-
Welcome to Celiac.com!
You have found your celiac tribe! Join us and ask questions in our forum, share your story, and connect with others.
-
Celiac.com Sponsor (A1):
Celiac.com Sponsor (A1-M):
-
Get Celiac.com Updates:Support Celiac.com!
Search the Community
Showing results for tags 'prescriptions'.
-
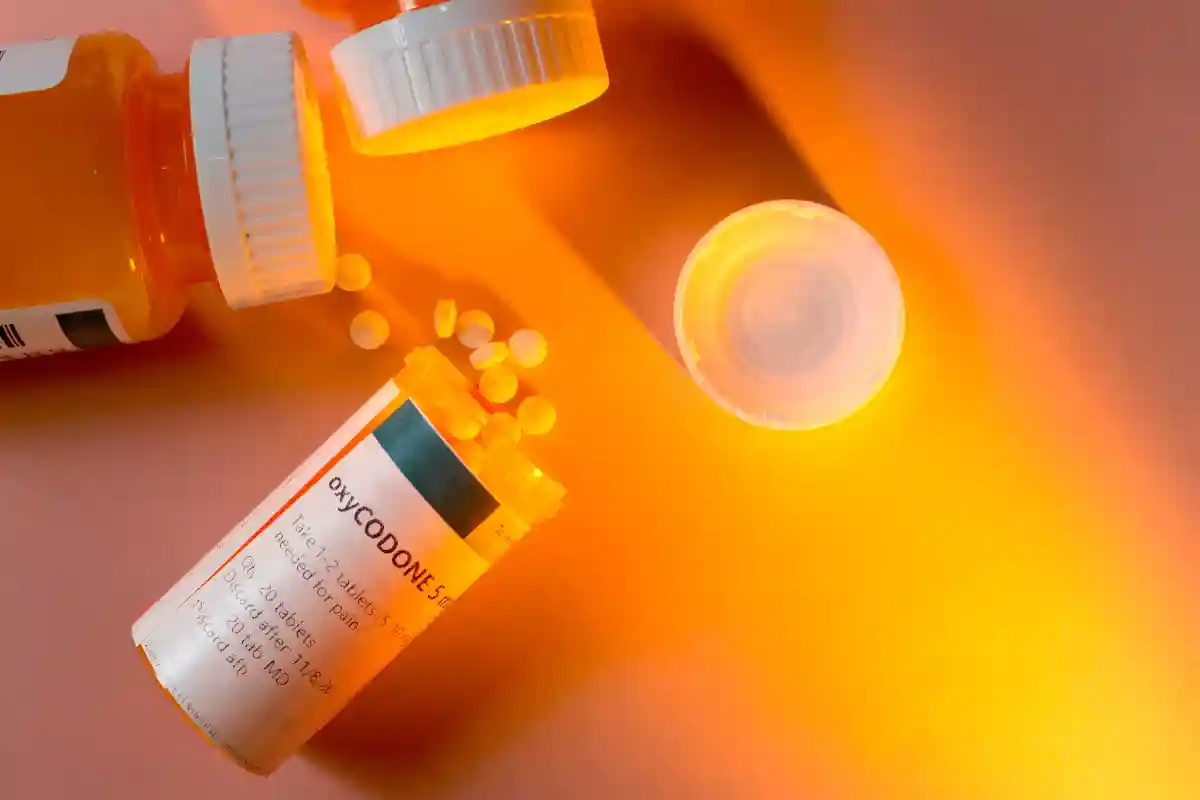
Celiac.com 01/27/2024 - We've done many articles that cover nutrient deficiencies that are associated with untreated celiac disease, but many people do not realize that celiac disease can also lead to malabsorption of medications and supplements. Celiac disease damages the lining of the small intestine, where both nutrient and certain medication absorption takes place. This damage can result in decreased absorption of various substances, including both over the counter and prescription medications, and supplements. Medications that are taken orally and absorbed in the small intestine may be affected by malabsorption in individuals with untreated celiac disease. As a result, the effectiveness of these medications might be compromised. It's essential for individuals with celiac disease to maintain a strict gluten-free diet to allow the small intestine to heal and improve nutrient absorption, including medications. Common Medications Affected by Celiac Disease Malabsorption Here are some common medications that may be affected by celiac disease-related malabsorption, but many more medications might also be affected: Thyroid Medications: Medications used to treat thyroid disorders, such as levothyroxine, may have reduced absorption in individuals with untreated celiac disease. Certain Antibiotics: Some antibiotics, including tetracycline and doxycycline, are absorbed in the small intestine. Malabsorption issues may affect their effectiveness. Anti-Inflammatory Drugs: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen, commonly used for pain and inflammation, may have altered absorption in individuals with celiac disease. Certain Anticonvulsants: Medications used to treat seizures, such as phenytoin, might be impacted by malabsorption in untreated celiac disease. Oral Contraceptives: Birth control pills, which are taken orally, may be affected by malabsorption in individuals with celiac disease. Blood Pressure Medications: Calcium Channel Blockers: Medications like amlodipine, which are calcium channel blockers used to treat high blood pressure, may be affected by impaired calcium absorption. Beta-Blockers: Some beta-blockers, such as metoprolol, may have altered absorption due to malabsorption issues. Cholesterol-Lowering Medications: Statins: Medications like atorvastatin and simvastatin, commonly prescribed for managing cholesterol levels, might be impacted by malabsorption in the small intestine. Pain Medications: Opioids: Medications containing opioids, such as codeine or