven disease to compare against 560 women without celiac disease. The data showed that 41.2% of women with celiac disease had increased difficulty conceiving compared with 36.5% of control subjects (P=0.03). Women with celiac disease also had more consultations with fertility specialists and higher rates of spontaneous abortion, preterm delivery, and cesarean section, compared with control subjects. Additionally, women with celiac disease were shown to have a shorter duration of fertility, to have a later onset of menarche and be younger when they experienced menopause, said Dr. Moleski. The data also revealed important differences between women with and without celiac disease. In all, 22.4% of women with celiac disease had consulted with fertility specialists, compared with 19% of those without (P=0.04). Also, 43.3% of celiacs had a history of spontaneous abortion, compared with 36.6% of non-celiacs (P=0.02). Compared with the control group of non-celiacs, women with celiac disease also had higher rates of cesarean delivery, 26.4% versus 23.8% of non-celiac women. Lastly, rates of preterm delivery were 23.2% for celiac women, and 14% for those without celiac disease (P=0.007), while the group with celiac disease was was also slightly older at the onset of their first period (12.7 versus 12.4 years, P=0.01). Among women reporting a history of spontaneous abortion, more than 80% of miscarriages occurred prior to diagnosis of celiac disease, said Dr. Moleski. She concluded that the retrospective analysis done by her team shows a clear relationship between celiac disease, fertility, and pregnancy outcomes, and suggests that the results demonstrate "a need for increased awareness of this association among patients and physicians." Sources: Medpagetoday.com American College of Gastroenterology, 2012; Moleski SM, et al "Infertility and pregnancy outcomes in celiac disease" ACG 2012; Abstract 15.
- 1 comment
-
- celiac
- celiac disease
- (and 6 more)
-
I had a rant here about 3 months ago after I received the results of my own biopsy, and was advised to go gluten free anyway, which I still haven't done but I'm experimenting with foods and hope to be gluten free soon. I wanted to come here and ask your advice again, because my dad had a biopsy about 4 weeks ago, the results of which came today, and I am so surprised to read they're negative. They told him it was very likely that he had celiac because his blood test was transglutaminase positive. He has low iron, low vitamin D, reflux, and his long-term symptoms of M.E/Chronic Fatigue Syndrome which I know are also common symptoms of celiac. Everyone was sure he might have it, so I don't understand why his biopsy was "normal with no evidence" of the disease. The letter does however suggest further blood tests to see if he might develop celiac disease in the future. If his immune system is attacking and it's showing in his blood, doesn't that mean he's already developed it? Why would it do that if he didn't have celiac going on now? I've been encouraging him to try gluten free bread and biscuits but he's been reluctant, now he definitely won't. Should he? Or should he wave the whole thing off and continue eating his sandwiches like he did quite happily today? I guess they will tell him at the appointment. It's just so ridiculous because after he eats wheat he gets reflux! I was also counting on his results being positive... Sorry I'm rehashing my story now, but since 2011 I've had severe, chronic reflux that has gotten worse with time and has remained a mystery after a barium, manometry and two endoscopies; IBS; light headedness/heavy/cotton wool head with brain fog; headaches and jaw pain; muscle pain and severe weakness; sensitivity to noise, light, and heat, also the sun; fatigue and crashing after activity; bone pain; also severe acne that only responds to antibiotics; dry and flaky skin; brittle, cracked and peeling nails; year-round allergies, like having a mild cold permanently; and the occasional mouth ulcer and bleeding gums. The absolute worst is the reflux, followed by the IBS and then my head. I haven't been able to spin in a circle for years. I can't dance. Can't exercise. I feel so dizzy and sick all the time. Can't bend over or lie down with the reflux. Have cut out all acidic foods and FODMAPS. I am underweight. The reflux doesn't allow me to drink much water now because it feels like I have a little ocean of acid/bile sitting in my esophagus and drinking just adds more to it. So my throat has been so dry for months now. Barium and endoscopy both showed acid/bile sitting there, and a hernia. Manometry presumably showed no reason for reflux like a problem with the wave or a loose LES. But my blood work was negative and then my biopsy was negative. I cried on my friend's shoulder when I got that letter, and I've been counting on dad's results since. Now... Now what? I haven't heard from the hospital in 3 months, since my results came back. I don't know if they're waiting to figure out my father before figuring out me, or if they've discarded me. They told me I'm difficult. So I'm looking for gluten free foods but it's difficult without medical support, and being the only one in the house that wants to be gluten free, cross contamination is going to be a constant threat. Just persuading them to have a second toaster is a battle in itself. (Gluten free pancakes are all very well, but not if I put them in that toaster!) Honestly, I'm at my wits' end. I haven't been healthy since 2011. I'm only 28. I don't remember what it feels like to not have reflux, acid, bile; to eat anything with no pain or gas or toilet trips; to spin in a circle or go to amusement parks; what it feels like to have a clear head. I avoid sunny days. This was all triggered and set off at the end of 2011 by panic attacks and a hospital stay. Oh, I forgot to mention that my stools are often pale, like beech furniture (that might be a strange comparison!). I've really just... had it. So I'm not really sure what I'm asking... should we both go gluten free despite negative biopsies? Or might we just have M.E/Chronic Fatigue Syndrome, which my dad was diagnosed with 18 years ago? Thank you for reading!!
