
Celiac.com 10/27/2015 - In 2006, I presented a research paper called "Open Original Shared Link". At that time I was thinking about the sick children who were coming through my clinic with skin, gut and brain symptoms: that is they had eczema and itchy skin; sore tummies and constipation; and behaviour disturbances. It turned out that most of this group of children had high levels of Anti-Gliadin-Antibodies (AGA), of whom 80% got completely better when they went on a gluten-free diet. This was a landmark paper for me, and it led me to describe "Open Original Shared Link".
However, that was nearly 10 years ago! and a lot has happened since then. Perhaps most notable the publication of the consensus paper on the Open Original Shared Link. The algorithm developed to diagnose gluten sensitivity/ intolerance relies on the elimination and challenge of gluten, rather than immunologic blood tests. I have been using the AGA test in my clinic since 1989 (that is for 25 years!) and I have found it extremely useful as a diagnostic test, when it is positive. But, many people react to gluten and have negative AGA results. So I agree with the authors of the "Spectrum" paper. The basis of a gluten-sensitivity/intolerance diagnosis should be based on elimination and challenge. Importantly, prior to removing gluten from your diet, please ensure that you get the appropriate tests for celiac disease (Open Original Shared Link).
Celiac.com Sponsor (A12):
So who in the year 2015 should be suspected of having a gluten-related-illness? Well anyone who has chronic symptoms. Even if they have a diagnostic label - because they might have the wrong diagnosis. so here are the 3 steps in my gluten-free logic:
Step ONE - the premise IF:
- a) Gluten sensitivity is common: estimates show it affects over 10% of the population;
-
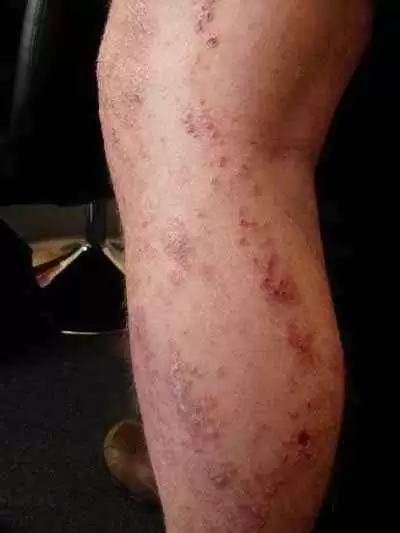
 Gluten-related illnesses are varied and have multiple symptoms: a quote from the consensus paper on the Spectrum of Gluten-Related-Disorders emphasizes this. The symptoms in gluten sensitivity may resemble those associated with celiac disease but with a prevalence of extra-intestinal symptoms, such as behavioral changes, bone or joint pain, muscle cramps, leg numbness, weight loss and chronic fatigue. Their symptoms include abdominal pain (68%); eczema and/or rash (40%); headache (35%); "foggy mind" (34%); fatigue (33%); diarrhea (33%); depression (22%); anemia (20%); numbness in the legs, arms or fingers 20%; and joint pain (11%);
Gluten-related illnesses are varied and have multiple symptoms: a quote from the consensus paper on the Spectrum of Gluten-Related-Disorders emphasizes this. The symptoms in gluten sensitivity may resemble those associated with celiac disease but with a prevalence of extra-intestinal symptoms, such as behavioral changes, bone or joint pain, muscle cramps, leg numbness, weight loss and chronic fatigue. Their symptoms include abdominal pain (68%); eczema and/or rash (40%); headache (35%); "foggy mind" (34%); fatigue (33%); diarrhea (33%); depression (22%); anemia (20%); numbness in the legs, arms or fingers 20%; and joint pain (11%); - c) There is no definitive diagnostic test for gluten sensitivity: the Consensus paper goes on to say "However, currently there are no laboratory biomarkers specific for gluten sensitivity. Usually the diagnosis is based on exclusion criteria; an elimination diet of gluten-containing foods followed by an open challenge is most often used to evaluate whether health improves with the elimination or reduction of gluten from the patient’s diet";
- d) There is no harm from going on a gluten-free diet; in other words a gluten-free is healthy.
Step TWO - The logical THEN:
Then the logical conclusion is that "anyone", with "any symptoms" that are "chronic and unexplained" (that is they do not have a definite diagnosis) and "at any time" (people can develop gluten-illness at any time in their life) should be put onto a gluten-free diet for a clinical trial for three months or more.
Step THREE - The CONCLUSION:
The logical conclusion is that whatever the blood-test results, and whatever the endoscopy results, and whatever the symptoms, a beneficial response to a gluten-free diet suggests that their illness is gluten-related (some people might demand a double blind food challenge).
Comment
Up until now, most gluten/celiac doctors have dismissed the idea that their patients might be suffering from "non-celiac gluten-sensitivity" (NCGS). They have attributed their patients beneficial response to a gluten-free diet as a placebo response (all in their head!). This is clearly not the case. There is mounting evidence for this: see this research paper - Open Original Shared Link. In this paper the authors conclude: "In a cross-over trial of subjects with suspected NCGS, the severity of overall symptoms increased significantly during 1 week of intake of small amounts of gluten, compared with placebo".
The above logic means that ALL people, with ANY undiagnosed illnesses, at any TIME in their life, should be given a gluten-free trial. This is likely to have huge health benefits and wide ramifications on the management and burden of ill health on the community. Already 10% of Australians and Canadian are adopting a gluten-free diet, and 30% percent of adults in the USA are interested in avoiding or cutting down on gluten in their diets, says a survey from the NPD Group, a consumer research firm. NDP has been following gluten-free issues since 2009 and its January 2013 survey revealed the highest interest in gluten-free diets yet (reported in HuffPost - 26 Feb 2015).
It is my prediction that in another generation most people who wish to stay healthy, will choose to adopt a gluten-free diet, before they get harmed by gluten.













.webp.9196c21eadaae0966868676eb72fb80c.webp)





Recommended Comments