oxycodone, may have absorption challenges in individuals with untreated celiac disease. Diabetes Medications: Metformin: This common medication for managing diabetes may be affected by impaired absorption in individuals with celiac disease. It's important to note that individual responses to medication can vary, and the severity of malabsorption can differ among those with celiac disease. Therefore, open communication with healthcare providers is crucial to monitor medication effectiveness, adjust dosages when needed, and explore alternative treatments if necessary. Common Supplements Affected by Celiac Disease Malabsorption Here are some common supplements that may be affected by celiac disease-related malabsorption, but many more supplements might also be affected: Calcium Supplements: Calcium carbonate or citrate: Individuals with celiac disease may experience difficulty absorbing calcium, impacting bone health. Supplementing with calcium is common to address potential deficiencies. Iron Supplements: Iron sulfate or ferrous fumarate: Celiac disease can lead to iron deficiency anemia due to impaired iron absorption. Iron supplements are often recommended to address low iron levels. Vitamin D Supplements: Cholecalciferol (Vitamin D3): Malabsorption of fat-soluble vitamins, including vitamin D, can occur in celiac disease. Supplementation is often necessary to maintain adequate vitamin D levels. B Vitamins: B12 (Methylcobalamin): Deficiencies in B vitamins, particularly B12, may occur in individuals with celiac disease due to malabsorption. B12 supplements can be prescribed to address deficiencies. Folate (Folic Acid or Methylfolate): Methylfolate: Similar to B12, folic acid absorption may be compromised. Supplementing with methylfolate can be considered. Zinc Supplements: Zinc citrate or picolinate: Zinc absorption may be reduced in celiac disease. Zinc supplementation is recommended for those with zinc deficiencies. Magnesium Supplements: Magnesium citrate or glycinate: Malabsorption issues can affect magnesium levels. Supplementing with magnesium is common to address deficiencies. Omega-3 Fatty Acids: Fish Oil (EPA and DHA): Essential fatty acids may be poorly absorbed. Omega-3 supplements can help maintain a balance of these crucial fats. Summary Individuals with untreated celiac disease may experience malabsorption of various medications and supplements due to damage to the small intestine's lining. This can impact the absorption and effectiveness of certain drugs and supplements that are commonly taken or prescribed for various conditions. It's essential for individuals with celiac disease to be aware of potential interactions and work closely with their healthcare providers, including pharmacists, to ensure appropriate adjustments in medication dosage or explore alternative forms of administration when necessary.