- 6 replies
-
- biopsy
- chronic fatigue syndrome
-
(and 3 more)
Tagged with:
-
I'm not exactly sure what to do at this point if what I am reading is correct. I don't want to go into too much detail right off the bat but I can tell you more if needed. I had an allergy test done, they messed up the first time and did a small panel, but my Whey Allergin, IgG came back as 32.20. Ref range: 0-88.60 mcg/mL In the notes it says "values less than 2.00 mcg/mL represent absent or undetectable levels of allergen-specific IgG anitibody. Values 2.00 mcg/mL and above indicate progressive increases in the relative concentration of allergen-specific IgG." This is where my doctor sent back for a full 96 allergy test, but he was concerned about any cross-reactivity due to the Whey results so he requested a Celiac panel as well. Everything on the food allergies came back as negative, besides some environmental allergies that were already tested previously and noted before. Could you please tell me your thoughts on the results? I think they might be negative. But if so, what do I do now? Should I request some other testing? Let it go? I would love to get some relief though and find out what is wrong with me. I fell like I have many of the symptoms that have been attached with Celiac disease. Not that I'm saying I would like to be diagnosed with something but if I were diagnosed it would make my medical history make much more sense. If you would like more detail on symptoms I can outline them. For Gluten Allergen, IgG, Casein Allergen, IgG and Whey Allergen, IgG (The Whey was the one on the first set of tests though) it says "Request Credited -- ORDINC; Test ordered incorrectly" Here are the results for Celiac Disease Panel: IgA - Result - Sufficient Gliadin IgA Ab - Result - 10.3 -- Ref Range - 0.0-14.9 Tis.Transglut.Ab IgA - Result - <0.5 -- Ref Range - 0.0-14.9 the notes section is not helpful at all. And I guess they didn't do the IgG so should I be asking them to do that? The doctor has to send it to a different lab than the one they use due to insurance. Thank you all in advance!
- 2 replies
-
- blood test
- celiac
- (and 4 more)
-
Hello everyone I am new to the site but suspect I have something going on due to all my symptoms and so purchased a biocard home testing kit. I read the result before 10 minutes and it was negative. Before I went to bed I had an urge to look again and sure enough there was a red line showing positive. This was however after the 10 minute limit. My question is has anyone done a similar thing and gone on to receive a positive result from the dr? Many thanks for any help and advice.
