Celiac.com 04/07/2026 - Celiac disease is an autoimmune condition in which eating gluten triggers inflammation and damage in the small intestine. While the intestinal effects are well known, researchers increasingly recognize that celiac disease can affect other organs as well. One area of concern is the pancreas, the organ responsible for producing digestive enzymes and regulating blood sugar.
Acute pancreatitis is a sudden inflammation of the pancreas that often causes severe upper abdominal pain and may require hospitalization. The most common causes are gallstones and heavy alcohol use, although infections, medications, and immune-related conditions can also contribute. Because both celiac disease and pancreatitis involve inflammation and immune system activity, researchers have wondered whether people with celiac disease face a higher risk of developing pancreatitis.
Celiac.com Sponsor (A12):
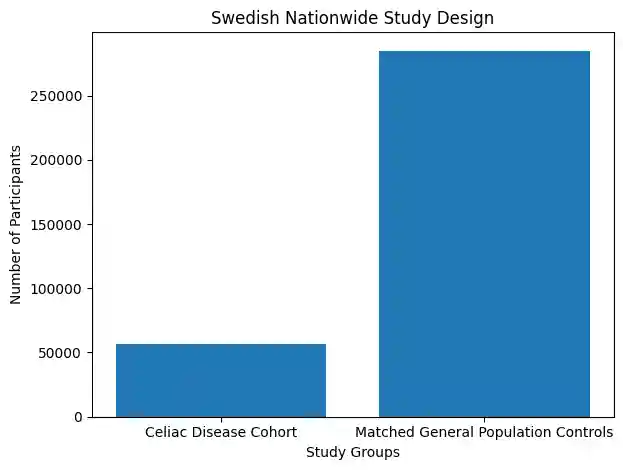
This large Swedish nationwide study examined that question in detail, following more than fifty-seven thousand people with biopsy-confirmed celiac disease for many years and comparing them to matched individuals from the general population.
How the Study Was Conducted
The researchers used national health registers in Sweden that track biopsy results, hospital admissions, diagnoses, and prescriptions. They identified over fifty-seven thousand individuals diagnosed with celiac disease between 1969 and 2023. Each person was matched with up to five people of similar age, sex, location, and calendar year who did not have celiac disease.
Participants were followed for a median of more than fifteen years. During that time, the researchers tracked new cases of acute pancreatitis. They also examined specific types of pancreatitis, including cases related to gallstones, cases not related to gallstones, cases associated with heavy alcohol use, and severe attacks requiring prolonged hospitalization or resulting in complications. In addition, they evaluated whether people who experienced one episode of pancreatitis were more likely to have repeated episodes.
A Moderate but Persistent Increase in Risk
Over the follow-up period, people with celiac disease were more likely to develop a first episode of acute pancreatitis compared to those without celiac disease. In absolute terms, the difference was modest. However, the relative risk was approximately forty percent higher overall.
The increased risk was most noticeable shortly after diagnosis of celiac disease but remained elevated for more than twenty-five years. When the researchers calculated long-term impact, they estimated that for every one hundred eighty-five people with celiac disease followed over twenty-five years, there would be one additional case of acute pancreatitis compared to the general population.
Although this represents a statistically meaningful difference, it is important to understand that the overall likelihood of developing pancreatitis remained relatively low.
Different Causes Show Different Patterns
When researchers separated pancreatitis by cause, interesting patterns emerged. Both gallstone-related and non-gallstone-related pancreatitis were more common in individuals with celiac disease. However, alcohol-related pancreatitis was not significantly increased.
Non-gallstone-related pancreatitis showed the strongest association early after celiac diagnosis, then gradually declined over time. In contrast, gallstone-related pancreatitis became more prominent several years after diagnosis and remained elevated in the long term.
Severe cases of pancreatitis were also more common in people with celiac disease. These severe episodes included prolonged hospital stays, major complications, or death within ninety days of discharge. Even here, the absolute number of cases was small, but the relative risk increase was notable.
What About Recurring Pancreatitis?
One key question was whether celiac disease increases the risk of repeated attacks once someone has already experienced pancreatitis. Interestingly, the study found no clear increase in recurrent episodes among people with celiac disease who survived their first attack. In fact, recurrence rates were similar between those with and without celiac disease.
This suggests that while celiac disease may increase the chance of a first episode, it does not appear to make subsequent episodes more likely.
Does Healing the Intestine Change the Risk?
The researchers also examined whether persistent intestinal damage influenced pancreatitis risk. Among people who had follow-up biopsies after diagnosis, some showed complete or partial healing of the intestinal lining, while others continued to have villous atrophy, meaning the intestinal lining remained damaged.
Surprisingly, persistent intestinal damage did not significantly increase the risk of pancreatitis compared to those whose intestines had healed. This finding suggests that the connection between celiac disease and pancreatitis may not depend solely on ongoing visible intestinal injury.
Possible Explanations for the Link
Although this study could not prove cause and effect, researchers proposed several possible explanations for the association.
First, celiac disease may increase the likelihood of gallstone formation. Changes in digestion and hormone signaling in the small intestine could influence gallbladder movement and bile composition, which may contribute to gallstones.
Second, immune system activation and inflammation in celiac disease may make the pancreas more vulnerable to injury. Both conditions involve inflammatory signaling molecules that can amplify immune responses.
Third, certain medications sometimes used in difficult-to-treat cases of celiac disease have been linked to pancreatitis. When the researchers restricted analyses to individuals who had not received such medications, the strength of the association decreased somewhat, suggesting that treatment factors may partly contribute.
Finally, infections and changes in intestinal barrier function could also play a role, although these mechanisms require further investigation.
Strengths and Limitations
This study has several strengths. It included a very large number of participants, used biopsy-confirmed diagnoses, and followed individuals for decades. The Swedish national health registers are known for their high quality and completeness, making the findings reliable.
However, there are limitations. The study could not directly measure diet adherence, lifestyle factors such as smoking or alcohol intake in detail, or precise mechanisms linking the two conditions. Also, most participants were from Nordic countries, so results may not apply equally to populations with different genetic backgrounds.
Why This Study Matters for People with Celiac Disease
For individuals living with celiac disease, this research provides important perspective. It confirms that there is a modest but real increase in the long-term risk of developing a first episode of acute pancreatitis. However, the overall risk remains low, and most people with celiac disease will never experience pancreatitis.
The findings highlight the importance of general health measures, such as maintaining a balanced gluten-free diet, managing metabolic risk factors, limiting heavy alcohol consumption, and discussing medication risks with healthcare providers. Because symptoms of pancreatitis can overlap with abdominal discomfort sometimes seen in celiac disease, awareness may also help ensure prompt medical evaluation if severe pain develops.
Most reassuringly, the study found no evidence that celiac disease increases the likelihood of repeated pancreatitis episodes once a first event has occurred.
Conclusion
This large, long-term study shows that people with celiac disease face a moderately increased risk of developing acute pancreatitis, particularly in the years following diagnosis. The association persists over time but does not appear to increase recurrence risk. While more research is needed to clarify the biological mechanisms, these findings encourage informed monitoring and preventive care rather than alarm. For patients and clinicians alike, understanding this connection supports better long-term health planning beyond gluten avoidance alone.
Read more at: onlinelibrary.wiley.com





Recommended Comments
There are no comments to display.
Create an account or sign in to comment
You need to be a member in order to leave a comment
Create an account
Sign up for a new account in our community. It's easy!
Register a new accountSign in
Already have an account? Sign in here.
Sign In Now