- 5 comments
-
- absorption
- celiac disease
- (and 6 more)
-

Gluten-Free Prescription Medications and Dietary Supplements
Sarah Curcio posted an article in Autumn 2021 Issue
Celiac.com 11/30/2021 - We all know symptoms of celiac disease are activated by the consumption of gluten, which can be found in wheat, barley, rye, and even oats that aren’t certified gluten-free. Most individuals who go on a gluten-free diet will think about food only, not necessarily medications. However, the truth of the matter is you need to be careful with both nutritional supplements, and over-the-counter and prescription medications, as they could contain gluten. More often than not, excipients, which are binding agents or inactive ingredients in pills, tend to contain wheat, potato, corn, or rice. Additionally, even if a brand name drug is gluten-free, this does not mean that its generic version is. Nutritional supplements tend to be easier because a lot of companies now label their bottles "gluten-free", or list all ingredients used in them on the packaging. For supplements that are not clearly labelled, checking the product on their company Web site is the best way to be sure, and sometimes you may need to call the manufacturer directly. Currently, however, prescriptions don't include "gluten-free" on their labels, and, unlike foods, are also not required to list any of the top eight common food allergens that they might contain. If you know your pharmacist well, they might be able to assist you, or you could reach out directly to the manufacturer. Another option is the Dailymed Web site which allows you to search for most prescription medications, including their generic equivalents, to find out what inactive ingredients are used to make them. Search for inactive ingredients and allergens contained in prescription medications: https://dailymed.nlm.nih.gov/dailymed/ Below are some potential suspect inactive ingredients that could contain gluten if their source is not specified: Modified starch Pregelatinized starch Pregelatinized modified starch Dextrates Dextrin Dextrimaltose Caramel coloring So, the next time you have to refill a prescription keep this information handy. That way, you protect your villi from further damage. Reference: beyondceliac.org- 6 comments
-
- gluten-free
- inactive
- (and 7 more)
-
Celiac.com 01/06/2020 - National charity Coeliac UK is opposing the further proposed cuts to gluten-free prescriptions for many patients in Buckinghamshire, which they say goes against the Government’s decision to maintain this essential support for all patients with celiac disease. For those unfamiliar with the British system of getting gluten-free food to people with celiac and other gluten sensitivities, the system works by providing prescriptions for gluten-free bread and flour mixes. Citing recent trends toward more readily available gluten-free foods in general, there has been a push by some in UK government to eliminate food prescriptions, which are currently handled as part of the NHS, the UK's famous health program. The charity points to a recent effort by the NHS Buckinghamshire Clinical Commissioning Group (CCG) to include people who would not be affected by any policy change in their survey of views on the matter of eliminating access to gluten-free bread and flour mix currently available on prescription. The charity fears that allowing people with no actual stake in the matter to comment, including those who don't understand why people need gluten-free food, or who see gluten-free food as a lifestyle choice, rather than a medical necessity, will skew the debate and the result. The charity's concern is that cuts to gluten-free prescriptions may leave some celiac patients without access to the gluten-free food they need to maintain their diet, which is medically necessary to treat celiac disease. The charity has encouraged all those affected to complete an online survey so that their opinions are heard. Although the survey is now closed, the responses to it will be published on February 10, 2020. What do you think? Should people who don't have celiac disease or gluten-intolerance have a say in the debate over access to gluten-free food? Share your thought in the comments below. Read more at bucksherald.co.uk
- 8 comments
-
- coeliac uk
- gluten-free
-
(and 4 more)
Tagged with:
-
Celiac.com 03/28/2020 - Were you thinking that there wasn't much gluten in your medicine? Had you read that less than 1% of drugs were made with it? Think again, because while pharmaceutical manufacturers don't actually add gluten to drugs in most instances, they very frequently cannot say that their products are gluten free. That's because before some ingredients get into a manufacturing facility, they are purchased from suppliers that are not controlled by the drug maker. Let me explain. When you take a drug, most of what you are swallowing is filler. This is called an excipient in the trade. Excipients are inert stuff that the actual drug is mixed with, and it influences the rate the drug enters your blood. For people with celiac disease, the problem is that the excipient is often made from starches derived from corn, rice, tapioca, etc. If you're reading this, you probably just recognized how gluten