-
Celiac.com 10/13/2017 - Tissue transglutaminase (tTG) immunoglobulin A (IgA) testing is a sensitive adjunct to the diagnosis of coeliac disease. The threshold for positivity was developed for diagnosis, with negative results reported as below the reference value (<4 U/mL). A team of researchers recently set out to investigate if an undetectable tissue transglutaminase IgA antibodies (tTG IgA<1.2 U/mL) is more predictive of healing compared to patients with negative but detectable serology (1.2-3.9 U/mL). The research team included H. Fang, K. S. King, J. J. Larson, M. R. Snyder, T. T. Wu, M. J. Gandhi, and J. A. Murray. They are variously affiliated with the Department of Medicine, the Division of Gastroenterology and Hepatology, the Division of Anatomic Pathology, the Division of Clinical Biochemistry and Immunology, the Division of Biomedical Statistics and Informatics, and the Division of Transfusion Medicine at the Mayo Clinic, Rochester, MN, USA. The research team conducted a retrospective study of 402 treated coeliac disease patients seen at the Mayo Clinic with negative tTG IgA values drawn within 1 month of duodenal biopsy between January 2009 and December 2015. The team used Corazza-Villanacci scores to assess mucosal healing, and logistic regression to assess the relationship of clinical variables with a normal biopsy. They also noted the presence of gastrointestinal symptoms. Their results showed that patients with undetectable test levels more frequently had normal duodenal histology, as compared with patients with detectable tTG IgA levels. Asymptomatic patients more often showed normal duodenal histology as compared to symptomatic patients. Patients with undetectable blood levels, and who followed a gluten-free diet for ≥2 years were more likely to have no villous atrophy, as compared to patients with detectable blood levels. Follow-up biopsies revealed that people recovering from celiac disease with negative tTG IgA serology showed that undetectable test levels are associated with normal histology. Source: AP&T
-
- antibodies
- celiac
- (and 11 more)
-
Celiac.com 06/29/2012 - A group of researchers recently set out to study cases of positive tissue transglutaminase antibodies with negative endomysial antibodies to determine whether or not such cases amount to celiac disease. The team included Thomas Hornung; Pavel Gordins; Clare Parker; and Nicholas Thompson. They are variously affiliated with the departments of Gastroenterology, and Immunology at the Northern Deanery of Newcastle upon Tyne, and with the department of Gastroenterology at Freeman Hospital in Newcastle upon Tyne in the UK. The most sensitive and specific blood tests for diagnosing celiac disease are those that detect immunoglobulin A (IgA) antibodies against human tissue transglutaminase (tTGA) enzyme, and those that measure aspects of connective tissue covering individual smooth muscle fibers, endomysial antibodies (EMA). Because of the high sensitivity (up to 98%) and high specificity (around 96%) reported for the tTGA assay, detection of tTGA is currently the primary blood test used in screening for celiac disease. The tTGA test also has a high negative predictive value approaching 100%, which makes it an excellent test for excluding celiac disease in both high and low risk groups. In contrast, positive predictive value of the tTGA test is rather poor with values between 28.6% and 60.2% being reported in several studies. EMA, on the other hand, has extremely high specificity values close to 100% and positive predictive value values approaching 80%.[5 10] However, compared with tTGA, EMA has lower sensitivity, usually under 90%. This being the case, the present standard celiac disease screening strategy is to first use tTGA, and then confirm positive results using EMA. However, doing it this way, doctors often end up with a group of patients who show divergent test results. For their study, the researchers wanted to gauge the percentage of patients with positive tTGA and negative EMA, but who were confirmed with celiac disease upon biopsy, and to identify factors in these patients that may help to increase diagnostic accuracy in such patients. The research team identified 125 consecutive patients with positive tTGA and negative EMA, who subsequently underwent endoscopy with at least two biopsies from the second part of the duodenum. The team charted any tTGA result over 15 U/ml as positive. They excluded any patients with known celiac disease at the time of testing. They then reviewed patient notes to assess indications for celiac disease