could be getting into your medicine even when a drug maker did not intentionally use gluten as the excipient. Drug companies affirm that even when they have not added gluten to a particular drug, there could be gluten in that drug, and they won't say the drug is gluten free. Here is where Sister Jeanne Patricia Crowe Pharm.D. (no relation to the actor) comes into the picture. About ten years ago Sister Jeanne Patricia did a study which established just how much trouble drug makers had even knowing when there was gluten in their products. Working with her research partner Nancy Patin Falini M.A., R.D., Crowe sent out questionnaires to about 170 drug makers asking each what the gluten content of their medicine was. Their results were published in the American Journal of Health-System Pharmacy in 2001 (1). In their peer reviewed article titled Gluten in Pharmaceutical Products, the two researchers were able to conclude the following: Only 5 of 100 pharmaceutical companies that responded to a survey reported having a policy of producing gluten-free products. Many companies believed their products were gluten-free but could not guarantee it. But what Crowe and Falini's results also showed was that drug makers themselves had a hard time making sure that when they bought an ingredient from an outside supplier, that they were not letting gluten get into their manufacturing facility. Two other studies support the Crowe and Falini findings, so they are pretty convincing. Simply put, gluten can be making its way into your drugs, and you can't find out about it because the drug manufacturer also doesn't know it's there. And if the drug maker doesn't know, then when your pharmacist helps you to read the package insert, it really won't matter much what it says on the label. This chaotic situation is not acceptable for the manufacture of medication. At the least, a company that makes drugs needs to determine whether they are making their product with an excipient like corn starch, and whether that the corn starch is gluten-free. Either the excipient is gluten-free or it isn't. Even when a consumer goes to buy a gluten-free food like Cheese Curls, the manufacturer at least has a letter from its raw ingredient suppliers, stating that the ingredients are gluten-free. Some food makers will even test every batch of raw ingredient before it enters their own facility. It isn't too much to ask that drug makers learn what's in their products. The FDA is currently looking at how to address the issue of gluten in medications. One approach is to require that drug makers disclose when a particular drug is gluten-free. At the other extreme, as a petitioner, I have argued that because gluten is toxic, the law of the United States should be satisfied, and gluten should be taken off the list of allowed excipients. But the work of Sister Crowe and Nancy Falini has demonstrated just why the FDA must take a step back and first require drug makers themselves to know exactly what's inside that pill or capsule. I hope that I've gotten at least a few of you wound up. I'm a bit surprised that drug makers would put themselves in a position where they sometimes don't know what's in any given pill they make. Don't they see the liability issues? Where are their lawyers, anyway? In the first article I wrote for celiac.com, I asked readers to let the FDA know that they wanted to get gluten out of drugs, and many people did exactly that. And those comments do get read. Now I am going to make sure that the FDA takes into account the work of Sister Crowe and Nancy Falini. Tell the FDA what you think. Maybe next time you fill a prescription for whatever ails you, it will be possible for you and your pharmacist to determine whether gluten is present in your medication. Michael Weber lives in New York and can still remember what pizza tastes like. References: 1. Crowe, JP, Falini, NP Gluten in pharmaceutical products Am J Health Syst Pharm 2001 58: 396-401
- 3 comments
-
- drugs
- gluen-free
-
(and 5 more)
Tagged with:
-
EMAIL YOUR US REPRESENTATIVE TODAY IN SUPPORT OF THE GLUTEN IN MEDICINE DISCLOSURE ACT OF 2019 Please personalize the sample letter pasted below. Email this letter to your local representative. A state-by-state directory is available at: https://www.house.gov/representatives?fbclid=IwAR3eNMLYkKJCJ52NLkbcZ7wqwGf9NafcHq-p9ydg7RZpvFNuz5ezQhhSv5I Here's a link to the bill: https://www.congress.gov/bill/116th-congress/house-bill/2074/all-info#cosponsors-content Sample letter: Cosponsor H.R. 2074: The Gluten in Medicine Disclosure Act of 2019 Dear [Name of your representative]: According to the Mayo Clinic, the rate of celiac disease has almost quadrupled over the past 50 years. Celiac disease is a serious, genetic autoimmune disorder in which ingesting gluten causes damage to the villi of the small intestine. It affects nearly 3 million people in the United States. In comparison, Alzheimer’s disease affects approximately 2 million people. The only treatment is the total elimination of gluten-containing products, including wheat, barley, and rye sources. For some, failure to avoid these can lead to life-threatening complications. Currently, this is nearly impossible to determine the presence of gluten in prescription