serological screening, including the presence of iron deficiency anaemia, and symptoms such as diarrhea or weight loss, and family history of celiac disease. They defined diarrhea as a bowel frequency of more than three times a day. They then assessed histological evidence of celiac disease based on subsequent duodenal biopsies, plus Marsh grading. In cases where patient histology was unclear, they relied on the clinical assessment of a consulting gastroenterologist. Unclear histology included minimal/mild increase in intraepithelial lymphocytes of not more than 30 per 100 enterocytes and without villous atrophy, plus mild villous blunting with no increase in intraepithelial lymphocytes. They then categorized patients as either celiac disease negative, or celiac disease positive. Patients with no histological evidence of celiac disease on duodenal biopsies or equivocal histology plus overall clinical impression of celiac disease absence were categorized as celiac disease negative. Patients with histological evidence of celiac disease on duodenal biopsies or equivocal histology plus overall clinical impression of celiac disease presence were categorized as celiac disease positive. To measure IgA anti-tTGA antibody the team used a commercially available enzyme linked immunosorbent assay called Aeskulisa, manufactured by Aesku Diagnostics GmbH in Wendelsheim, Germany. To detect IgA anti-EMA with the standard immunofluorescent method, they used commercial slides of monkey oesophagus sections (Euroimmun, Euroimmun AG, Lübeck, Germany). They used conjugated sheep antihuman IgA as a secondary antibody, relying on a test manufactured by Instrumentation Laboratory UK Ltd., in Warrington, UK. Overall, the team categorized 113 patients (90.4%) as celiac disease negative. Of these, 102 patients had no histological features of celiac disease, while 11 patients had unclear histology plus an overall clinical impression of not having celiac disease. They categorized twelve patients (9.6%) as celiac disease positive. Of these, 10 patients had positive histology, and two patients had unclear histology plus an overall clinical impression of having celiac disease. Of those with positive histology, 17% were Marsh grade I, 8% were Marsh grade II, 33% were Marsh grade IIIa, 17% were Marsh grade IIIb and 25% were Marsh grade IIIc. Those with celiac disease were more likely to be older and to have a higher tTGA level. The groups showed no difference in any clinical parameter. Source: Frontline Gastroenterol. 2012;3(2):81-83.
- 2 comments
-
- antibodies
- assessing
- (and 9 more)
-
Celiac.com 06/27/2013 - Patients with villous atrophy and negative celiac disease serologies pose a diagnostic and therapeutic dilemma. When doctors are unable to determine what is causing villous atrophy in a patient without celiac disease, they usually classify it as a case of "unclassified sprue." However, doctors currently know very little about the best way to treat and manage cases of unclassified sprue. To get a better picture of this dilemma, a team of researchers recently examined the connections between villous atrophy and negative celiac serology. The research team included M. Degaetani, C.A. Tennyson, B. Lebwohl, S.K. Lewis, H. Abu Daya, C. Arguelles-Grande, G. Bhagat G, and P.H. Green. They are variously affiliated with the Celiac Disease Center, and the Department of Medicine at Columbia University College of Physicians and Surgeons at Columbia University Medical Center in New York, USA. For their study, the team looked at adult patients with biopsy-proven villous atrophy and negative celiac serology, evaluated at our tertiary referral center over a 10-year period. They noted test results for HLA DQ2/8 alleles, antienterocyte antibodies, giardia stool antigen, bacterial overgrowth, total serum immunoglobulins, and HIV. They also recorded treatment, response, and repeat-biopsy findings for each patient. They found that most of the 72 cases were classified as seronegative celiac disease, medication-related villous atrophy, and unclassified sprue. The majority of patients diagnosed with unclassified sprue reported symptomatic improvement with immunosuppressive therapy. Some patients diagnosed with unclassified sprue were found to have villous atrophy associated with the use of olmesartan. The team encourages further examination of the role of medications in the development of villous atrophy, along with the optimal dose and length of immunosuppression for patients with unclassified sprue. Source: Am J Gastroenterol. 2013 May;108(5):647-53. doi: 10.1038/ajg.2013.45.
-
Celiac.com 04/20/2010 - A team of researchers recently set out to determine whether new serology assays can detect gluten sensitivity among enteropathy patients seronegative for anti–tissue transglutaminase. Emilia Sugai, Hui Jer Hwang, Horacio Vázquez, Edgardo Smecuol, Sonia Niveloni, Roberto Mazure, Eduardo Mauriño, Pascale Aeschlimann, Walter Binder, Daniel Aeschlimann and Julio C. Bai comprised the research team. They are variously affiliated with the Small Bowel Section of the Department of Medicine at C. Bonorino Udaondo Gastroenterology Hospital in Buenos Aires, Argentina, the Matrix Biology and Tissue Repair Research Unit at the Cardiff University School of Dentistry in Cardiff, UK, and with INOVA Diagnostics, Inc., of San Diego, California. Some patients with celiac disease may not show a normal positive reaction to the test most commonly used for IgA anti–tissue transglutaminase (anti-tTG) antibodies. The research team set out to determine the usefulness of newer assays incorporating synthetic deamidated gliadin-related peptides (DGPs), or other TG isoenzymes as antigen, for detecting gluten sensitivity in IgA anti-tTG–seronegative patients. The team tested blood samples drawn at diagnosis from 12 anti-tTG–seronegative patients with a celiac-like enteropathy, from 26 patients with skin biopsy–proven dermatitis herpetiformis (DH) and, lastly, from 26 patients with IgA anti-tTG–positive celiac disease. All patients showed typical levels of total IgA. On each patient, the team conducted intestinal biopsy and serum testing for detection of IgA and IgG isotypes of both anti-DGP and anti-tTG in a single assay (tTG/DGP Screen; INOVA Diagnostics). They also tested each patient for simultaneous detection of both IgA and IgG anti-DGP antibody isotypes (DGP Dual; INOVA Diagnostics). Lastly, they tested each patient for the detection of antibodies to transglutaminase 3 (TG3) or transglutaminase 6 (TG6). All patients who showed positive anti-tTG results also tested positive in anti-DGP assays. The tTG/DGP Screen caught six of the 19 anti-tTG seronegatives (31.6%), while anti-DGP Dual produced caught five of these cases (26.3%). Whereas both assays detected 2 anti-tTG–negative DH patients with partial villous atrophy, they were positive in only 2 of the 5 cases with no histologically discernible mucosal damage. Testing for antibodies to TG3 and TG6 caught seven of the 19 anti-tTG–negative patients (36.8%), five of whom also tested positive for anti-DGP. From these results, the team concludes that using tTG/DGP Screen, or anti-DGP Dual, to detect anti-DGP improves diagnostic sensitivity of gluten sensitive patients with non–IgA- deficiency, or anti-tTG–seronegativity, and celiac-like enteropathy. The same enhancement is also achieved by detecting antibodies to other TG isoenzymes. Source: Clinical Chemistry 56: 661-665, 2010.
- 1 comment
-
- among
- anti–tissue
- (and 9 more)
-
Vijay Kumar, M.D., Research Associate Professor at the University of Buffalo and President and Director of IMMCO Diagnostics: The three serological tests that are used for diagnosing celiac disease are: Anti-endomysial antibody (EMA) Anti-reticulin antibody (ARA) Anti-gliadin antibody (AGA) Each of these three tests provide a certain degree of reliability for diagnosing celiac disease. Of these, endomysial antibody is the most specific test. The following table is taken from our studies (Lerner, Kumar, Iancu, Immunological diagnosis of childhood coeliac disease: comparison between antigliadin, antireticulin and antiendomysial antibodies). % of Sensitivity % of Specificity Predictive Value % Pos Predictive Value % Neg EMA 97% 98% 97% 98% ARA 65% 100% 100% 72% IgG AGA 88% 92% 88% 92% IgA AGA 52% 94% 87% 74% The following definitions related to sensitivity, specificity, positive and negative predictive values may help: Sensitivity is the probability of a positive test result in a patient with disease. Specificity is the probability of negative test result in a patient without disease. Positive predictive value is the probability of disease in a patient with positive test result. Negative predictive value is the probability of no disease in a patient with negative test result. Karoly Horvath, M.D., Ph.D., Associate Professor of Pediatrics; Director, Peds GI & Nutrition Laboratory; University of Maryland at Baltimore: The summary below shows the results of the main serological tests based on several publications including 388 patients with celiac disease, and 771 healthy subjects. SENSITIVITY- the proportion of subjects with the disease who have a positive test. It indicates how good a test is at identifying the diseased: Percentage of - IgA AGA Percentage of - IgG AGA Percentage of - IgA EMA Average 78% 79% 97% Range 46-100% 57-94% 89-100% SPECIFICITY- the proportion of subjects without the disease who have a negative test. It