medicine. In 2004, the Food Allergen Labeling Consumer Protection Act required packaged food labels to identify all ingredients containing wheat and other allergens. This requirement does not extend to prescription drugs. After repeated efforts to shed light on this issue, the FDA released draft guidance in 2017 encouraging drug manufacturers to disclose the presence of gluten. While some manufacturers have taken this step, it has not been implemented consistently. This leads to anxiety of not knowing whether or not your medicine is causing more harm than good. That is why Representatives Tim Ryan and Tom Cole introduced the Gluten in Medicine Disclosure Act, which will make it easier to identify gluten in prescription drugs. This legislation would require drug manufacturers to label medications intended for human use with the list of ingredients, their source, and whether gluten is present. A gluten-containing drug that does not meet these requirements would be considered misbranded under Section 502 of the Federal Food, Drug, and Cosmetic Act. This labeling will allow concerned consumers to know, for example, if the starch in their prescription drugs comes from wheat or corn. For the nearly 3 million Americans living with celiac disease, that small distinction is an important one. Please join other members in cosponsoring this important piece of legislation to make it easier and safer for individuals with celiac disease or gluten sensitivity to make informed purchases of needed medications. For more information or to cosponsor, please contact Rachel Jenkins (rachel.jenkins@mail.house.gov) in Congressman Ryan’s Office or Shane Hand (shane.hand@mail.house.gov) in Congressman Cole’s Office. Sincerely,
-
Celiac.com 08/22/2018 - There’s been some data to support the idea that local pharmacists might have an important role to play in helping people with celiac disease to remain gluten-free by providing information about possible gluten in drugs, and even liaising with manufacturers for gluten information on the patient’s behalf, as needed. But how solid is your local pharmacist when it comes to celiac disease awareness? A team of researchers recently set out to evaluate pharmacists' knowledge of celiac disease, and to look for areas where further information may be beneficial. The research team included Carmela Avena-Woods, PharmD, BS Pharm; Robert A. Mangione, EdD; and Wenchen Kenneth Wu, PhD, MBA. They are all with St. John's University in Queens, New York. To gather data for their evaluation, their team sent a survey to community pharmacists who practice in a national chain pharmacy in one region of New Jersey and New York. A total of 418 pharmacists, just under 40%, responded to the survey. Sixty percent of the responses correctly noted that there are currently no federal regulations requiring manufacturers to designate medications as gluten-free. Still, forty percent got that wrong. Perhaps most alarmingly, of the pharmacists who claimed a basic or advanced understanding of celiac disease, only 27% correctly indicated that celiac disease is both an autoimmune and a chronic lifelong disease. Interestingly, twenty percent of pharmacists said they often suggested a change of diet to people with suspected celiac disease before a clinical diagnosis was made. This study suggests that community pharmacists have some understanding of celiac disease, but that additional celiac education is advisable if they are to play an integral role in helping people with celiac disease to maintain a gluten-free diet. Read more at: Am J Pharm Educ. 2018;82(2)
- 2 comments
-
- celiac
- celiac disease
-
(and 6 more)
Tagged with:
-
Celiac.com 05/24/2018 - England is facing some hard questions about gluten-free food prescriptions for people with celiac disease. Under England’s National Health Plan, people with celiac disease are eligible for gluten-free foods as part of their medical treatment. The latest research shows that prescription practice for gluten-free foods varies widely, and often seems independent of medical factors. This news has put those prescribing practices under scrutiny. "Gluten free prescribing is clearly in a state of flux at the moment, with an apparent rapid reduction in prescribing nationally," say the researchers. Their data analysis revealed that after a steady increase in prescriptions between 1998 and 2010, the prescription rate for gluten free foods has both fallen, and become more variable, in recent years. Not only is there tremendous variation in gluten free prescribing, say the researchers, “this variation appears to exist largely without good reason…” Worse still, the research showed that those living in the most deprived areas of the country are the least likely to be prescribed gluten-free products, possibly due to a lower rate of celiac diagnosis in disadvantaged groups, say the researchers. But following a public consultation, the government decided earlier this year to restrict the range of gluten free products rather than banning them outright. As research data pile up and gluten-free food becomes cheaper and more ubiquitous, look for more changes to England’s gluten-free prescription program to follow. Read more about this research in the online journal BMJ Open.