indicates how good a test is at identifying the non-diseased: Percentage of - IgA AGA Percentage of - IgG AGA Percentage of - IgA EMA Average 92% 84% 98.5% Range 84-100% 52-98% 97-100% POSITIVE PREDICTIVE VALUE- the probability that a person with positive results actually has the disease: Percentage of - IgA AGA Percentage of - IgG AGA Percentage of - IgA EMA Average 72% 57% 92% Range 45-100% 42-76% 91-94% NEGATIVE PREDICTIVE VALUE- the probability that a person with negative results does not have the disease: Percentage of - IgA AGA Percentage of - IgG AGA Percentage of - IgA EMA Average 94% 94% 100% Range 89-100% 83-99% 100% References: McMillan SA, Haughton DJ, Biggart JD, Edgar JD, Porter KG, McNeill TA. Predictive value for coeliac disease of antibodies to gliadin, endomysium, and jejunum in patients attending for jejunal biopsy. Brit Med J 1991;303:1163-1165 Ferreira M, Lloyd Davies S, Butler M, Scott D, Clark M, Kumar P. Endomysial antibody: is it the best screening test for coeliac disease? Gut 1992;33:1633-1637. Khoshoo V, Bhan MK, Puri S, Jain R, Jayashree S, Bhatnagar S, Kumar R, Stintzing G. Serum antigliadin antibody profile in childhood protracted diarrhea due to coeliac disease and other causes in a developing country. Scand J Gastroenterol 1989;24:1212-1216. Chan KN, Phillips AD, Mirakian R, Walker-Smith JA. Endomysial antibody screening in children. J Pediatr Gastroenterol Nutr 1994;18:316-320. Bode S, Weile B, Krasilnikoff PA, Gdmand-Hyer E. The diagnostic value of the gliadin antibody testing celiac disease in children: a prospective study. J Pediatr Gastroenterol Nutr 1993;17:260-264. Calabuig M, Torregosa R, Polo P, Tom s C, Alvarez V, Garcia-Vila A, Brines J, Vilar P, Farr C, Varea V. Serological markers and celiac disease: a new diagnostic approach ? J Pediatr Gastroenterol Nutr 1990;10:435-442.
-
Dig Dis Sci. 2004 Apr;49(4):546-50 Celiac.com 08/27/2004 – Dr. Peter Green and colleagues at the Department of Medicine, Columbia University College of Physicians and Surgeons, New York, New York, conducted a study designed to determine the sensitivity of the various serological tests used to diagnose celiac disease. To do this they looked at 115 adults with biopsy-proven celiac disease who fulfilled strict criteria which included serological testing at the time of their diagnosis, and a positive response to a gluten-free diet. Out of those studied, 71% had total villous atrophy, and 29% had partial villous atrophy. Serological results indicated that only 77% of those with total and 33% of those with partial villous atrophy actually tested positive for celiac disease, and it did not matter whether the patients presented with classical or silent symptoms. All patients who were positive for anti-tissue transglutaminase had total villous atrophy. The researchers conclude: Seronegative celiac disease occurs. Endomysial antibody positivity correlates with more severe villous atrophy and not mode of presentation of celiac disease. Serologic tests, in clinical practice, lack the sensitivity reported in the literature.
-
Vijay Kumar, M.D., Research Associate Professor at the University of Buffalo and President and Director of IMMCO Diagnostics: If the test is negative and there is a strong suspicion of celiac disease, it must be repeated after several weeks (3-4 weeks), especially after a high gluten intake. We did a study of two cases with DH who were serologically negative. However, a gluten challenge 1g/Kg body wt/day resulted in positive serology; the results became normal on a gluten free diet. If you are a relative of a celiac disease patient and are on a regular diet and the serology performed by an experienced laboratory is negative then there may not be any need for retesting until and unless clinically justified. Karoly Horvath, M.D., Ph.D., Associate Professor of Pediatrics; Director, Peds GI & Nutrition Laboratory; University of Maryland at Baltimore: There is no rule for it. If a family member with previous negative tests experiences any gastrointestinal symptoms associated with celiac disease, he/she should undergo serological testing as soon as possible. It is well known that up to 15% of the family members of a patient with celiac disease may have the asymptomatic (latent or silent) form of celiac disease, although they have positive serological tests and have the pathological changes in the upper part of the small intestine. It is also evident that there are at least three developmental stages of mucosal lesions (Marsh MN. Gastroenterology 1992;102:330-354) and celiac disease may manifest at each period of life. That is why we recommend a repeat test every 2-3 years in first degree relatives of celiac patients.
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8-M):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8-M):









.webp.5cf0e450131b7d3b603652520875971f.webp)