- 1 comment
-
- celiac disease
- celiac treatment
- (and 4 more)
-
Celiac.com 07/20/2017 - In the face of budget cuts, and in a move that may offer a glimpse of things to come, doctors with the the UK's National Health Service are eliminating gluten-free food prescriptions for adults, beginning in parts of Devon. As of July 1, the Northern, Eastern and Western Devon Clinical Commissioning Group (CCG) responsible for planning and buying the majority of healthcare services for local people have recommended limiting gluten free foods including bread, pasta, flour and multipurpose mixes, to under 18 years of age. That means that approximately 3,400 adults in Devon will no longer receive gluten free food prescriptions, a move calculated to save tax payers around £350,000 per year. The CCG says the action is part of a plan to encourage people to purchase items that they usually get via a physician's prescription. The new guidelines were allegedly developed with input from GPs, patients and other stakeholders. The patient letter from the CCG said: "Gluten free products are now widely available from shops and online, and are often sold to the public at prices that are considerably lower than the NHS pays when they are provided on prescription. Given greater availability and lower cost, the CCG says that the move makes sense. However, many gluten-free Devon residents are offended by what they see as an attempt to pass higher costs to them. One resident, Graham Devaney, of Umberleigh, said: "I think it's absolutely disgusting. I now won't be able to eat bread because for a small loaf of gluten free bread from Sainsbury's it costs about £3, and I can't afford that because I'm disabled." Read more at devonlive.com.
-
Celiac.com 03/07/2017 - The Brits are having a bit of a dustup over the best way to help people support with celiac disease. Currently, Britain's National Health Service supplies prescriptions for gluten-free food staples for people with celiac disease. Seemingly, no one disagrees with medical experts that celiac suffers should get support from the National Health Service to buy certain staple gluten-free products. The question, at least from one side of the political spectrum, seems to be whether prescriptions are the best way to provide that support. And that question lies at the heart of the dustup. In a recent article, the British Medical Journal presents a 'head to head' case for and against gluten-free prescriptions on the NHS. In opposition to prescriptions, James Cave, a GP from Newbury, suggests an alternative would be a national voucher scheme or a personalized health budget for patients, so they receive the difference between the cost of gluten-free products and the prescription. Matthew Kurien clinical lecturer in gastroenterology, Professor David Sanders, and Sarah Sleet, Chief Executive of Coeliac UK make the case in favor of providing prescription access to gluten-free staple foods, and say that removing prescriptions unfairly discriminates against people with celiac disease. They explain "targeting gluten-free food prescriptions may reduce costs in the short term but there will be long term costs in terms of patient outcomes." They also note that there is no other example in the NHS of a disease having its treatment costs cut by 50-100 per cent. Read more at Plymouth Herald.com.
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8-M):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8):
Celiac.com Sponsor (A8-M):